Iontophoresis – The Most Effective Way To Deliver Cardiovascular Drugs
Iontophoresis, which uses a low current, has significantly impacted the skin permeation process.
Author:Suleman ShahReviewer:Han JuJul 05, 202261 Shares1.4K Views
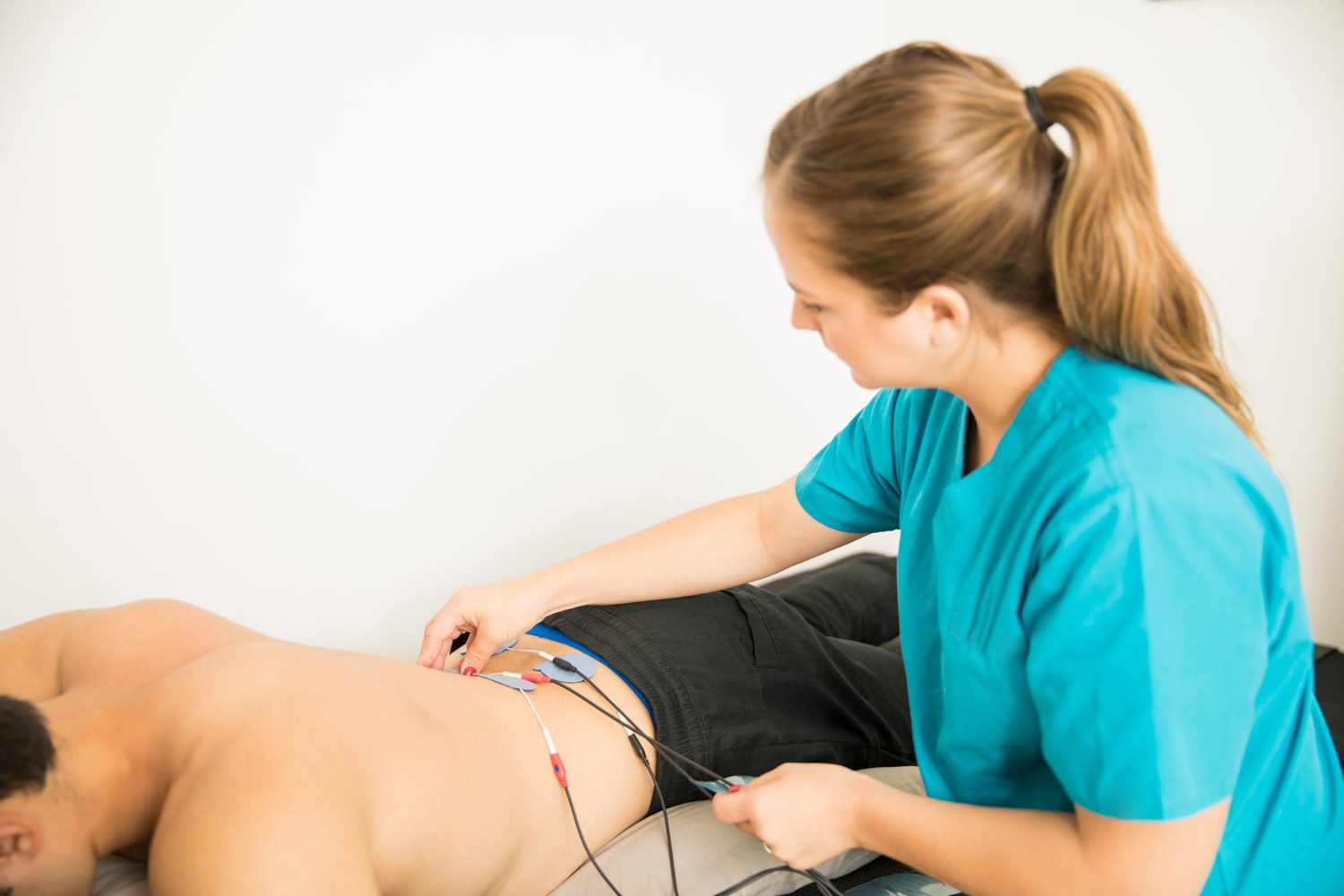
Because most medications penetrate poorly through the skin, attaining therapeutic levels through increasing permeation rate is a significant difficulty. Iontophoresis, which uses a low current, has significantly impacted skin permeation.
Ideally suited for protein therapeutics, efforts have been made to use the technique to accelerate the development of low-molecular-weight medications for long-term administration.
However, commercialization was not possible until recently because of the difficulties involved with energy supply. Fortunately, the tremendous expansion of microelectronics has filled this need and catapulted the technologyinto the spotlight.
What Is Iontophoresis?
A medical device employs modest electrical currents to transfer medicine across biological membranes during iontophoresis, generally done while your injured body part is immersed in water.
Iontophoresis is most typically used to treat hyperhidrosis problems, which causes chronic and excessive sweating.
Currents are often administered to the hands, feet, or armpits to block sweat glands temporarily. Some people experience a mild tingling sensation during the process, although the electrical current is not powerful enough to shock them.
Sweating may occur in response to particular triggers, such as hot weather or physical exertion, or it may occur without any stimulus. Medical illnesses such as hyperthyroidism or menopause may also induce it.
Iontophoresis may be used to treat sports injuries and hyperhidrosis by administering anti-inflammatory drugs directly into the skin.

IONTOPHORESIS - How Does It Work?? - We Break It Down HERE
Iontophoresis Properties
In addition to the typical drug reservoir, an iontophoretic device requires an energy supply. Once triggered, the source produces energy in a predetermined and regulated way.
The skin has a net negative charge at physiological pH, and cations traverse the skin barrier more effectively than anions. The electric current causes a potential gradient across the skin tissue, and the charged drug is repelled from the drug reservoir underneath the active electrode.
Human skin pores are substantially broader and more linear than the convoluted uneven channel that runs through the lipophilic matrix of unbroken skin. Because iontophoretic propulsion is directly related to current intensity, the technology is anticipated to assure planned and repeatable medicinal material delivery.
Iontophoretic Research Approaches
Iontophoretic system development is a diverse research activity that may be divided into numerous categories.
While the energy supply device is a specialized microelectronic research area, formulation development must address specific vital issues: the pathways of percutaneous penetration must be characterized, rate-limiting steps in transdermal absorption must be identified, the particular drug structure-penetration relationship must be understood, and the skin safety factors must be evaluated.
The laser scanning confocal microscopy and vibrating probe electronic technology are used to determine the mechanism of molecular penetration.
According to research on pindolol, radial mass transfer is the primary mechanism of iontophoresis. Identifying the skin's propensity for various ions and structures may also help improve a formulation.
Skin impedance and reversibility measurements are often used to assess safety and optimize medication delivery. However, the primary emphasis of pharmaceutical research is on improving permeability, which may result in the improved therapeutic effectiveness of medications.
Researchers are evaluating the viability of this technology to extract the drug molecule from the subdermal area for noninvasive therapeutic medication monitoring since it is a promising approach.
Iontophoresis Use In Cardiovascular Drugs
Fentanyl, an analgesic patch, has become a blockbuster product, with an annual turnover of 1.59 billion US dollars in 2002. Transdermal nitroglycerine has been approved for use in acute myocardial infarction by the American Heart Association.
Permeation is being explored using both passive and energy-assisted methods. The repeatability of drug flow is the greatest issue in passive delivery. Flux values determined from passive permeation vary depending on species, skin type, and skin area.
Iontophoresis employs a trans-follicular route, and the densities of follicles in animals and humans vary. The penetration rate of Nadolol increased 1225 times.
Because the medication is somewhat soluble in water and the freebase is highly lipophilic, the enhanced impact of iontophoresis may be ascribed to the aid of ion-exchange resins. Two passive permeation measurements for propranolol hydrochloride differ significantly, suggesting the influence of species difference.
Because it has a low molecular weight and is water-soluble, atenolol is theoretically an excellent choice for iontophoresis.
Standard Methods For Increasing Iontophoretic Flux
Standardization of numerous parameters, skin conditions, and formulation excipients are required for optimizing iontophoretic administration. Still, the manner and duration of energy delivery are the most crucial and researched areas. Because the energy delivery method affects the flux, research is conducted to determine the appropriate current density and the pattern of energy supply.
One of the ways used was switching iontophoresis, which involves reversing the polarity of electrodes on transdermal absorption. Verapamil permeation was shown to be more significant at a particular switching interval, and the permeability coefficient and cumulative quantity improved considerably. Increasing the current density in most circumstances enhances mass transmission, but a limiting value of 0.5 mA/cm2 is considered safe and sufficient.
Optimization of formulation parameters is often done using ionic strength, pH, buffer types, specific adjuvants, and the membranes used in the formulation. The parameters such as pH, ionic strength, drug concentration, and so on considerably impacted iontophoretic flow.
The inclusion of particular adjuvants in the device, such as ion exchange resins, is also advantageous. Transdermal permeation may be stereo-selective in some instances. Yes, researchers have investigated this strategy in maximizing permeability.
Manipulating the association state and generation of charged analogs might be a helpful strategy for proving iontophoretic delivery. The construction of insulin analogs with additional negative charges resulted in 50 to 100 times flux augmentation.
Skin moisture was discovered to be an essential characteristic that may improve penetration rate. Similarly, removing skin lipids by alcohol therapymay help with delivery. As a result, these basal therapy attempts are being made to maximize the penetration rate.
Another strategy that researchers examine is using permeation enhancers in the donor vehicle to increase iontophoretic flow. Because electroporation and iontophoresis have the same common denominator of electro-repulsion, an effort is also being made to improve iontophoretic flow by lowering skin impedance via early electroporation.
People Also Ask
What Is The Process Of Iontophoresis?
The method of delivering a small electrical current through the skin is known as iontophoresis. Iontophoresis offers a wide range of medical applications. The use of iontophoresis to reduce perspiration by inhibiting sweat glands is discussed in this article.
What Is Iontophoresis And How Does It Work?
A medical device employs modest electrical currents to transfer medicine across biological membranes during iontophoresis, generally done while your injured body part is immersed in water. Iontophoresis is most typically used to treat hyperhidrosis problems, which causes chronic and excessive sweating.
What Is Iontophoresis Used For?
Physical therapists employ iontophoresis to treat various ailments, including bursitis, tendonitis/tendinopathy, and scar tissue management. It uses electrical stimulation to assist in administering drugs into your body via the skin.
What Does Iontophoresis Machine Do?
A medical device employs modest electrical currents to transfer medicine across biological membranes during iontophoresis, generally done while your injured body part is immersed in water. Iontophoresis is most typically used to treat hyperhidrosis, which causes chronic and excessive sweating.
Conclusion
Iontophoresis is considered to be helpful in areas other than drug delivery. It is already being used in diagnostics. People with diabetesemploy reverse iontophoresis to test their glucose levels noninvasively.
It is being researched to develop a diagnostic test for phenylketonuria, a potentially deadly metabolic disorder in babies. The approach may also be used to evaluate vascular functioning. Opponents of iontophoresis contend that electroporation, rather than iontophoresis, is a superior option for active drug delivery in termsof safety and effectiveness.
It also has more potential than micro-conduit technology, which employs the targeted impact of high-energy micro-particles on specific portions of the skin's surface to form holes for non-invasive analyte and drug administration sampling.
The electroporation method, which requires significantly greater voltage, i.e., 100-1000V, might cause dangerous side effects and is likely to be used in specialist healthcare, while hi-tech micro-conduits technology is still in its infancy.
On the other hand, iontophoretic systems utilizing modest levels of power may be built with a 9-volt button battery and readily marketed. Cardiovascular agents have a guaranteed market for transdermal products due to their necessity for chronic administration. Because of the advanced status of research in this sector, iontophoretic delivery of such medications is expected to become a reality in the near future.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles
