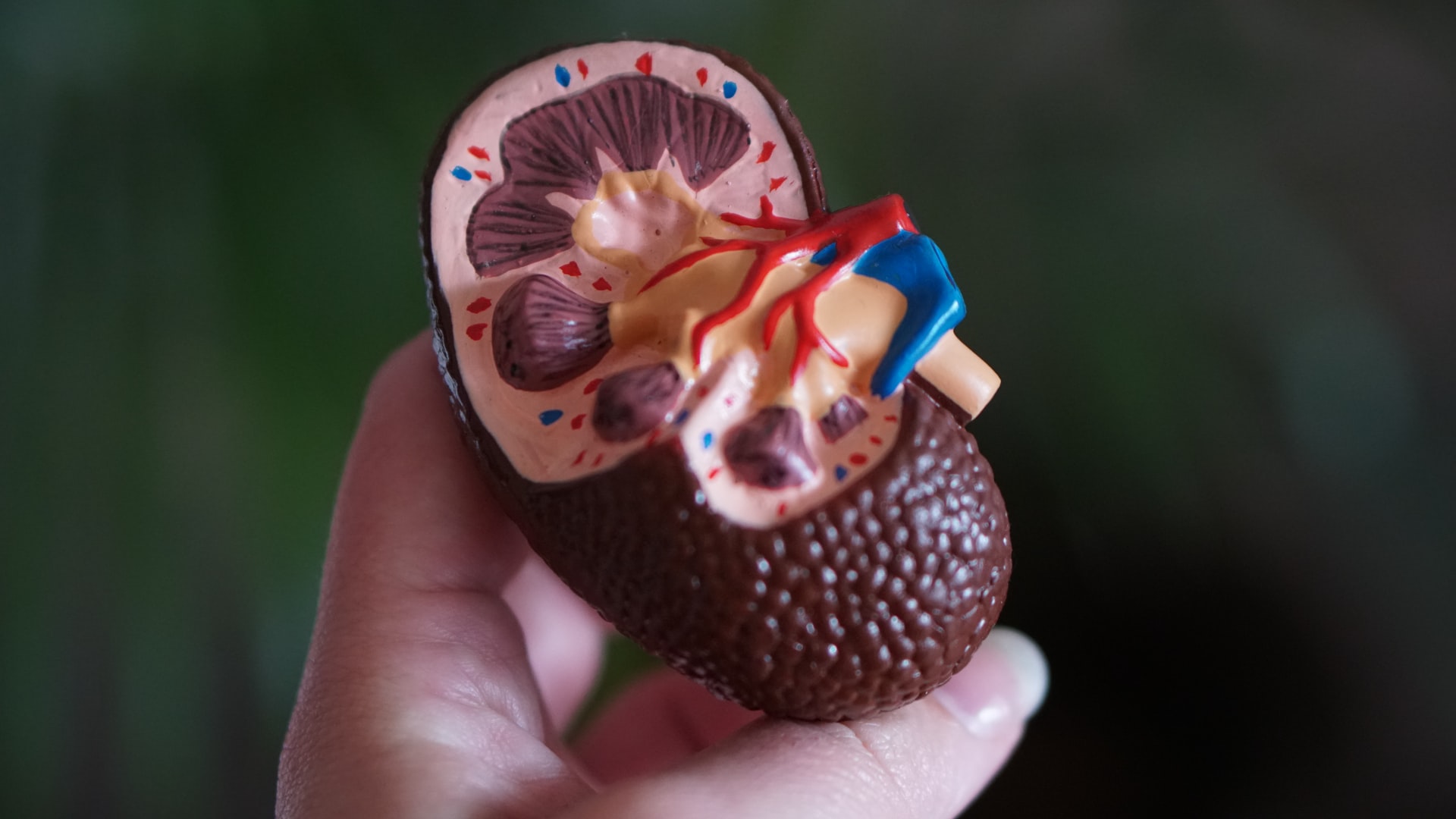
Diabetic Nephropathy - How Does It Work With Cell Apoptosis?
Apoptosis aids in the treatment of diabetic nephropathy, but the mechanism by which high glucose (HG) triggers apoptosis is still unknown. Apoptosis is involved in the causes and prevention of a variety of medical conditions. Apoptosis plays an important role in cancer prevention in humans, causing cells with damaged DNA to commit "suicide" before becoming cancerous.
Author:Suleman ShahReviewer:Han JuJul 17, 20235.5K Shares241.7K Views
Apoptosis aids in the treatment of diabetic nephropathy, but the mechanism by which high glucose (HG) triggers apoptosis is still unknown.
Apoptosis is involved in the causes and prevention of a variety of medical conditions. Apoptosis plays an important role in cancer prevention in humans, causing cells with damaged DNA to commit "suicide" before becoming cancerous.
It also plays a role in muscle atrophy, when the body decides that spending calories on maintaining muscle cells that aren't being used regularly is no longer a good idea.
What Does Apoptosis Mean?
In multicellular organisms, apoptosis is the process of programmed cell death. It is a tightly controlled and regulated process that occurs naturally during development and aging as a homeostatic mechanism to keep cell populations in tissues in check.
In a developing human embryo, for example, cells between the digits undergo apoptosis, which causes the separation of fingers and toes. Apoptosis is a defense mechanism that occurs when cells are damaged by disease or noxious agents. Cell shrinkage and pyknosis can be seen by light microscopy during the early stages of apoptosis.
The cytoplasm becomes denser as the cell shrinks, and the organelles become more compact. The most distinguishing feature of apoptosis is pyknosis, which is caused by chromatin condensation. Later in the process, apoptosis produces apoptotic bodies, which phagocytic cells engulf and remove quickly before the contents spill out onto surrounding cells, causing inflammation.
Intrinsic pathways, in which a cell receives a signal to start apoptosis from one of its own genes or proteins in response to DNA damage, and extrinsic pathways, in which a cell receives a signal to start apoptosis from other cells in the organism, are the two major types of apoptosis pathways. When an organism recognizes that a cell has outlived its utility or is no longer a good investment for the organism to support, the extrinsic pathway is activated.
The Two Apoptosis Pathways
Apoptosis can be triggered by one of two pathways:
- Intrinsic Pathway
- Extrinsic Pathway
The Extrinsic Pathway
External stimuli, such as ligand binding at cell surface death receptors, activate this pathway, which causes apoptosis. The Tumor Necrosis Factor (TNF) gene family contains these receptors. Caspases are activated when receptors bind to them.
The Intrinsic Pathway
Internal stimuli like biochemical stress, DNA damage, and a lack of growth factors trigger apoptosis through this pathway. Two groups of molecules, Bax and Bcl-2, regulate this pathway. The survival or apoptosis of a cell in response to stimuli is determined by these groups of molecules.
What Are Some Examples Of Apoptosis?
From Tadpole To Frog
Frog tadpoles are a spectacular example of this, as they destroy and re-absorb entire body structures during their transformation into frogs.
As the tadpole matures, apoptosis signals instruct cells in the gills, fins, and tail to die. These disassembled cells' raw materials are used to build new limbs and provide food for them.
The Human Nervous System Development
Huge numbers of cells die through apoptosis during the early stages of human nervous system development.
Scientists aren't sure why the developing nervous system experiences so much programmed cell death. Some speculate that this is due to the fact that forming the correct connections is a complex and potentially difficult process for young neurons, and that maximizing the nervous system's efficiency is clearly in the organism's best interests.
Mouse Feet
Mice's feet begin lifeas flat, spade-shaped things during embryonic development. The feet split into five distinct toes as development progresses, thanks to a process known as apoptosis! To create the distinct gaps between the toes, cells connecting the toes die off.
This is an example of how programmed cell death can be used to shape useful structures and create useful features while also removing those that are no longer needed.
Apoptosis And Cancer
Apoptosis is primarily used to eliminate cells that are harmful to the rest of the organism. When a cell detects that its DNA has been severely damaged, it goes into apoptosis. In these cases, DNA damage activates apoptosis pathways, preventing the cell from transforming into a cancerous tumor.
However, it is clear that this process does not always work. All cancers are thought to be the result of a damaged cell failing to commit apoptosis and instead continuing to reproduce itself.
If essential genes required for apoptosis are damaged, it may not be possible for the cell to die. Some doctors and scientists, on the other hand, have been studying apoptosis in depth in the hopes of learning how to trigger it specifically in cancer cells with new medications or other treatments.
How Cell Apoptosis Works With Diabetic Nephropathy
The role of the tuberin/mTOR pathway in apoptosis in type 1 diabetesand in refined proximal rounded epithelial (PTE) cells exposed to HG was investigated because it can balance apoptosis.
Diabetic rodents had more apoptotic cells in their kidney cortex than control rodents. Diabetesenlistment also increased tuberin phosphorylation in relation to mTOR initiation (as measured by p70S6K phosphorylation), Bcl-2 inactivation, cytosolic cytochrome c articulation, caspase 3 activation, and PARP cleavage; insulin treatment prevented these changes. Phosphorylation of tuberin and p70S6K, phosphorylation of Bcl-2, articulation of cytosolic cytochrome c, and caspase 3 activity were all increased in vitro after PTE cells were exposed to HG.
The caspase substrate YY1 was moved from the cytoplasm to the core by high glucose, which improved PARP cleavage. The mTOR inhibitor rapamycin was used to reduce the number of apoptotic cells induced by HG as well as the previously mentioned downstream effects of mTOR activation. In addition, using siRNA to silence tuberin reduced PARP cleavage.
These findings show that in diabetes, the tuberin/mTOR pathway promotes apoptosis in rounded epithelial cells, with cleavage of PARP by YY1 interfering to some extent. Biotin is a water-soluble nutrient that plays a variety of roles in the delegate digestion of starches, fats, and amino acids. Its role as a fundamental, covalently bound cofactor for five carboxylases is what gives it its name.
The mitochondrial carboxylase propionyl-CoA carboxylase (PCC) uses covalently bound biotin as a cofactor. Reduced PCC action in blood lymphocytes reflects a reduction in intracellular biotin status in people who have begun biotin deficiency on a trial basis.
The enactment coefficient (AC) of PCC, which compares PCC action after hatching of unblemished, suitable blood lymphocytes with biotin to PCC action in a similar example before brooding with biotin, is another measure of tissue biotin status. Biotin transport into lymphocytes is also reflected in the increase in the AC of PCC, resulting in apo-PCC mass. During peripheral biotin deficiency, the AC expands, mirroring the intracellular collection of apo-PCC. Because of its small size (244.31 Daltons) and proximity to the watery stage, biotin is likely drained significantly by both hemodialysis and peritoneal dialysis.
However, dialysis patients are now routinely given 150-300 g of biotin orally every day, which is 5-10 times the recommended Adequate Intake (AI) for healthy adults. We hypothesized that poor biotin status may contribute to the pathogenesis of RLS in some dialysis patients under these perplexing circumstances. People with ESRD who are on constant dialysis were studied in the background.
RLS was assessed prior to enlistment by the members' primary care doctors based on clinical side effects, which included a desire or need to move the legs, which is frequently accompanied or caused by loud noises, side effects are more severe when lying still, manifestations are at any rate halfway and incidentally diminished by action, and side effects show a circadian pattern, with a peak in the evening or around evening.
At the hour of enlistment, all members with RLS had an IRLS Group rating scale score of at least 4, confirming the diagnosis of RLS. This scoring system has been shown to be consistent, with a high level of dependability and legitimacy. The IRLS score was calculated using the IRLS examiner, which uses a 10-point scale to assess the seriousness of sleep disturbances as well as the frequency and severity of anxious leg symptoms.
People Also Ask
Does Diabetes Cause Apoptosis?
Both Type 1 diabetes mellitus (T1DM) and Type 2 diabetes mellitus (T2DM) have pancreatic-cell apoptosis as a pathological feature. Insulin resistance combined with visceral obesity causes glucose toxicity, which accelerates cell death through apoptosis in T2DM.
What Is The Mechanism Of Diabetic Nephropathy?
Although the exact cause of diabetic nephropathy is unknown, various mechanisms have been proposed, including hyperglycemia (which causes hyperfiltration and renal injury), advanced glycation products, and cytokine activation.
What Is Destroyed In Diabetic Nephropathy?
Diabetic nephropathy is a common complication of diabetes, both type 1 and type 2. Diabetes that is not well controlled can damage the blood vessel clusters in your kidneys that filter waste from your blood over time. This can damage the kidneys and raise blood pressure.
What Causes Beta Cell Apoptosis?
In type 2 diabetes, chronic exposure to high glucose and free fatty acids (FFAs) causes beta-cell dysfunction and may even lead to beta-cell apoptosis. High glucose exposure has two effects: it causes "glucose hypersensitization" and then apoptosis, both of which are triggered by different mechanisms.
Conclusion
Apoptosis can be triggered by a wide range of physiological and pathological stimuli. However, not all cells will respond to the same stimulus in the same way. Irradiation or cancer chemotherapy drugs, for example, cause DNA damage, which can cause apoptosis in some cells via a p53-dependent pathway. Apoptosis' effect on diabetic nephropathy is being investigated in a number of studies.
There's also the problem of distinguishing between apoptosis and necrosis, two processes that can occur simultaneously, sequentially, or independently. The type of stimuli and/or the degree of stimulation can sometimes determine whether cells die by apoptosis or necrosis. A variety of harmful stimuli, including heat, radiation, hypoxia, and cytotoxic anti-cancer drugs, can cause apoptosis at low doses, but at higher doses, these same stimuli can cause necrosis.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles