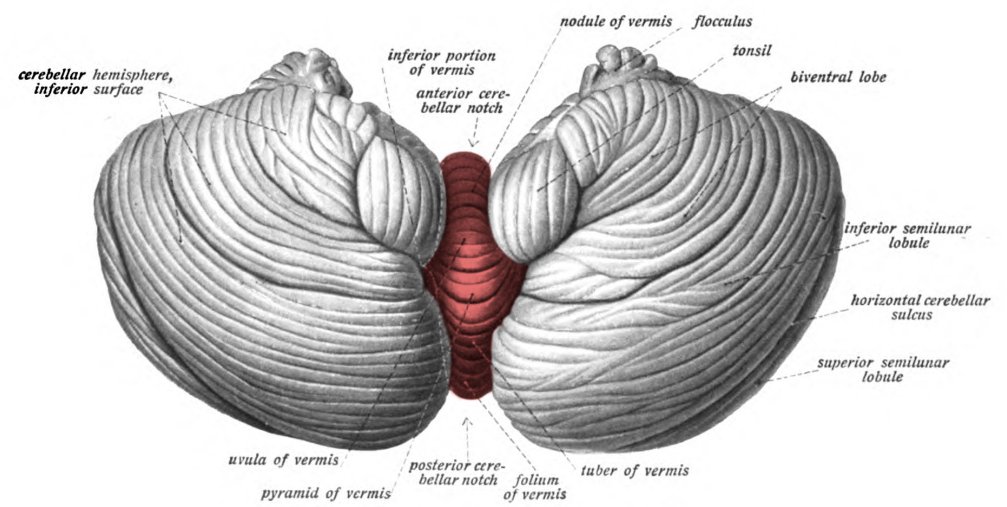
Cerebellar Tonsil - Details Of Its Gross And Neurosurgical Anatomy
The herniation of the human cerebellar tonsil through the foramen magnum, whether congenital or acquired, is well-known. 'tonsilla cerebella,''ventral paraflocculus,' 'cerebellar amygdala (almond-shaped),' and 'amygdala cerebelli' are all synonyms for the cerebellar tonsil. The tonsil is part of the cerebellar lobe's posterior region. The uvula, which is the lower half of the vermian surface's diamond-shaped formation, protrudes downward between the tonsils, simulating the oropharyngeal situation.
Author:Suleman ShahReviewer:Han JuNov 05, 2022179 Shares2.5K Views
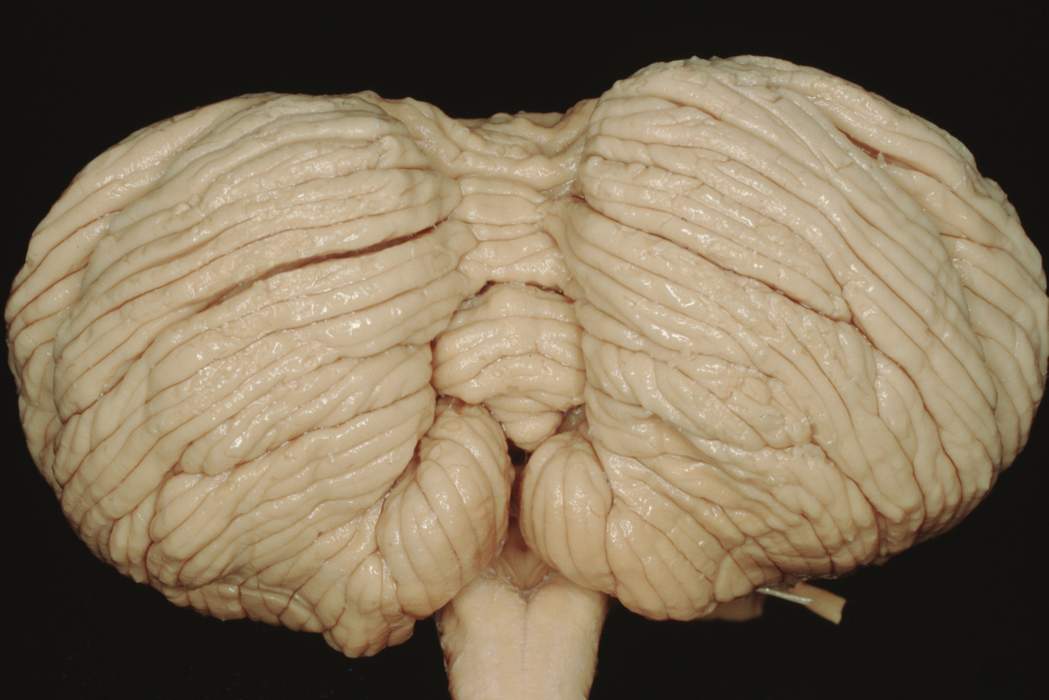
The herniation of the human cerebellar tonsilthrough the foramen magnum, whether congenital or acquired, is well-known. 'Tonsilla cerebella', 'ventral paraflocculus,' 'cerebellar amygdala (almond-shaped),' and 'amygdala cerebelli' are all synonyms for the cerebellar tonsil.
The tonsil is part of the cerebellar lobe's posterior region. The uvula, which is the lower half of the vermian surface's diamond-shaped formation, protrudes downward between the tonsils, simulating the oropharyngeal situation.
The main goal of this article is to look at the gross anatomy, morphometric characteristics, and arterial vasculature of the human cerebellar tonsil. It also aimed to gain a better understanding of the neurosurgical anatomy of this clinically important brain structure.
Gross Anatomy
The cerebellar tonsil is a rounded lobule on the undersurface of each cerebellar hemisphere, which is connected to the uvula of the cerebellar vermis on the medial side and the flocculonodular lobe on the superior side. The uvula's tapering edges are bordered by the tonsil's rostromedial margin. The tonsillar peduncle, a white matter bundle, connects this ovoid structure to the cerebellum along its superolateral border. The tonsillar surfaces that are left are uninhabitable.
The cisterna magna is faced by the inferior (caudal) pole and the posterior surface of the cerebellar tonsil. Except superiorly at the level of the tonsillar peduncle, the lateral surface of each tonsil is covered by a narrow cleft that separates it from the biventral lobule (the tonsillar biventral or post pyramidal fissure). The medial, anterior, and superior surfaces are all in contact with other neural structures, but are separated by narrow fissures.
The cerebellomedullary fissure connects the anterior surface of each tonsil to the posterior surface of the medulla. The tonsils' medial surfaces face each other across a narrow cleft in the fourth ventricle called the vallecula cerebelli. A posterior extension of the cerebellomedullary fissure, known as the telenovela tonsillar cleft, separates the superior (rostral) pole from surrounding structures.
The supratonsillar cleft refers to the cleft's superior extension over the superior pole of the tonsil. The three structures (tela choroidea, inferior medullary velum, and nodule) that make up the lower half of the roof of the fourth ventricle face the ventral aspect of the superior pole of each tonsil. The superior pole's posterior aspect faces the uvula on the medial side and the biventral lobule on the lateral side.
The tonsil is the most visible structure that prevents access to the fourth ventricle's caudal part. From the level of the nodule anterior to the tonsils to the level of the foramen of Magendie, the medial segments of the fourth ventricle's choroid plexus stretch. There are two parts to each medial segment: a rostral or nodular part and a caudal or tonsillar part. Tonsillar parts are located anterior to the tonsils and extend inferiorly through the Magendie foramen.
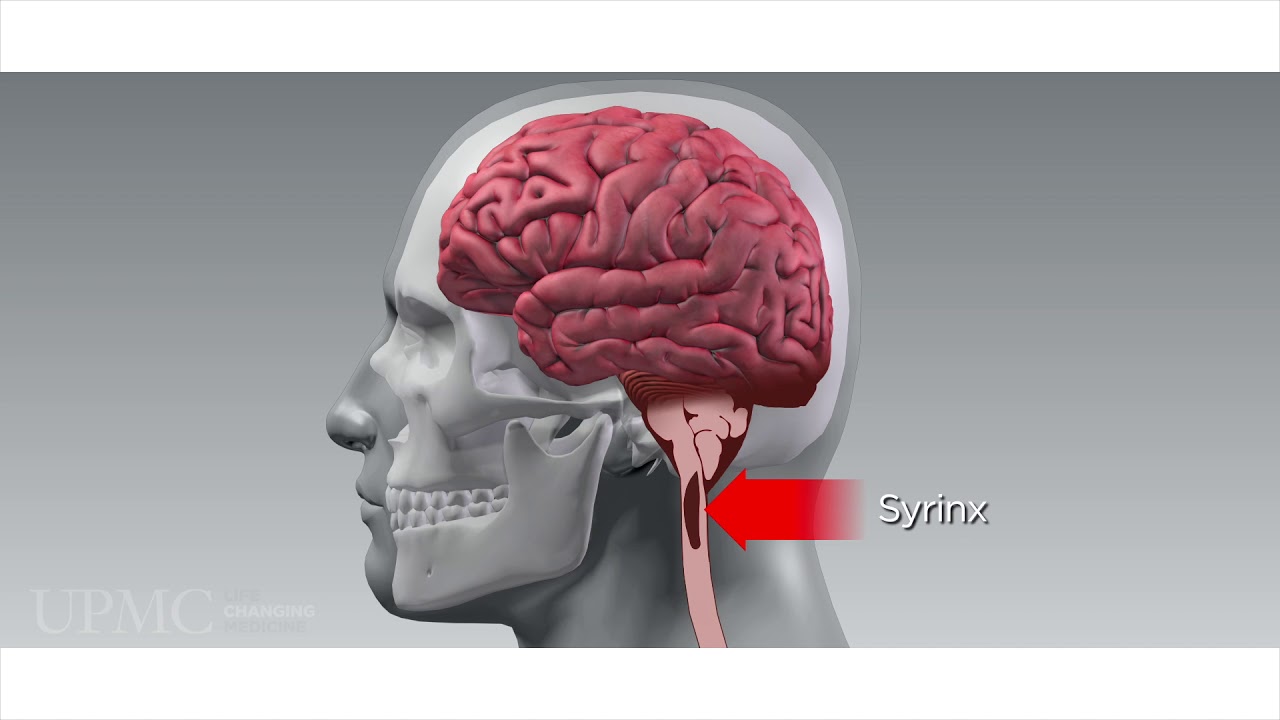
Chiari Malformation - Diagnosis and Treatment
Functional Sata
When it comes to movement coordination, the cerebellum is crucial. It receives sensory input and influences descending motor pathways in order to produce fine, smooth, and coordinated motion. The cerebellar tonsil is part of the neocerebellum (also known as the pontocerebellum), which is the largest part of the cerebellum and controls the movement of the limbs' distal parts. It receives information from the cerebral cortex and aids in motor activity planning.
The cerebellar tonsils and other cerebellar structures, which are affected in horizontal gaze-evoked nystagmus, are thought to be part of a gaze-holding neural integrator control system, according to evidence. Additionally, gaze-evoked nystagmus could be a sign of ipsilaterally located midline and lower cerebellar lesions. The cerebellum is involved in non-motor sensory, cognitive, vegetative, and affective functions, according to recent neuroimaging and neurological research. Hypercapnia and subsequent air hunger were found to activate the cerebellar tonsil, as well as other cerebellar structures.
Imaging Data
MRIs of the cerebellar hemispheres with a 5 millimeter sagittal (1.5 Tesla) resolution show several structures, including the tonsils. T1-weighted and T2-weighted sequences, which provide the greatest contrast between CSF and parenchyma, are best for identifying surface features of the hemispheres, such as deeper fissures and shallower sulci. Cerebellar disease can be identified, localized, and quantified using MRI in patients with clinical deficits.
Anatomy of the Cerebellum (3D Anatomy Tutorial) | UKMLA | CPSA
On proton-density-weighted and T2-weighted spin-echo images of 5 mm coronal (1.5 Tesla) MRIs, which provide excellent contrast between gray and white matter, the primary white matter tracts innervating several hemispheric (including tonsil) and vermian lobules are well shown. Normal and abnormal morphologic differences between the cerebellar hemispheres should be easily identified, localized, and quantified using MRI in the coronal plane.
Neurosurgical Anatomy
Increased intracranial pressure causes the cerebellar tonsils to engage in the foramen magnum, which is a well-known complication. Except in cases of posterior fossa infarcts, acute subdural haematomas, or during a lumbar puncture, tonsillar herniation is not always a fatal complication. Acute herniation is rightfully considered one of the determinants of clinical outcome in such cases. Tonsillar herniation and a smaller posterior fossa are two features of myelomeningocele, a congenital neural tube defect.
In adolescents, any inferior displacement of a tonsil below the basion-opisthion reference line should be considered abnormal. Any inferior displacement of the tonsils, or such displacement to the extent of 5 mm when it is located below the foramen magnum, is referred to as tonsillar ectopia. Tonsillar ectopia, which includes a slight descent of the cerebellar tonsils as well as Chiari type I malformation, is a common occurrence in older children and adults and is thought to be an acquired form of Chiari malformation.
Hydrocephalus plays no role in the development of this entity, unlike the other Chiari malformations. It's more than likely a paraxial mesoderm disorder, with posterior fossa hypoplasia and content overcrowding, rather than a neuroectoderm embryological anomaly. Tonsillar ectopia is a potentially treatable condition that can manifest in adulthood. In these cases, radiological contrast studies are used to make a diagnosis; it's especially important to look at the cervical canal in prone and supine positions.
Chiari type I malformation has a prevalence of less than 1% to 3%. Subjects with new-onset tonsillar ectopia due to repeated lumbar puncture, idiopathic intracranial hypotension, lumboperitoneal shunting, or spontaneous development can experience the occipital and exertional headaches associated with this malformation. With a return to normal tonsil positioning, this new-onset headache may fade. Tonsillar ectopia's clinical significance is determined by the degree of posterior fossa hypoplasia and the reduction in CSF flow velocity.
Surgery
During the transcerebellomedullary fissure approach to the fourth ventricle, the PICA's tonsillar medullary and telovelar tonsillar segments are the most important vessels encountered. In 5% of specimens, the tonsillar medullary PICA segment passed through the cerebellomedullary fissure to be placed superior to the tonsil, 17.5% at the level of the upper pole of the tonsil, 37.5% at the middle of the tonsil, and 37.5% at the lower pole of the tonsil, according to Ucerler et al. For surgery in and around the fourth ventricle, a thorough understanding of the PICA branches' relationship to the cerebellar tonsils is necessary.
For tumors of the fourth ventricle, the tonsillouveal fissure approach avoids dividing the inferior vermis. The telovelar approach (median inferior suboccipital cerebellomedullary fissure approach) takes the path to the fourth ventricle through the vallecula, with microsurgical opening of the arachnoidal layers allowing separation of the two tonsils and access to the tonsillouveal sulcus between the uvula and nodulus.
People Also Ask
What Does It Mean To Have Low-Lying Cerebellar Tonsils?
They usually occupy the entirety of the skull. The two cerebellar tonsils may descend or protrude through the skull and into the upper spinal canal in some people, rather than sitting inside the skull. A Chiari malformation (CM) is characterized by low-lying cerebellar tonsils.
Does The Cerebellum Have A Tonsil?
The cerebellum is a part of the brain in the back of the head that is located low down. The cerebellar 'tonsils' are two small areas at the bottom of it.
What Is The Consequence Of Cerebellar Tonsil Herniation?
The cerebellar tonsils can protrude several millimeters below the foramen magnum if they are herniated. The tonsils press on the brainstem and spinal cord, obstructing CSF flow and causing Chiari symptoms.
Is Cerebellar Tonsillar Life Threatening?
The movement of cerebellar tonsils through the foramen magnum causes tonsillar herniation, which is the movement of brain tissue from one intracranial compartment to another. This is a life-threatening and time-sensitive pathology that may be reversible with emergency surgery and medical management.
Conclusion
Some congenital and acquired disorders, such as Chiari malformations and raised intracranial pressure, can cause the position of the cerebellar tonsil to change. The high prevalence of single-source tonsillar arterial supply, which can be explained in part by vascular abnormalities like arterial hypoplasticity, makes this structure vulnerable to vascular accidents (primarily infarcts) of the inferior cerebellar arteries. For neurosurgical interventions in this area, a thorough understanding of regional tonsillar anatomy and its relationships to the PICA branches is critical.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles