Mucinus Producing Hepatic Cystic Lesions Radiology – What Are They? Diagnosis And Treatment
Mucinus producing hepatic cystic lesions radiology have differing malignant potential, therapy, and prognosis.
Author:Suleman ShahReviewer:Han JuJul 06, 202230 Shares553 Views
Mucinus producing hepatic cystic lesions radiologydemonstrates it is critical to distinguish mucinous cystic neoplasm of the liver from the intraductal papillary tumor of the bile duct from more frequent cystic hepatic masses because they have different malignant potential, therapy, and prognosis.
Mucinous cystic neoplasm of the liver (MCN) and intraductal papillary neoplasm of the bile duct (IPNB) are uncommon and different entities with discrete clinical, pathologic, and imaging characteristics. The presence of subepithelial ovarian-like hypercellular stroma (OLS), the distinguishing histopathologic hallmark of MCN, distinguishes them pathologically.
MCN is a benign, giant, solitary, symptomatic, multiloculated cystic tumor that often arises in middle-aged women. On the other hand, NBC is a diverse spectrum of tumors that are usually linked with invasive carcinoma, occurs in older individuals, and may be distinguished from MCN by contact with the biliary tree, intraductal masses, concomitant biliary ductal dilatation, and the absence of OLS.
Understanding these rare neoplasms has grown and evolved and continues to do so today. Still, uncertainty and controversy persist due to the tumors' rarity, relatively recent designation as separate entities, inherent clinicopathologic heterogeneity, overlapping imaging features, and the fact that many prior studies likely included MCN and cystic IPNB as a single entity.
Historical discrepancies and nonstandardized terminology have contributed to confusion about these neoplasms. The interpreting radiologist must know these entities to suggest a specific diagnosis or generate a meaningful differential diagnosis in the appropriate setting.
This is especially important because MCN and cystic IPNB have overlapping imaging features with other more common hepatobiliary cystic masses but have different management and prognosis.
Biliary Cystadenoma
Biliary cystadenomas are rare benign cystic liver neoplasms. Biliary cystadenomas mainly affect middle-aged individuals and are more frequent in women. The clinical appearance of biliary cystadenomas varies according to tumor size and location. Symptoms and warning signals may include:
- Obstructive jaundice
- Palpable liver edge
- Mass rising abdominal girth
- Right upper quadrant discomfort (large tumors)
- Vomiting and nausea
Biliary cystadenomas are cystic neoplasms that may be unilocular or multilocular. They are only sometimes detected in the extrahepatic biliary tree and gallbladder. Cysts bordered with cuboidal or columnar epithelium mimic normal biliary epithelium. Generally, the criteria for cystadenomas are not connected with the bile ducts, and a variable quantity of mucin-producing epithelium is linked with ovarian-type subepithelial stroma.
Biliary cystadenomas may be unilocular or multilocular and vary in size from 3 to 40 cm. Unfortunately, no imaging findings may reliably distinguish biliary cystadenoma from biliary cystadenocarcinoma.
A biliary cystadenoma manifests as a unilocular or multilocular cyst with the increased transmission. The cysts might be entirely anechoic or have low-level echoes from blood products, mucus, or proteinaceous fluid. Mural nodules and papillary projections may also protrude into the cyst lumen. Acoustic shadowing may be seen if septal or wall calcification is present.
Although biliary cystadenomas are benign tumors, they may return after excision and can progress to malignant biliary cystadenocarcinomas.
Mucinous Cystic Neoplasm Of The Liver
Mucinous cystic neoplasms of the liver (MCN-L), also known as cystadenomas or cystadenocarcinomas, are uncommon cystic tumors that develop in the liver parenchyma or, less commonly, in the extrahepatic bile ducts. They are estimated to account for 5% of all liver cysts. MCN-L is distinguished from an intraductal papillary neoplasm of the bile duct (IPNB), intrahepatic cholangiocarcinoma with cystic change, echinococcal cyst, and simple cyst. Microscopic examination for ovarian-type stroma is the only way to distinguish invasive MCNs from non-invasive MCNs. To distinguish MCNs from other cystic liver lesions, an intraoperative sample and frozen section(s) are required. With a proper early diagnosis, the treatment of choice is complete excision, which may result in excellent survival. However, its uncommon occurrence and limited detection usually result in an inaccurate first or delayed diagnosis or misdiagnosis.
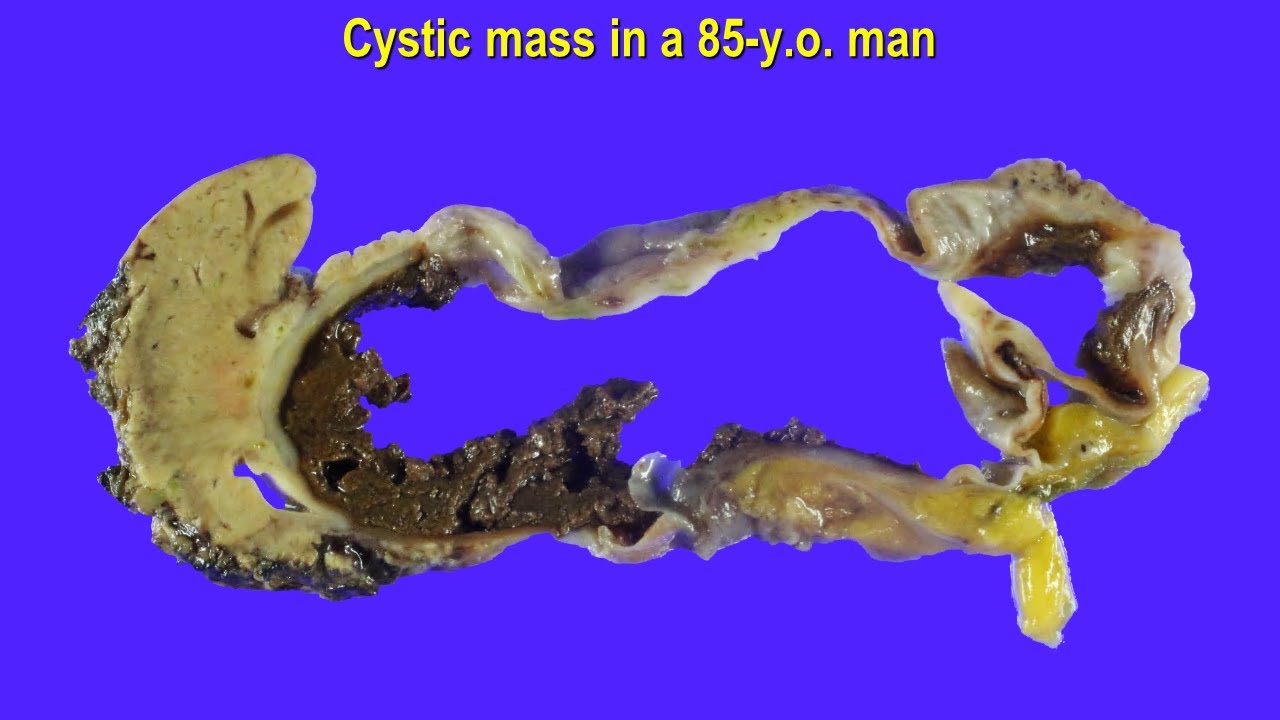
Cystic liver mass: How much does the Gender matter? - Hepatic mucinous cystic neoplasm (MCN)
Hepatic Mucinous Cystic Neoplasm Versus Simple Biliary Cyst
Hepatic cystic lesions are a frequent condition that affects up to 20% of the general population. Mucinous cystic neoplasm of the liver, also known as "biliary cystadenoma," is an uncommon cystic lesion with a 20% chance of malignant progression to mucinous cystic neoplasms with invasive characteristics. Because of the rarity of the lesion, research on hepatic mucinous cystic neoplasms has been limited. Because of the differences in care, presurgical identification of a hepatic mucinous cystic neoplasm from a typical biliary cyst is critical.
MCN recurs in up to 45.6 percent of cases when treated with unroofing and fenestration rather than excision. Other studies have evaluated cyst fluid analysis performance, such as carbohydrate antigen and carcinoembryonic antigen levels.
People Also Ask
Is Biliary Cystadenoma Cancerous?
Mucinous cystic neoplasms (MCNs) are cysts that are not generally malignant but may develop into malignancy. MCNs are often located in the pancreas's body or tail.
What Is Mucinous Cystic Neoplasm With Low Grade Dysplasia?
Mucinous cystic neoplasm (MCN) is an uncommon exocrine pancreatic tumor with four histological forms: noninvasive MCN with low-grade, intermediate-grade, or high-grade dysplasia, and invasive MCN.
What Is A Mucinous Cyst?
Mucinous cystic neoplasms (MCN) are large unilocular or multilocular thick-walled cysts that are often filled with mucinous fluid but may also include hemorrhagic or serous fluid. The cysts in high-grade MCN may have solid patches, mural nodules, or papillary projections.
Are Mucinous Cysts Cancerous?
Biliary cystadenomas develop from the biliary epithelium and often contain a brown or greenish fluid that resembles bile. Because they have the potential to become cancerous, the objective of surgery should be full excision through formal hepatic resection or enucleation.
Conclusion
Mucinous cystic neoplasms of the liver are uncommon cystic tumors that develop inside the liver parenchyma and account for 5% of all liver cysts. Because of its rarity and lack of identification, it usually results in delayed or misdiagnosed diagnoses. Mucinous cystic neoplasms should always be included in the preoperative differential workup of a cystic liver tumor. When the patient is physically suitable for surgery and there is no sign of systemic illness on the first workup, complete excision of a suspected non-invasive or invasive Mucinous cystic neoplasms of the liver is the therapy of choice. As mucinous cystic neoplasms are resected more often, and the proper categorization is used, survival rates and prognosis will become more defined.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles