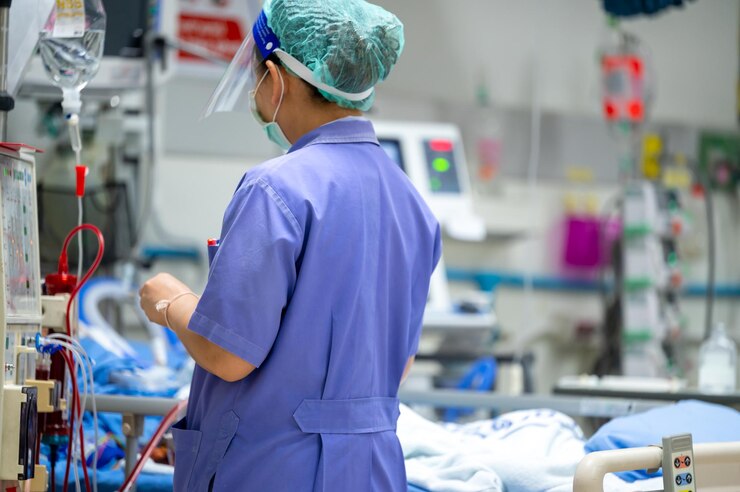
Fever After Dialysis – Its Effects On Dialysis Patients
Fever after dialysis is commonly caused by respiratory or digestive infections in patients during dialysis sessions.
Author:Suleman ShahReviewer:Han JuAug 16, 2022136 Shares2.1K Views
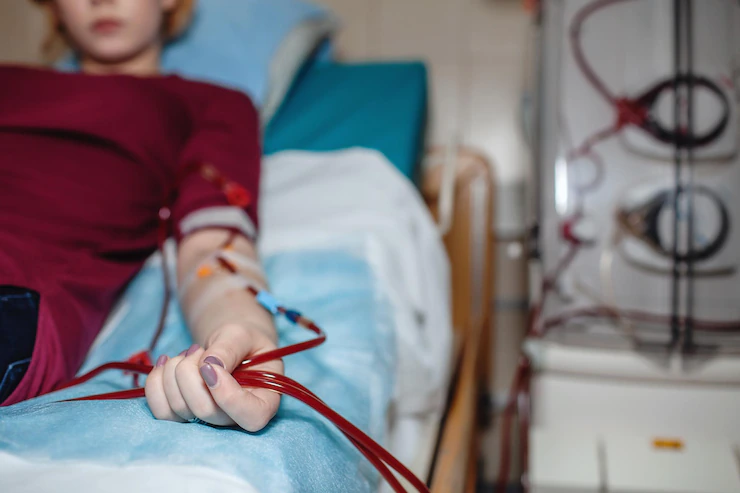
It might be intimidating initially, but many dialysis patients have full and busy lives.
Fever after dialysisis commonly caused by common respiratory or digestive infections in patients, but an endovascular infection should be anticipated when chills accompany fever during dialysis sessions.
Fever is sometimes related to autoimmune illnesses or malignant tumors.
Usually, historyand clinical examination, basic investigations of white blood cell count and urine, blood cultures, chest X-ray, abdomen ultrasound, or echocardiography may resolve the differential diagnosis of fever in dialysis patients.
Dialysis Side Effects
However, both peritoneal dialysis and hemodialysis may cause complications.
Side effects might be moderate to severe depending on your healthand whether or not you follow your food and hydration restrictions.
Most side effects are manageable if you follow your care team's advice.
- Hernia:Putting a catheter in your abdomen so that dialysis solution can go in and out could weaken the muscles holding your organs, leading to a hernia.
- Feeling overstuffed:Some dialysis patients find eating difficult because the dialysis solution makes them feel full. It may result in malnutrition.
- Bloating and weight gain:Bloating and weight gain are frequent side effects of Parkinson's disease. The fluid bloat from the dialysis solution accounts for some of the weight. Weight gain can also happen if the body absorbs the sugar in the dialysis solution, which can cause weight gain.
- Low blood pressure:Low blood pressure is the most frequent hemodialysis adverse effect, which may occur when too much fluid is removed from the blood during treatment. This creates a reduction in pressure, which causes nausea and dizziness.
- Muscular cramping:Some people have muscular cramps when too much fluid is eliminated or removed too rapidly.
- Clots in the blood:A blood clot may form in access. Check your entry regularly for the thrill (the pulse felt in the fistulaor graft) to ensure it is operating correctly.
- Itchy skin:Itchy skin is caused by elevated phosphoruslevels. Because dialysis can not correctly remove phosphorus, foods containing phosphorus are prohibited from the renal diet.
- Dry skin:Dialysis patients are also prone to dry skin, which may cause itching. Use moisturizing moisturizers instead of hot showers and abrasive soaps.
- Infection:Peritonitis, an infection at the catheter site, is a danger in Parkinson's disease. Peritonitis is characterized by fever, nausea, vomiting, and stomach discomfort.
- Negative sexual outcomes:Some sexual side effects of dialysis include a lack of libido, trouble getting an erection, and dryness in the vaginal area.
- Mental illness:A chronic ailment, such as renal disease, may be complex. In addition to physical pain, you may worry, feel hopeless, and notice a change in how you see yourself.
Fever And Chills After Dialysis
Chills are a complication of hemodialysis patients.
The prevalence of infection among hemodialysis patients who report having chills is unknown, and empirical broad-spectrum antibiotics are routinely used.
Patients who appear with chills during dialysis, with or without fever, have a substantial risk of infection.
Patients with no apparent source of infection, access by fistula or graft, and no fever, leukocytosis, or hypoalbuminemia are at minimal risk for bacteremia.
They may be studied without urgent antibiotic therapy.
All other patients should be given antibiotics right away if they have chills.
Fever in hemodialysis patients is often caused by infection, with less common reasons including cancer and autoimmune illnesses.
Sometimes, despite empirical therapy, fever continues, and examinations of the diagnosis above fail to discover the reason.
Thus, unusual etiologies must be examined, which may reveal some surprises, particularly in individuals who have been under medical supervision for a long time.
Treatment Of Fever In Dialysis Patients
The most common causes of fever in patients with renal failure and dialysis were infections of the bronchopulmonary system, urinary tract, or dialysis access site ('the big three').
There is an essential preponderance of bacterial infections in dialysis patients.
Two causes of renal failure are dialysis patients' late transplant rejection and peritoneal tonitis.
In a significant number of patients, the cause of fever could not be explained because fever and infection subsided before the diagnosis could be made, or it was of unknown origin.
Usually, the differential diagnosis of fever in dialysis patients can be cleared by history and clinical examination.
Patients should be given straight-forward ward treatment with vancomycin one g/week if the staphylococcal infection is suspected or a broad-spectrum beta-lactam antibiotic if another infection is likely.
If fever arises in the hospital or the patient is in bad condition, an aminoglycoside should be added with therapeutic drug monitoring.
Abscesses should be drained immediately and infected foreign bodies removed.
If fever continues after 4 days, the first diagnosis should be reconsidered.
Suppose one is perplexed by prolonged fever in a patient.
In that case, it is best to reevaluate the patient's history and examination, review charts, consult another physician, and discuss the problem with colleagues.
If fever persists for more than 3 weeks, four treatable causes of "fever of unknown origin" should be thoroughly excluded: Bacterial endocarditis; (2) intra-abdominal infections or abscesses; (3) tuberculosis; and (4) bone or joint infections.
Patients who are on regular dialysis treatment hardly ever present with factitious fever.
Although there may be rare cases like brucellosis in dialysis patients, there is usually no exotic disease but rather a masked, well-known cause of fever.
Caring for a dialysis patient with prolonged fever of unknown origin requires more than ordering a battery of the newest screening methods.
Every case of fever that lasts for a long time may be a mystery that tests all of a good doctor's scientific and communication skills.
How To Feel Better After Dialysis?
However, dialysis is not a one-time procedure.
You'll do it multiple times a week for one form of therapy and every day for another.
This may take many hours of your time, not to mention travel time if you need to go to a clinic for treatment.
All of this is a significant change in anyone's life.
It might be intimidating initially, but many dialysis patients have full and busy lives.
Here are some coping strategies.
Participate Actively In Your Treatment Team's
Learn all you can about dialysis. Consider all of your alternatives.
Knowing the facts will enable you to participate actively in treatment choices.
This is one of the most effective techniques to deal with worry and fear.
Make a list of questions to ask your doctor and nurse.
Talk to your social worker about your emotional needs.
Consult your dietician about dietary health concerns.
Make sure to include your relatives.
Make sure you have the assistance you need at home.
Keep An Eye Out For Depression.
Dialysis may have a significant impact.
You could have less time and energy.
Changes may be required at home and work.
You may have to give up certain hobbies and obligations, for example.
As a result, depression is widespread among dialysis patients.
It is natural to feel depressed at times in the beginning.
But be wary of real depression.
It is not typical to be depressed for longer than two weeks.
If your mood, appetite, sleep schedule, or energy level change, or if you lose interest in things you used to enjoy, you should see a therapist.
Have Fun With Your Life
Dialysis might compel you to alter your routine.
However, try to resume as many routine activities as possible.
Many dialysis patients continue to work.
Speak with your boss while holding a doctor's report.
Many of your prior activities may be resumed if you prepare correctly and remain flexible.
Try not to think of yourself as unwell.
This will benefit you in the long term.
Keep Exercising
Exercise is one of the most effective strategies to combat weariness and sadness.
Consult your doctor first to determine how much and what sort of exercise is appropriate for you.
Exercise will also assist you in reducing stress.
It will also improve your strength and endurance.
These advantages pile up.
You will have a higher quality of life.
If you're having problems keeping motivated, exercise with a friend or family member.
Make The Most Of Dialysis Time
It might be challenging to spend time connected to a computer.
That is why it is important to make the most of your time.
Don't let it go to waste.
Use it to catch up on emails or work on your laptop.
Or read a book you haven't had time to read.
To de-stress, you might also listen to music or practice guided meditation.
Use your dialysis time to your advantage.
Get A Restful Night's Sleep
Sleep issues are frequent among dialysis patients.
You may have difficulty falling or staying asleep.
You may also suffer from sleep apnea or restless legs syndrome.
Sleep deprivationmay cause daytime tiredness, headaches, and melancholy.
They may make dealing with dialysis more difficult.
Most individuals find that moderate exercise improves their sleep.
Avoid alcohol and caffeine as well.
Inform your doctor if you have any sleep issues.
Sleep apnea and RLS may both be treated.
Adhere To A Dialysis Diet
Your dialysis dietician may advise regulating your thirst and restricting fluid consumption.
You may also learn to avoid meals high in potassium, phosphorus, and salt.
Instead, load up on high-quality protein and calories.
You may establish a balanced meal plan with a little assistance that will help you cope by making you feel healthy and energetic.
Maintain A Positive Attitude
Begin by embracing your current position. Think about how dialysis may assist you.
It allows you to go about your daily life.
Consider the fact that some dialysis patients live as long as people who do not have renal disease.
Consider how much better you feel after dialysis.
Talk to your care team if you can't seem to get your mind to think positively.
Counseling might help you get through this difficult period.
People Also Ask
Why Do I Feel So Sick After Dialysis?
Low blood pressure is the most frequent hemodialysis adverse effect, which may occur when too much fluid is removed from the blood during treatment.
This creates a reduction in pressure, which causes nausea and dizziness.
Is It Normal To Have Chills After Dialysis?
Chills are a complication of hemodialysis patients. The prevalence of infection among hemodialysis patients who report chills is unknown, and empirical broad-spectrum antibiotics are routinely used.
What Are Common Side Effects Of Dialysis?
- Blood pressure is too low (hypotension)
- Cramps in the muscles
- Itching
- Sleep issues
- Anemia
- Bone disorders
- Blood pressure is high (hypertension)
- Overflow of fluids
Why Do Dialysis Patients Get Fevers?
Fever in haemodialysis patients is often caused by infection, with less common reasons including cancer and autoimmune illnesses.
Sometimes, despite empirical therapy, fever continues, and examinations of the diagnosis above fail to discover the reason.
Conclusion
The range of infections in dialysis patients has not changed much.
Infections of Scribner shunts, on the other hand, have given way to infections of central vein dialysis catheters.
The widespread use of vascular prostheses, which are more prone to infection than natural arterio-venous fistulas, is causing considerable worry.
When feasible, avoid central, particularly suclavian vein catheters; preserve natural veins; plan for vascular access in patients with renal insufficiency; and maintain the access site with care throughout dialysis.
In addition, nasal muciprocin ointments for the elimination of Staphylococcus aureus carriage and erythropoietin for the treatment of iron excess have been indicated.
Vaccination against pneumococcal and influenza viruses may lower the risk of pneumonia caused by pneumococcus or secondary to influenza.
Cuprophan dialysis membranes are suspected of playing a role in infections.
The biology of fever and the effects of uremia on host defenses mean that controlling fever in dialysis patients needs a practical approach by the clinician and vigilant nursing during dialysis.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles