Facial Nerve - Anatomic Landmarks For Localization Of The Branches
One of the most feared complications among surgeons and patients is facial nerve injury and subsequent facial musculature paralysis following facial, head, and neck surgery. The paralysis of facial musculature has significant medical, cosmetic, and psychological consequences, so the consequences of facial nerve injury can be devastating for patients.
Author:Suleman ShahReviewer:Han JuMay 31, 202355.9K Shares756.4K Views
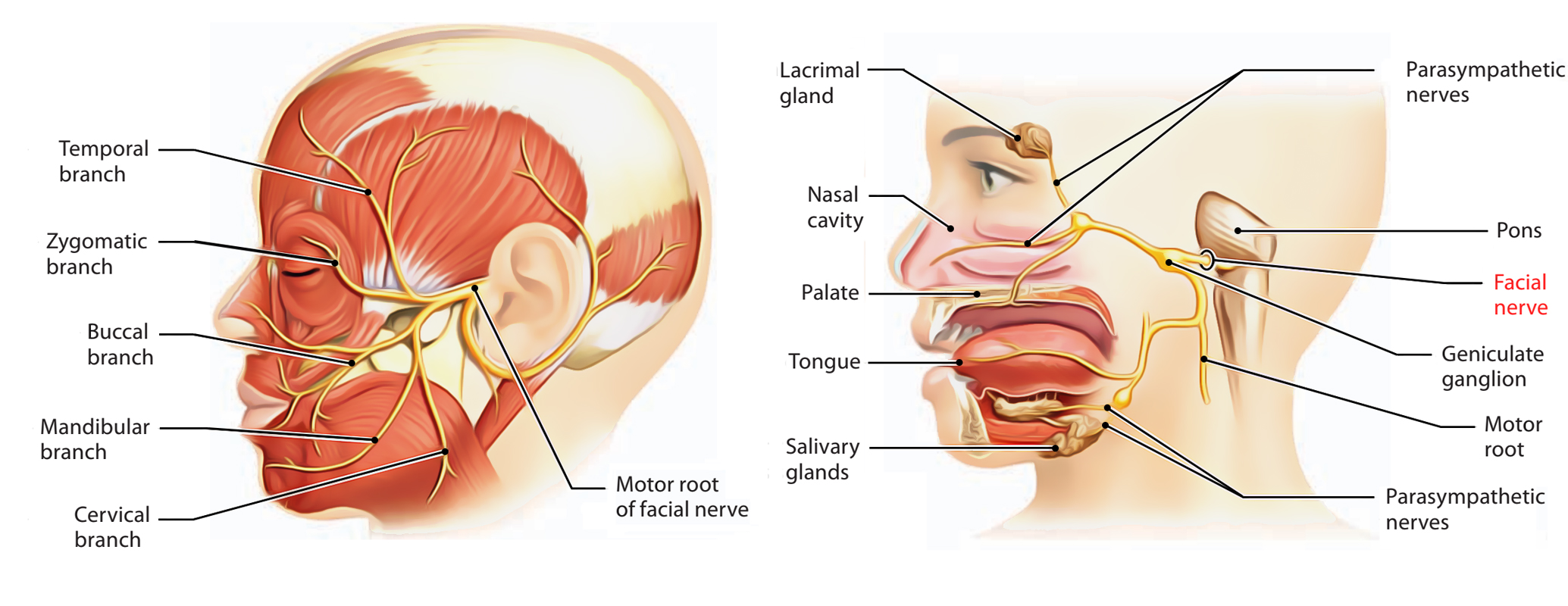
One of the most feared complications among surgeons and patients is facial nerveinjury and subsequent facial musculature paralysis following facial, head, and neck surgery.
The paralysis of facial musculature has significant medical, cosmetic, and psychological consequences, so the consequences of facial nerve injury can be devastating for patients.
While many intraoperative tools are used to reduce the risk of nerve injury, most surgeons still use anatomic landmarks to identify and protect the facial nerve and its divisions. The most useful anatomic landmarks are those that are fixed and can be reliably palpated.
However, a variety of landmarks have been proposed in the literature, and some of the most widely used rely on soft tissue landmarks that vary between individuals, often for historical reasons.
The zygomatic arch, orbital rim, angle of mandible, and mastoid process are among the bony landmarks assessed, while the eyebrow, lateral canthus, lobule, nares, and labial commissures are among the soft tissue landmarks.
Fronto-Temporal Branch
The fronto-temporal branch (FTN) has been extensively studied due to its high rates of injury and significant functional morbidity following injury. Surgical proceduressuch as facelifts, cutaneous surgery, and bicoronal approaches for craniofacial surgical access put the FTN in danger. Pitanguy's line, defined as a line drawn from a point 0.5 cm inferior to the tragus to a point 1.5 cm superior and lateral to the eyebrow, is one of the most widely used clinical estimates of FTN course. Pitanguy's line has been widely criticized by many authors due to its reliance on soft tissue landmarks that vary between individuals and its inability to predict nerve distribution, despite the fact that it does not meet our inclusion criteria.
A total of six studies evaluating the FTN of the facial nerve were found using our search criteria. In 30 cadaveric facial halves, Ishikawa attempted to define the FTN distribution. The nerve's various branches were measured in relation to a line drawn between the lateral canthus and the zygomatic arch's superior border.

The Facial Nerve [CN VII] | Structure, Function, & Major Branches
Zygomatic Branch
The zygomatic nerve (ZN) has been studied in relation to palpable landmarks in only a few studies. During mid-face approaches, the ZN is only rarely injured. However, the ZN was involved in 5.3% of 56 cases in a study looking at facial nerve injury after using coronal approaches for zygomatic fracture stabilization. Recovery from ZN injury was observed in all cases by 3 months after surgery.
Three studies that looked at the facial nerve's ZN were found to be suitable. Saylam et al. looked at the progression of the ZN in 66 cadaveric facial halves that had been fixed in formalin. The nerve's position in relation to the parotid's anterior border, the tragus, and the lateral palpebral commissure was determined. From the tragus to the point of emergence of the ZN at the anterior edge of the parotid gland, the nerve was discovered 30.71 mm away. From a point midway between the tragus and the lateral palpebral commissure, the mean vertical distance to the ZN was 19.29 mm. The distance between the ZN and the zygomatic and masseteric cutaneous ligaments in 22 hemifacial was measured in a second study.
Buccal Branch
Two studies that looked at landmarks for identifying the buccal branch of the facial nerve (BN) were found to be appropriate for review. The parotid duct was used in both studies as a landmark for locating the BN, which is a mobile soft tissue structure. Pogrel et al. looked at the BN's path in 20 cadaveric facial halves and noted where it intersected with the parotid duct.
A single nerve branch was found in 17 of the specimens, with 15/20 (75%) of them running inferior to the parotid duct. In the two remaining specimens, the BN course outperformed the duct. Two nerve branches, one superior and the other inferior to the duct, were found in three out of twenty specimens. From its point of emergence at the parotid gland's anterior edge to where it crossed the duct, the BN traveled a distance of 2.3 mm.
The vertical distance between the duct and the BN was measured when the BN was inferior to the duct, and it was 5.43 ± 3.65 mm. The authors concluded that the duct should be visualized intraoperatively, and that the BN is most likely to be found inferior to the duct, within 1cm. Saylam et al. measured the distance between the tragus and the point of emergence of the BN at the anterior edge of the parotid gland in 66 hemifacial formalin-fixed specimens while documenting the position of the BN relative to the parotid duct.
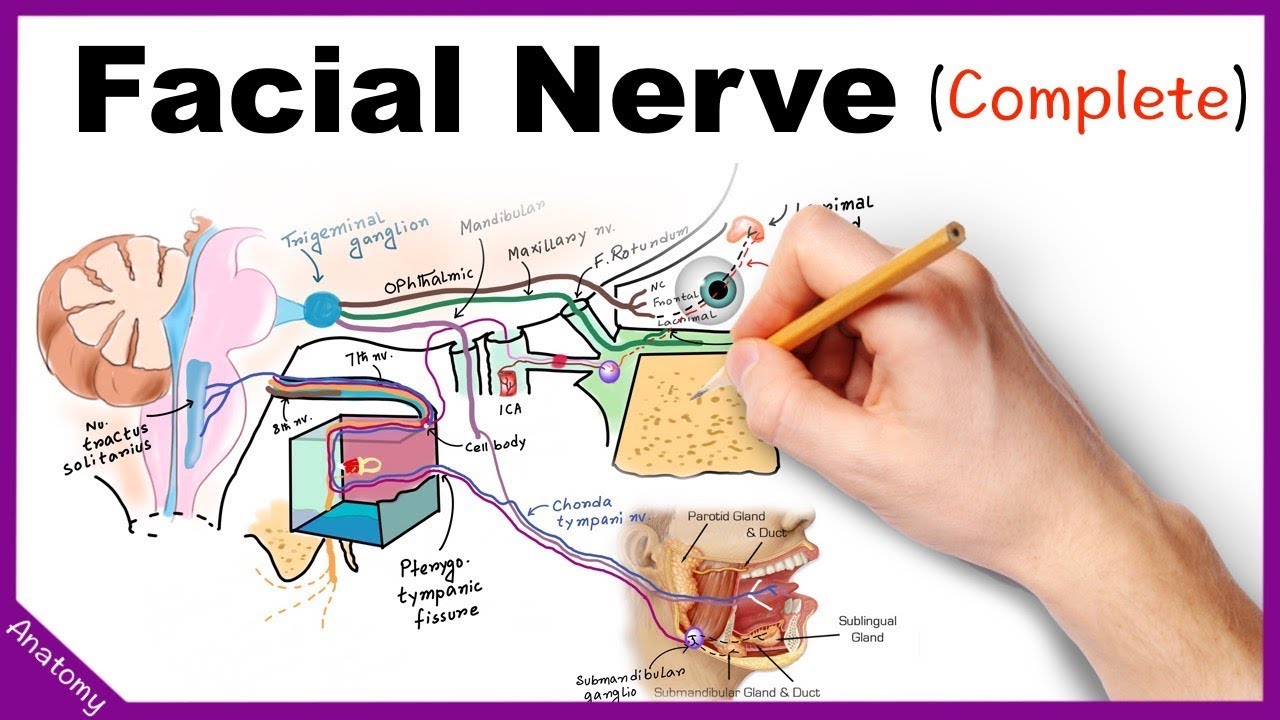
Facial Nerve Anatomy Simplified
Marginal Mandibular Branch
Parotidectomy, rhytidectomy, reduction of mandibular angle fractures, and other types of surgery in the submandibular region have all been linked to injury to this branch. The MMN has been extensively studied because it is frequently encountered during various surgical approaches to the neck and has a variable course. The MMN must be identified and protected during surgical approaches to the neck in order to maintain a symmetric smile and functionality after surgery. A total of four studies were reviewed based on the criteria we used for our search.
The angle of the mandible, facial artery, inferior border of the mandible, parotid edge, lobule, gonion, retromandibular vein, and masseteric tuberosity of the mandible were all used as landmarks to locate the marginal mandibular branch of the facial nerve (MMN). The mandible angle and related structures, the gonion, and the masseteric tuberosity were the most frequently evaluated landmarks.
The MMN was found to be 2.3 mm anterior to the angle of the mandible, 3.33 mm inferior to the angle of the mandible, 3.4 ± 6.0 mm from the gonion to the point of emergence of the MMN at the edge of the parotid gland, and 3 cm anterior to the masseteric tuberosity.
Cervical Branch
The low rates of injury and insignificant functional consequences of platysma paralysis may explain the lack of interest in studying the cervical branch's course and distribution. Cervical branch injury was found in 34 of the 2002 SMAS-platysma face lifts in one study. This amounted to a 1.7% overall success rate, with all patients regaining full function within 3 to 6 months of surgery.
However, there has been a surge in interest in the anatomy of the cervical branch due to its increased use in nerve reconstruction after brachial plexus injuries, neurectomy for pathologic platysmal movement, and intentional denervation to reduce the amount of banding required in the neck during SMAS plication facelifts. Only two of the studies that were found to be suitable for review focused on landmarks important for locating the facial nerve's cervical branch. The cervical branch of the facial nerve was first investigated in 110 formalin-embalmed cadaveric facial halves. In all specimens, the nerve was 0.83 ± 0.37cm posterior to the gonion and did not cross the angle of the mandible.
People Also Ask
What Are The Landmarks For Locating The Main Trunk Of The Facial Nerve?
The following are some of the more well-known landmarks: The anterior tip of the tragus portion of the external ear cartilage is called the "cartilaginous pointer" or "tragal pointer." The main trunk, which is inferior to the pointer, is said to be 1 cm deep.
Where Are The Facial Nerves Located?
At the stylomastoid foramen, a bone opening near the base of the ear, the facial nerve exits the base of the skull.
What Are The Two Anatomical Landmarks?
The ability to correctly number the lumbar vertebrae was determined using commonly used anatomical landmarks (ribs, aortic bifurcation (AB), right renal artery (RRA), and iliac crest height).
What Are The 5 Branches Of Facial Nerve?
The temporal, zygomatic, buccal, marginal mandibular, and cervical branches of the facial nerve emerge from the upper, anterior, and lower borders of the parotid gland, respectively.
Conclusion
Due to the variability in the arrangement of facial nerve anatomy, navigation to the various branches of the facial nerve using anatomic landmarks remains difficult. The use of soft tissue landmarks is common, but they are mobile and have a wide range of morphology. Bony landmarks are more reliable, but only a few have been described, and even fewer studies have attempted to evaluate the accuracy of independent raters' landmark identification.
Many studies use linear measurements from landmarks to locate the nerve, but patients vary in size, and because all of the studies found were done on adult specimens, surgical procedures on children cannot rely on these measurements.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles