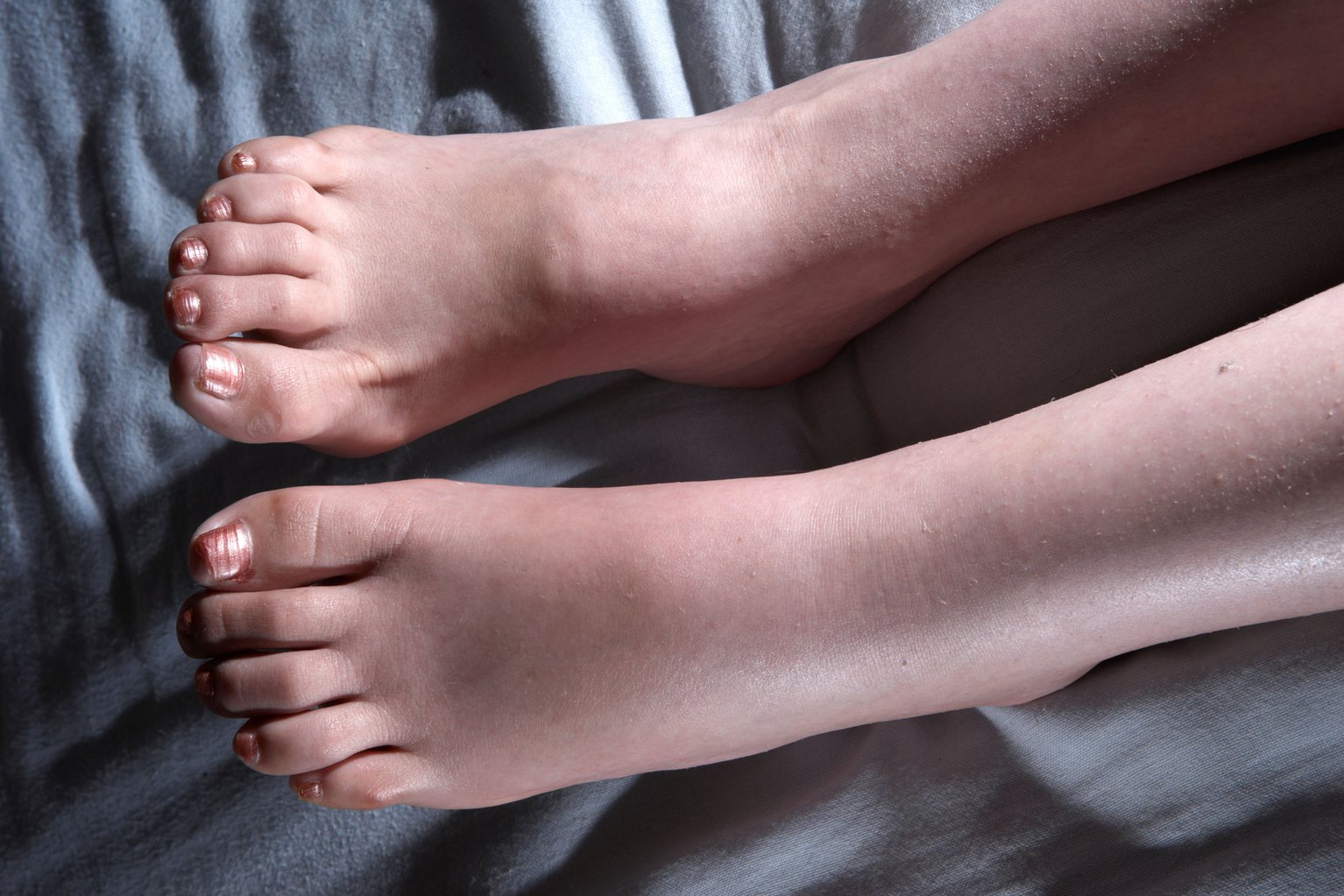
Inflammation - A New Look At The Role Of Aquaporins
Scientists have always been interested in the inflammatory process and the complicated mechanisms that control it, especially the roles of the different parts. Inflammation is a complex process that involves how the body reacts to being hurt. Some of the things that can cause inflammatory tissue damage are trauma, heat, chemicals, toxins, and microbes.
Author:Suleman ShahReviewer:Han JuJul 24, 202252 Shares790 Views
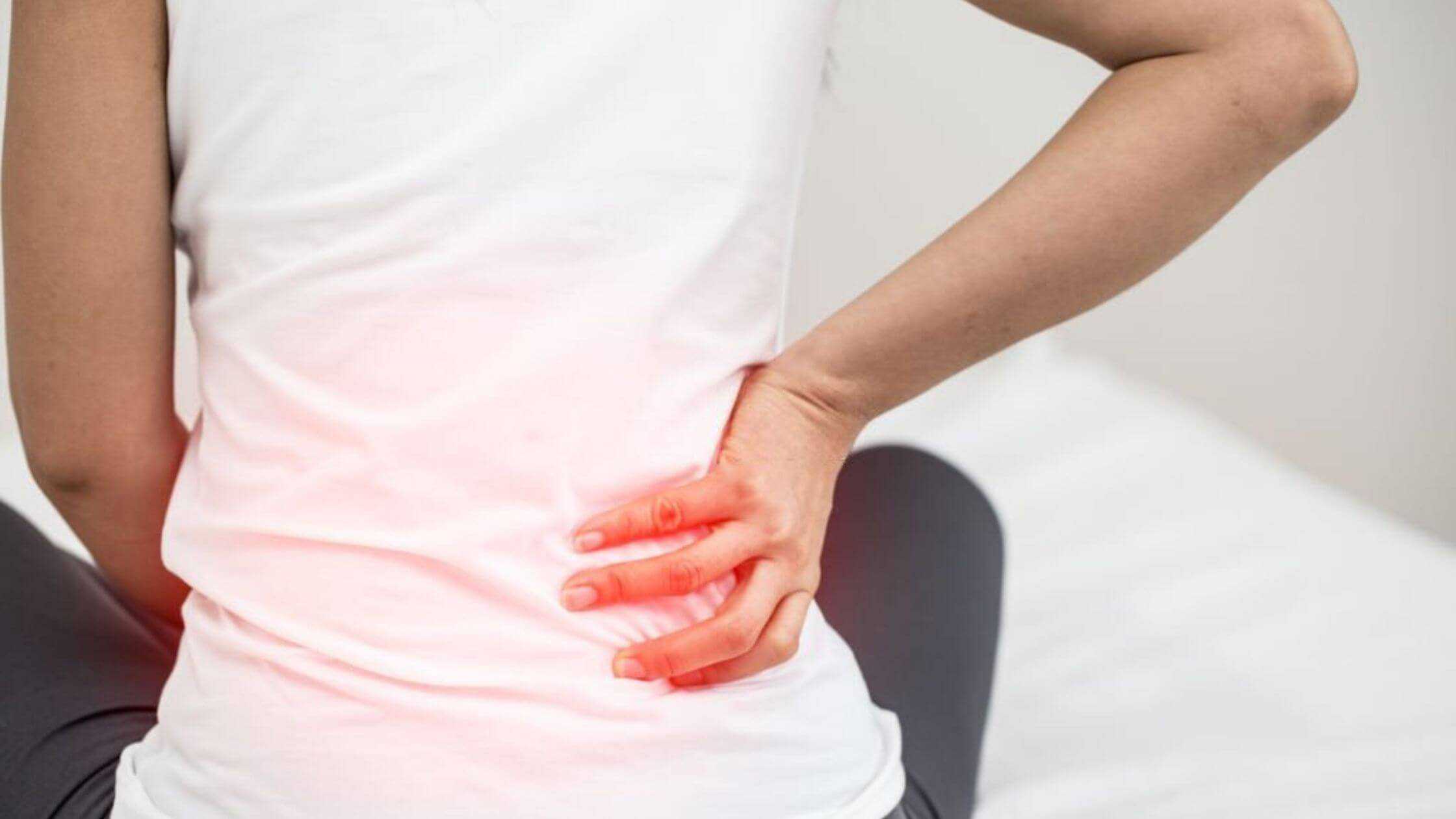
Scientists have always been interested in the inflammatory process and the complicated mechanisms that control it, especially the roles of the different parts.
Inflammationis a complex process that involves how the body reacts to being hurt. Some of the things that can cause inflammatory tissue damage are trauma, heat, chemicals, toxins, and microbes.
Different immune cells are involved in both acute and chronic inflammatory processes, which use up a lot of metabolic energy, cause function loss, tissue damage, and destruction, and use up a lot of metabolic energy.
All inflammatory responses are set up by many signals, and the immune systemplays a key role. In general, it can be broken up into two parts that work together.
The innate immune system, also called the non-specific immune system, is made up of cells and processes that protect the host from infections caused by pathogenic organisms. These cells and processes find infections and send signals to the brain.
These signals are needed to start the inflammatory cascade and the second part of the immune system, the adaptive immune response.
During activation, the injured tissues release many chemicals that cause changes in the nearby healthy tissues.
Aquaporins
Aquaporins (AQPs) are a group of integral membrane proteins with six transmembrane helices that are organized as monomers, dimers, and tetramers to form pores in the membranes of living cells. The first aquaporin was found in human erythrocytes and renal proximal tubule membranes. It was first called CHIP28 but was later renamed Aquaporin 1 (AQP1).
Since this discovery, many other proteins from the same aquaporin family have been found in mammalian cells, as well as in bacteria, plants, and fungi, and in all kingdoms of life. AQPs make holes in biological membranes and act as selective channels that let water (aquaporins) and small molecules or solutes (aquaglyceroporins) pass through.
The large family of aquaporins, which is made up of 13 proteins, has a new group called "unorthodox aquaporins." These last proteins are the least understood. Their structure and where they are found in the cell are two ways in which they are different from the other groups.
Scientists are curious about the structure and function of AQPs because they are found in a variety of cells and tissues. This supports the idea that water permeability is important for many physiological processes.
This conclusion is based on the fact that water is the most important part of any living thing and that water is constantly moving between almost all body tissues.

Inflammation - causes, symptoms, diagnosis, treatment, pathology
Aquaporins And Inflammation
In host-pathogen interplay, the immune system and communication between the host and the pathogen work together. In particular, cells that are involved in inflammation can have changes in their osmotic microenvironment, which can lead to an increase in cell hydraulic permeability and size as well as changes in the structure of their cytoskeleton. In some cases, weak bacterial stimuli can cause tissue damage, but they can also cause a stronger response and more damage, which can lead to long-term inflammation.
Many articles have talked about how AQPs might be involved in inflammatory processes, which makes sense since some of them are found in both innate and adaptive immune cells. AQPs are especially important for phagocytic functions and certain immune cell processes (i.e., activation and migration).
Aquaporins And Phagocytic Functions Of Immune Cells
During phagosome development, macrophages quickly change their size and shape, which affects water transport and volume regulation, both of which are needed for phagocytic cup formation. It has been suggested that AQP3 is involved in the formation of phagosomes using a mechanism similar to what has been seen in young human dendritic cells.
This mechanism shows that the transport of glycerol is an important part of macrophage phagocytosis. In fact, when AQP3-deficient mice were given a model of bacterial peritonitis, they died more often than wild-type mice. The ability of peritoneal macrophages from AQP3(−/−) mice to let water and glycerol in was less than that of macrophages from AQP3(+/+) mice.
Also, giving AQP3(−/−) mice extra glycerol helped restore some of the ATP and macrophage function that had been lost. AQP3 was found to be an important new part of the immune function of macrophages. It helps move water and glycerol and then takes part in phagocytosis and migration.
The effects of AQP3 also showed that the metabolic pathways for glycerol and glucose talk to each other. Changes in the amount of glucose and glycerol were also seen in AQP3(−/−) keratinocytes, pointing to a possible new role for glycerol in the way macrophages use energy.
Aquaporin Involvement In Migration Of Immune Cells
Loitto et al. were the first to show that AQPs are involved in cell migration. They showed that blocking AQP9 made it harder for neutrophils to move. Other studies showed that AQP1 and AQP4 were found at the leading edge of migrating CHO cells and astroglial cells, respectively, proving that AQP plays a role in cell migration.
Other data has shown that several AQPs make it easier for immune cells to move. In particular, chemokine-dependent T cell migration needs hydrogen peroxide to be taken in through AQP3-mediated uptake, which controls the immune response inside the cells.
AQP3 is also found in macrophages, and it is controlled by TNFα, PPARγ, calcium, and low pH, among other things. These results show that AQP3 is involved in the process of inflammation.
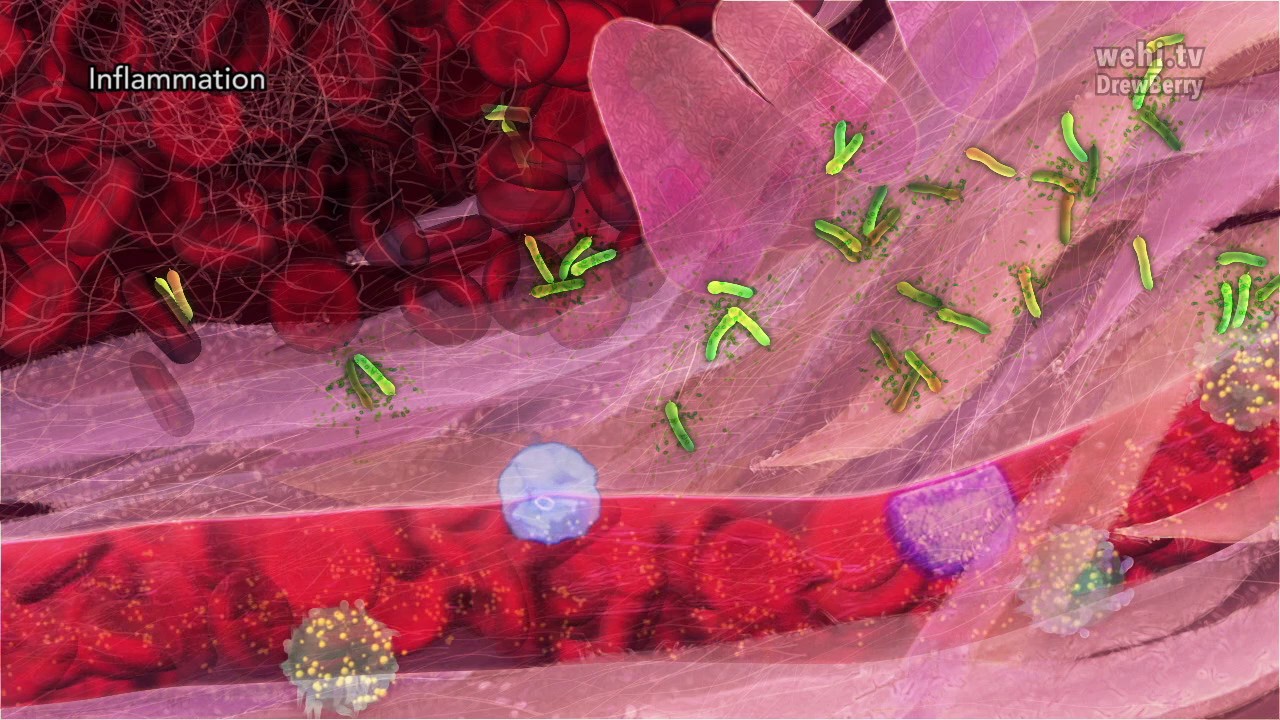
Inflammation
Aquaporins And Bone And Cartilage Diseases
AQPs have recently been used in research on a number of inflammatory diseases that affect bone and cartilage. It is well known that the main things that go wrong with rheumatoid arthritis (RA) are very high levels of inflammatory cytokines that are released by activated B and T cells and damaged cartilage and bone.
At the same time, different AQPs have been found in the cells of cartilage, where they control the flow of ions and molecules and, by doing so, control how the cartilage works.
Nagahara et al. showed that TNF could control the expression of either AQP9 mRNA or protein in synovial tissues in people with osteoarthritis (OA) and rheumatoid arthritis (RA). This result points to a specific role for cytokines, which could affect how AQP works by changing the activity of glucose transporters, which are important for chondrocyte metabolism.
According to this mechanism, AQP1 on the chondrocyte membrane could act as a regulator of metabolic or extracellular matrix water. This means that chondrocytes might change how they control their volume if their ionic and osmotic environment changes.
In a model of OA cartilage, RT-PCR was used to look at AQP1 mRNA and show that up-regulation of AQP1 was linked to the death of chondrocytes. This showed that AQPs play a direct role in the development of this disease.
Aquaporins In Bowel Diseases
The gastrointestinal tracts of humans and other mammals have shown that AQPs are present and play a role in both healthy and unhealthy processes. It was found that AQPs are involved in many ways that water moves through the body (intestinal permeability, fluid secretion, and absorption).
Concerning how AQPs are controlled, it is known that different substances (such as hormones and parts of the food we eat) change how they are expressed, which changes fluid homeostasis and a number of local mechanisms. In this rule, cAMP's role was also talked about.
Inflammatory bowel diseases (IBDs) are relapsing inflammatory diseases of the digestive tract that cause the immune system to be overstimulated, the gut to become inflamed, and fluid, solutes, and lipids to leak out of the bowel mucosa. Gut microflora is involved in IBDs.
IBDs have also been linked to problems with how electrolytes and water move through the body, which leads to changes in permeability and diarrhea. Because of this, a lot of research has been done on the link between colitis and AQPs.
In particular, the large increase in intestinal membrane permeability seen in these diseases has led researchers to think that AQPs may be involved. Also, it is well known that the amount of inflammation is linked to cytokines, which are important signaling molecules of the immune system in the gut.
TNFα and IL-1β, in particular, play a key role in gut inflammation by directly affecting intestinal epithelial tissue, which acts as a barrier between genetic, environmental, and immune factors.
Involvement Of Aquaporins In Neuroinflammation
The physiological and pathological role of AQP's expression and function in the nervous system is supported by more and more evidence from people and animals. A lot of research has been done on the possible role of these channel proteins in neuroinflammation.
For example, neuromyelitis optica (NMO) and multiple sclerosis, both of which are caused by a failure of innate immunity, have been studied.
The channel protein AQP4 is made by astrocytesin the CNS. It controls how water moves through the brain, how neurons fire, and how astrocytes move. In fact, lesions seen in people with NMO show that specific autoantibodies that target AQP4 are expressed on the membrane of astrocytic cells. This changes how cells work in different ways.
Among these, evidence was found of activation of the complement system, cellular cytotoxicity caused by an antibody-dependent mechanism, or both. NMO-IgG goes after AQP4, which is a specific target.
Also, it has been proven that AQP4 is involved in neuroinflammation (i.e., water poisoning and ischemic stroke) by showing that AQP4-deficient mice have less brain swelling and swelling of pericapillary astrocytic foot processes.
These results show that AQP4 plays a key role in controlling how water moves through the brain. They also suggest that blocking AQP4 could be a new way to treat conditions like cerebral edema, which are at the root of a number of brain diseases.
Inflammatory Diseases In Domestic Animal Species - The Involvement Of Aquaporins
In the past few years, a lot of research has been done on inflammatory diseases in domestic animals. However, there isn't a lot of information available because of ethical problems with using these animals as lab animals.
But there is evidence that both animals and people can get some inflammatory diseases, the causes of which are not always clear. Even though different diseases in domesticated species have been looked into, there haven't been many studies on the possible link between AQPs and inflammation. The dog is probably the most studied species because it is so similar to humans.
In particular, diseases caused by inflammation in organs and systems like the gut, central nervous system, and lungs have been studied in dog species with the goal of figuring out their pathophysiology and coming up with good treatment plans. In this way, Cerquetella et al. looked at the dysbiosis networks in IBDs in dogs, showing both differences and similarities with IBDs in humans.
The results of this study, which show important new things for translational medicine, mean that scientists need to do more work to figure out why some types of bacteria in dogs and humans are different. An interesting study also showed that the levels of AQP4 and IL6 in the cerebrospinal fluid (CSF) of dogs with idiopathic communicating internal hydrocephalus went up, but that these proteins went down after ventriculoperitoneal shunting.
A study on beagle dogs with acute respiratory distress syndrome showed a clear inflammatory process marked by a rise in TNFα, which can help cytokines like IL-1A, IL-6, and IL-10 be released. Also, damage to the pulmonary capillary membrane barrier may cause AQP1 and AQP5 to be less active. This suggests that they may be involved in controlling how fluid moves along this membrane.
Also, the expression of AQPs in birds has been looked at at the level of the nasal gland and the fluid it makes. In particular, AQP1 and AQP5 seem to help control nasal fluid secretion, which in invertebrates is always very salty.
People Also Ask
What Is Inflammation In The Body?
Inflammation is your body's attempt to heal itself by fighting off things that hurt it, like infections, injuries, and toxins. When something hurts your cells, your body sends out chemicals that tell your immune system to do something.
What Are The Five Most Common Signs Of Inflammation?
Pain, heat, redness, swelling, and loss of function are the five main signs of this response. Not every case of inflammation has all five of the main signs.
How Do I Get Rid Of Inflammation Fast?
Cut back on sugar and processed foods to reduce inflammation quickly. But it may be more important to exercise, do things that help you relax, get a good night's sleep, and eat lots of colorful, anti-inflammatory foods.
Will Inflammation Go Away On Its Own?
If acute inflammation is not treated, it should go away in a few days. Make an appointment with your doctor if you have any signs of inflammation that has been going on for a long time. They can do some tests and look at your symptoms to see if you need treatment for any underlying conditions.
Conclusions
The evidence mentioned above suggests that AQPs are more than just proteins that move things around. This is because immune and epithelial cells lose control of AQPs in response to infectious and inflammatory stimuli.
The fact that AQPs are involved in inflammation can help us learn more about the complicated ways that the body and pathogens talk to each other. Overall, it seems clear that AQPs are new potential therapeutic targets for controlling edema, cell migration, and the release of inflammatory cytokines and mediators.
Future research is needed to learn more about the molecular mechanisms that cause inflammation in response to osmotic stress and to find out more about the signaling pathways that control how AQPs work. Having these basic skills could help explain why osmotic imbalances are important not only in inflammation and diseases caused by inflammation but also in cancer.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles