Amyotrophic Lateral Sclerosis - How It Is Related To Enteroviral Infection
Amyotrophic lateral sclerosis (ALS) is a deadly neurological illness characterized by progressive degeneration of both upper and lower motor neurons, culminating in paralysis and death within three to five years of diagnosis. Despite being largely a motor neuron disease, approximately half of ALS patients have cognitive/behavioral deficits, suggesting a role for non-motor systems in ALS pathogenesis.
Author:Suleman ShahReviewer:Han JuJul 12, 2022144 Shares1.9K Views

Amyotrophic lateral sclerosis(ALS) is a deadly neurological illness characterized by progressive degeneration of both upper and lower motor neurons, culminating in paralysis and death within three to five years of diagnosis.
Despite being largely a motor neuron disease, approximately half of ALS patients have cognitive/behavioral deficits, suggesting a role for non-motor systems in ALS pathogenesis.
In Europe and North America, the general frequency of ALS is believed to be 3-5 instances per 100,000 persons, and it rises with age.
The usual age of ALS onset is between 55 and 65, with males having a larger cumulative lifetime risk (1:350) than women (1:400).
There is no cure for ALS at the moment. The only two FDA-approved medications for the treatment of ALS are riluzole (a glutamate release inhibitor) and edaravone (a free-radical scavenger).
Their advantages, however, are limited to slowing disease development and extending lifeby 2-3 months.
Over the last two decades, several different treatment strategies have been researched, but their clinical usefulness has yet to be demonstrated.
Enteroviruses And Neurological Disorders
Enteroviruses (EVs) are single, positive-stranded RNA viruses of the Picornaviridae family that include poliovirus, coxsackievirus, echovirus and enterovirus, with the latter (particularly EV-A71 and EV-D68) causing recent significant outbreaks in Asia-Pacific and North America, respectively.
EVs may induce asymptomatic infections or neurological problems. EVs have a strong tropism for the central nervous system (CNS) and cause poliomyelitis, aseptic meningitis, encephalitis, and non-polio flaccid paralysis in newborns and children.
Neurological illnesses caused by non-polio EVs have increased after polio immunization. EV-A71, echovirus, and coxsackievirus infections often cause acute flaccid paralysis. Recent epidemiological studies show a link between EV-D68 infection and acute flaccid myelitis.

Amyotrophic Lateral Sclerosis - Causes, Symptoms, Treatments & More…
Viral Infection And ALS
Viral infection has long been regarded as a risk factor for ALS and/or a causal pathogen. Many attempts have been done over the last 30 years to investigate the relationship between neurotropic viruses, particularly EVs, exogenous retroviruses such as human immunodeficiency virus and human T cell leukemia virus, and human endogenous retrovirus (HERV), and ALS.
HERVs are ancient retrovirus remnants that have been incorporated into the human genome and are generally inactive, but may be reactivated under physiological and pathological stress. Despite fruitless efforts to establish evidence of exogenous retroviruses in ALS patient tissues, multiple studies have revealed increased HERV-K gene expression and reverse transcriptase activity in ALS patients' blood and brain tissues.
Transgenic mice expressing HERV-K in neurons acquire progressive motor neuron failure comparable to the human ALS phenotype, implying a viral etiology of ALS. Additional research is being conducted to investigate the mechanism by which HERV-K produces neuropathology, as well as to evaluate current anti-retroviral medications and create new anti-HERV inhibitors for the treatment of retrovirus-associated ALS.
EV-Induced Molecular And Pathological ALS Changes
Emerging evidence from cell culture and mouse experiments shows that EV infection causes ALS-specific cellular and molecular phenotypes such as RNA-processing defects, impaired nucleocytoplasmic transport, neuroinflammation, impaired protein quality control, and, most notably, TDP-43 (transactive response DNA binding protein-43) pathology, implying a possible link between EV infection and ALS pathogenesis.
RNA-Processing Defects And TDP-43 Pathology
ALS-causing mutations have been found in multiple genes that encode RNA-binding proteins (RBPs), including TARDBP, FUS, HNRNPA1, MATR3, TAF15, and TIA1.
Mislocalization, aggregation, and cleavage of TDP-43 (TDP-43 pathology) in motor neurons and glial cells is seen in ~97% of ALS patients and is a pathological characteristic of ALS. The TARDBP-encoded DNA/RNA-binding protein TDP-43 regulates RNA metabolism.
Loss and gain-of-function in TDP-43 pathology may cause illness initiation and progression. Poliovirus, EV-A71, and coxsackievirus rely on cellular proteins for cytoplasmic reproduction.
Numerous RBPs, which are typically nucleocytoplasmic shuttling proteins confined to the nucleus, are retained in the cytoplasm during EV infection and hijacked by EVs for viral translation and RNA replication. EV-A71 infection redistributes heterogeneous nuclear ribonucleoprotein A1 from the nucleus to the cytoplasm, where it boosts EV-A71 replication by aiding viral translation.
CVB3 infection mislocalizes and cleaves TDP-43 through CVB3-encoded proteinases, causing RNA-processing deficiencies. These data imply EV infection and ALS share a mechanistic characteristic in RNA metabolism.
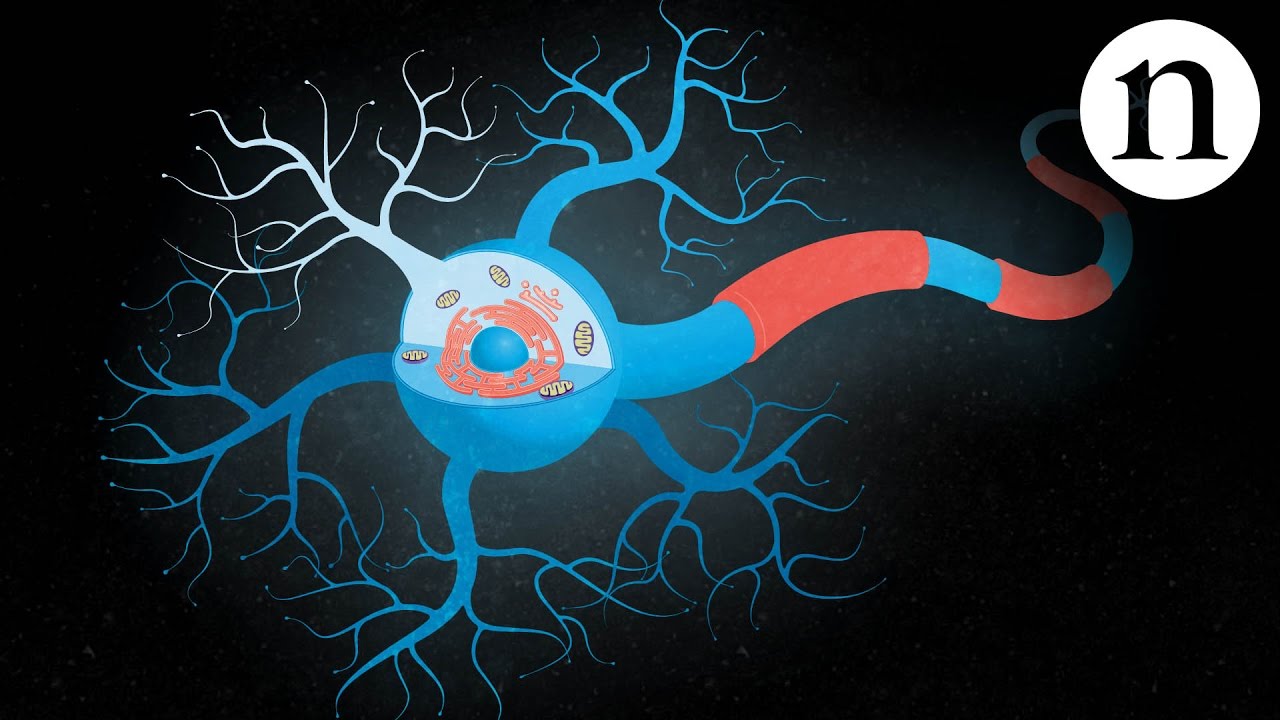
Inside ALS: The neurons behind the disease
Compromised Nucleocytoplasmic Trafficking
Defects in nucleocytoplasmic shuttling are a key issue in ALS research, leading to RBP mislocalization in the cytoplasm. Recent investigations show that the G4C2 hexanucleotide repeat expansion mutation in the first intron of chromosome 9 open reading frame 72 (C9orf72) plays a key role in nucleocytoplasmic transport failure.
C9orf72 mutations cause ~40% of FALS and 5%–10% of SALS. Expression of G4C2 repeats affects nucleocytoplasmic transport via interfering with Ran GTPase-activating protein 1 and disrupting the nuclear pore complex. EV-induced disease often involves impaired nucleocytoplasmic trafficking.
Nucleoporin (Nup) proteins Nup62, Nup98, and Nup153, important NPC components, are degraded by polio virus-encoded proteinase 2A, blocking nuclear import. EVs get access to nuclear proteins needed for viral replication and limit host immune response by blocking nuclear trafficking of anti-viral signal molecules.
A recent study that CVB3 proteinase 2A alone may promote TDP-43 accumulation suggests a probable overlap between EV and ALS.
Neuroinflammation
The role of the immune systemin the development of ALS has been extensively studied, with the majority of research focusing on the activation of glial cells and astrocytes, which leads to the up-regulation of multiple pro-inflammatory cytokines such as tumor necrosis factor-α, monocyte chemoattractant protein-1, cyclooxygenase-2, and interleukins.
Beyond direct harm, EVs may increase immune-mediated injury in viral infections by increasing the synthesis of pro-inflammatory cytokines, leukocyte infiltration, and astrogliosis. Chronic CVB3 infection has been found to cause CNS microgliosis and astrogliosis in chronically infected mice brains.
The presence of immune cells and cytokines inside the CNS may exacerbate virus-mediated neuropathology as well as possible bystander harm induced by T cell activation.
Furthermore, neuroinflammation caused by microglia and astrocytes may cause cell death by increasing the generation of reactive oxygen species. Overall, existing data suggests that persistent EV infection might cause late-onset CNS impairment by triggering inflammatory responses.
Defective Autophagy
ALS-causing mutations in genes such as SQSTM1/p62, OPTN, TBK1, VCP, and UBQLN2 are typically associated with protein quality control. Autophagy dysfunction and the subsequent buildup of misfolded proteins and large RNA clusters (e.g., RNA granules) have been linked to the etiology of ALS.
Recent research suggests that EVs may use the autophagic route to their advantage. Autophagy is a dynamic process that consists of autophagosome synthesis and destruction after fusion with a lysosome, which is referred to as autophagic flux.
The EV proteinase-mediated cleavage of synaptosomal-associated protein 29, a crucial component of the soluble N-ethylmaleimide-sensitive factor activating protein receptor (SNARE) complex necessary for autophagosome-lysosome fusion, inhibits autophagic flow.
Autophagosomes accumulate as a consequence of decreased autophagic flow and promote viral development by providing membrane scaffolding for viral assembly and replication.
Inhibiting autophagic flow also causes protein aggregation formation, which contributes to viral pathogenicity. Apart from bulk degradation, autophagy may selectively recycle misfolded proteins/damaged organelles through autophagic receptors such as sequestosome 1 (SQSTM1)/p62 and BRCA1 neighbor (Nbr1), which direct ubiquitinated proteins/organelles to autophagosomes for destruction.
EV infection causes SQSTM1 and/or Nbr1 cleavage through the proteolytic activity of EV proteinases, resulting in decreased protein aggregation clearance. The new findings implies that EVs use a unique molecular mechanism to increase viral replication and generate ALS-like viral pathogenesis.
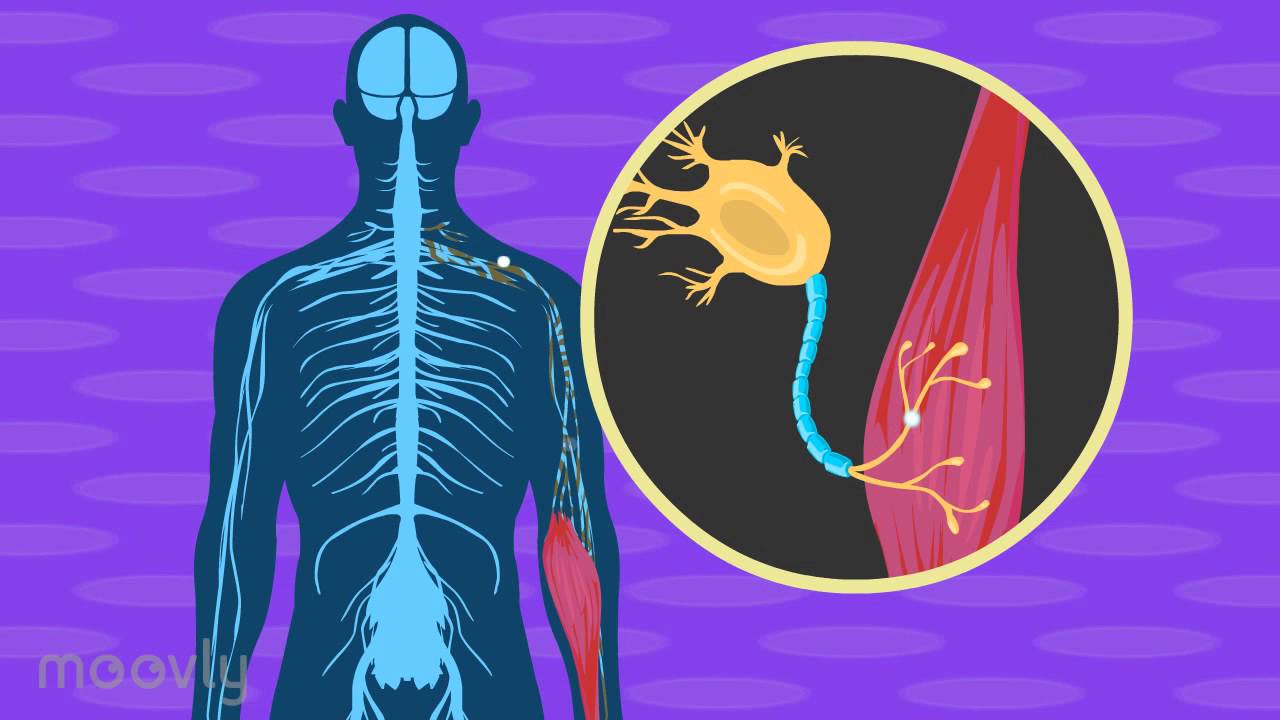
What is ALS?
Prion-Like Mechanism
ALS is known to begin focally and expand neuroanatomically to other locations. Recent research reveals that misfolded protein transmission involves both exosome-dependent and independent processes.
As non-enveloped viruses, EVs are thought to be able to escape the infected cell only by causing it to rupture. However, it has become obvious that this group of viruses, which includes poliovirus, CVB3, and EV-A71, may move across cells in a non-lytic manner through extracellular microvesicles (EMVs) such as exosomes.
As a result, EVs develop a membrane barrier that protects them from host immune recognition. Thus, EV-induced EMV secretion might be a route for the transfer of misfolded proteins (e.g., misfolded SOD1 and TDP-43) inside the CNS during chronic infection.
People Also Ask
What Is The Main Cause For Amyotrophic Lateral Sclerosis?
The etiology of ALS is unknown, and experts aren't sure why it affects some individuals but not others. Scientific data, on the other hand, reveals that both genetics and environment have a role in motor neuron degeneration and the development of ALS.
What Happens When You Have Amyotrophic Lateral Sclerosis?
Motor neurons in your brain and spinal cord die as a result of ALS. When this occurs, your brain is unable to deliver information to your muscles. Because the muscles get no impulses, they become very feeble. This is referred to as atrophy.
What Is Your Life Expectancy With Amyotrophic Lateral Sclerosis?
Although the average survival duration with ALS is two to five years, some patients survive for five, ten, or even fifteen years. Symptoms may first appear in the muscles that govern speech and swallowing, as well as in the hands, arms, legs, or feet.
Can You Survive Amyotrophic Lateral Sclerosis?
ALS is a deadly disease. After diagnosis, the typical life expectancy is two to five years, however some people may survive for years or even decades. For example, scientist Stephen Hawking lived for more than 50 years after being diagnosed.
Conclusion
Sporadic amyotrophic lateral sclerosis (SALS) is an idiopathic, terminal neurodegenerative illness of the motor neuron system for which there is now no viable therapy. For decades, an EV etiology of SALS has been hypothesized; nevertheless, human viral interrogation experiments provide contradictory data.
Emerging data suggests that EV infection causes amyotrophic lateral sclerosis-specific molecular characteristics. This result, together with previous discoveries that EVs may cause a persistent infection in the CNS, shows that chronic and persistent EV infection may be a cause/risk factor for amyotrophic lateral sclerosis.
More research is required to clearly confirm the link, such as determining if subclinical EV infection might increase the early start and progression of amyotrophic lateral sclerosis in normal animals or mice who are genetically prone to the disease.
Recent advances have increased awareness of the important clinical and genetic parallels between ALS and frontotemporal dementia(FTD).
Indeed, 13% of ALS patients also have FTD. Mutations in the same collection of genes that cause ALS, including C9ORF72, TARDBP, FUS, TIA1, and SQSTM1/p62, have also been associated with FTD. Furthermore, ALS and FTD have identical neuropathological features and disease processes. As a result, it is fair to believe that EV infection contributes to FTD.
Finally, identifying EV as an unique causal/risk factor for SALS opens up a world of possibilities for future treatment approaches. During EV infection, long after the acute infection has ended, the administration of ribavirin, a generic anti-RNA viral medication that can cross the BBB, may dramatically diminish viral-mediated neuropathology.
Furthermore, pleconaril, an anti-picornavirus medication that has been shown to traverse the BBB and limit several species of EV infection within the CNS, has been shown to cross the BBB and limit multiple species of EV infection within the CNS. As a result, it is expected that antiviral therapy will provide fresh hope for the treatment of ALS.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles