Ultrasonography - How It Affects The Imaging Of Gouty Arthritis
For gouty arthritis, ultrasonography (US) is a promising new imaging modality. Rheumatologists have become increasingly interested in musculoskeletal ultrasonography (MSKUS) imaging over the last ten years.
Author:Suleman ShahReviewer:Han JuJun 01, 202211 Shares778 Views
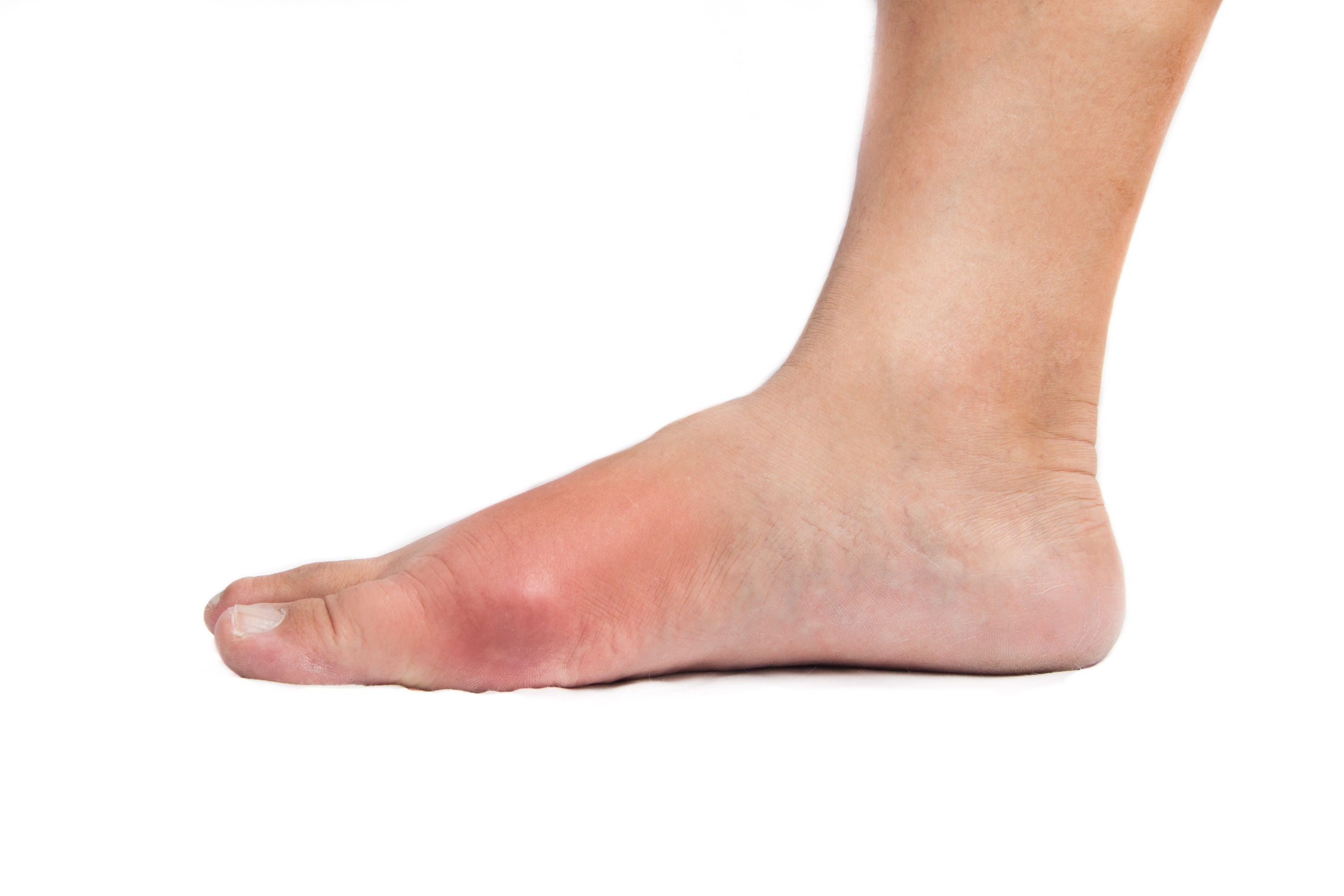
For gouty arthritis, ultrasonography(US) is a promising new imaging modality. Rheumatologists have become increasingly interested in musculoskeletal ultrasonography (MSKUS) imaging over the last ten years.
Ultrasonography is a noninvasive imaging modality for evaluating joints, periarticular tissue, tendons, muscles, bursae, and nerves. Ultrasonography does not emit radiation, is less expensive than CT and MRI, has a high resolution, and can image in multiple planes.
Ultrasonography-guided procedures, such as synovial fluid and tophi aspiration, as well as synovial biopsies, are possible with it.
How Does Ultrasonography Work?
Ultrasonography, also known as sonography or ultrasound, is a diagnostic medical test that creates an image by using high-frequency sound waves to bounce off of body structures.
To send ultrasound waves and listen for an echo, sonography uses a device called a transducer on the skin's surface. The ultrasound waves are then converted into images by a computer. Structures in the image can be seen, measured, and identified by a trained technician. The images are then read by a healthcare provider to assist in the diagnosis of the issue or problem.
A sonogram is a real-time image of what's happening inside the body. To aid in the diagnosis of certain medical conditions, sonography is used to assess the size, shape, and density of tissues. Ultrasound imaginghas long been used to look into the abdomen without having to cut it open.

What is Gout? An Introduction to Gouty Arthritis (1 of 6)
What Is A Gouty Arthritis?
Gouty arthritis, which affects 8.3 million Americans, is the most common type of inflammatory arthritis. Gouty arthritis is caused by the deposition of monosodium urate (MSU) crystals in joints and soft tissues as a result of hyperuricemia. MSU crystals precipitate in joints and soft tissues when serum urate (SU) levels rise above 6.8 mg/dl. MSU crystal deposition can cause inflammationand cause an acute gouty arthritis attack, which is characterized by excruciating pain, tenderness, warmth, swelling, erythema, and loss of function in the affected joint or joints.
Chronic inflammation is frequently present during the intercritical period, even when the patient is asymptomatic. Recurrent acute attacks may become more frequent and severe if MSU crystal deposition and chronic inflammation continue, and a chronic destructive gouty arthritis with disfiguring tophi, joint destruction, and persistent pain may develop.
The rising global prevalence of gouty arthritis emphasizes the importance of identifying patients with the disease early on. Demonstrating the presence of MSU crystals through needle aspiration of joint fluid or tophaceous material (MSU crystal deposits) and polarizing microscopy for MSU crystals is the current gold standard for establishing a definite diagnosis of gouty arthritis.
Because MSU crystals are radiolucent, conventional radiography (CR) is ineffective in detecting early MSU crystal deposition in joints, and soft tissue radiographs of gouty arthritis-affected joints are frequently normal. Only 45% of gouty arthritis patients have radiographic bone changes that are suggestive of the disease.
How Is Gouty Arthritis Diagnosed With Ultrasonography?
Gouty arthritis, both acute and chronic, can be diagnosed with ultrasonography. The use of ultrasonography to diagnose gouty arthritis was found to be a reliable, non-invasive method. According to histopathological studies, gouty arthritis is defined by the crystallization of MSU crystals on hyaline cartilage. The earliest changes of gouty arthritis include such deposition on the surface of hyaline cartilage, along with microtophi. Several ultrasonographic diagnostic features suggestive of gouty arthritis were discovered. A hyperechoic, irregular band over the superficial margin of the articular cartilage, referred to as icing, was found in 92% of gouty joints but not in any of the controls.
Gouty arthritis had the icing, and hypoechoic to hyperechoic, inhomogeneous material surrounded by a small anechoic rim, representing tophaceous material, was only seen in gouty joints and not in any of the controls. In 65% of metatarsophalangeal joints and 25% of MCP joints, erosions were found. In metatarsophalangeal joints that had not previously been affected by an acute gouty arthritis attack, Wright et al. discovered ultrasonography changes suggestive of gouty arthritis.
Does Doppler Ultrasonography Have Any Effect In Gouty Arthritis?
The Doppler method detects red blood cell movement in vessels. With contrasting colors and power, color Doppler ultrasonography detects blood flow direction. The 'power' of the blood flow in the vessel is encoded by Doppler ultrasonography. The fibrovascular matrix vessels become engorged during acute gouty arthritis attacks, producing a positive color and power Doppler signal. Between attacks in chronic tophaceous gouty arthritis, when the patient is usually asymptomatic, ongoing inflammation has recently been discovered.
How Ultrasonography Helps In Treatment
Serial ultrasonography images can be used to evaluate how well anti-inflammatory or urate-lowering therapyis working. Ultrasonography can be used to determine the size of Tophus, and the measurement can be repeated during subsequent patient visits. Changes in tophus size can be observed.The majority of tophi with changes in maximal diameter or volume were in patients with proper serum urate (SU) level control, though changes were also seen in patients with higher SU levels on rare occasions.
MSU deposition on hyaline cartilage can also be affected by urate-lowering therapy changes early on. All gouty arthritis patients exhibit the double contour sign. Urate-lowering drugs influenced the disappearance of the double contour sign once SU levels stayed below ≤6 mg/dl for at least 7 months. At the follow-up, this sign had vanished in patients with SU levels of less than ≤6 ml/dl. Patients who maintained an SU level of 7 mg/dl, on the other hand, did not see the double contour sign disappear.
People Also Ask
Can You Diagnose Gout With Ultrasound?
According to a new study, ultrasound can help distinguish between goutand non-gout. The gold standard for gout diagnosis is the presence of synovial monosodium urate monohydrate (MSU) crystals.
What Imaging Is Used For Gout?
Traditional radiography (CR), ultrasonography (US), computed tomography (CT), dual energy computed tomography (DECT), magnetic resonance imaging (MRI), and nuclear medicine are all imaging modalities that have clinical relevance in gout.
What Is The Role Of Ultrasonography In Assessing Rheumatoid Arthritis?
Rheumatoid Arthritis Patients Undergo Ultrasound Monitoring. Ultrasonogaphy has been shown in several studies to be able to show changes in synovitis and tenosynovitis in RA patients over time.
Can You Diagnose Gout With An X-Ray?
Uric acid crystals could be seen on an x-ray of the joint. X-rays, on the other hand, can be normal even when gout is present. According to experts, chronic gout must be present for 5 to 10 years before x-rays reveal joint changes. A joint fluid analysis is used to diagnose the majority of gout cases.
Conclusion
Ultrasonography imaging of gouty arthritis joints has advanced, indicating new and exciting possibilities in the future. Diagnose gouty arthritis, understand the role of inflammation, and possibly screen a population at risk for preclinical gouty arthritis are just a few of the goals.
Ultrasonography can also be used to assess early gouty arthritis damage and as an outcome measure of the success of anti-inflammatory treatment for acute gouty arthritis, as well as a measure of the success of urate-lowering drugs in reducing joint damage and monitoring therapy response. The role of ultrasonography in gouty arthritis will need to be studied further in the future.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles
