Urachal Cyst – Symptoms, Causes, And Treatment
Urachal cysts may appear at any age, although they are more common in older children and adults.
Author:Suleman ShahReviewer:Han JuJun 24, 2022147 Shares2K Views
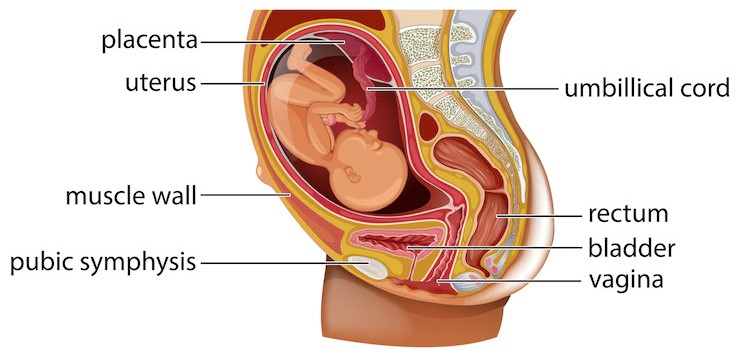
A urachalcystis a sac-like pocket of tissue that forms in the urachus, a structure in the growing infant that links the umbilical cord to the bladder. Although it usually vanishes before birth, some urachus may persist in certain persons.
Urachal cysts may appear at any age, although they are more common in older children and adults. Unless problems, such as infection, urachal cysts are seldom linked with any signs or symptoms. Symptoms in these circumstances may include stomach discomfort, fever, urine pain, and hematuria.
Urachal Abnormalities
During the first trimester of pregnancy, the urachus is a relic of a channel between the bladder and the umbilicus (belly button) via which urine first empties in the baby. Urachus disorders arise when there are problems with the channel's closing off during fetal development. There are at least four different forms of urachal anomalies. The most frequent test for urachal diseases is a CT or MRI scan. A voiding cystourethrogram (VCUG) test is conducted occasionally to confirm that the bladder empties adequately. If an infection accompanies the disease, the infection is generally treated first, followed by urachus excision.
Causes
The urachus is a tube between the fetus's bladder and umbilical cord that permits urine to drain from the fetus during the first trimester.
The urachal channel shuts off during the third trimester and forms the medial umbilical ligament. A urachal cystmay develop if the structure stays open.
Urachal anomalies are infrequent and are often identified by chance during imaging scans and autopsy. They are twice as common in males as in women.
The specific etiology of urachal anomalies is unclear. However, several variables are thought to contribute to their development.
Urachal cysts are a congenital (existing from birth) disorder; thus, there might be a hereditary component. According to specific studies, cysts form due to insufficient development of the urachal region.
Several forms of urachal anomalies may induce postnatal symptoms, including:
- Urachus patent is the remaining connection between the bladder and belly button
- The urachal sinus occurs when the connection between the belly button and the rest of the abdominal area does not seal off
- Diverticulum results after a lack of closure between the belly button and the bladder
Infection may occur with any form of urachal defect. Urachal cyst infections are most frequent in children between two and four.
Urachal abnormalities may not always create symptoms or need therapy. They sometimes go undetected for years and never make any concerns.
Symptoms
Having a urachal cyst does not guarantee that you will have symptoms. Urachal cysts and abscesses typically produce symptoms only if they get infected.
The following are symptoms of an infected urachal cyst:
- Pain in the abdomen
- Fever
- Masses in the abdomen
- Urine pain or burning Frequent urinary tract infections
- Urine with blood
A severe urachal cyst infection might result in more extensive symptoms such as abdominal redness and swelling, acute exhaustion, vomiting, and severe abdominal pain.
Urachal cysts seldom enable the urine to discharge from the belly button.
The drainage in neonates is frequently caused by an issue in the canal that links the bladder and the belly button (urachal sinus). It may result in inadequate umbilical cord repair after delivery.
A urachal cyst draining generates a persistently damp belly button, with a yellow fluid flowing from the stem of the abdominal fold. Skin reddening and a foul odor may develop if not cleaned regularly.
You should seek medical attention if you are suffering signs of an infected urachal cyst. Infected cysts may cause significant healthproblems if not treated.

Urachal cyst (Medical Condition)
Diagnosis
Medical History And Physical Exam
To start the diagnostic procedure, a doctor or other health care practitioner will collect a medical historyby asking questions about the patient's current symptoms and diagnosis. They also often inquire about the patient's prior medical history, medicines, allergies, social background, and family medical history. The doctor may also evaluate a patient's medical records, including the results of previous tests and treatments if they are accessible.
The doctor will examine the patient's body during the physical exam to check for physical symptoms of a medical condition. The procedures utilized during the exam may vary based on the symptoms; however, they usually include:
They examine a person's vital signs, including their temperature, heart rate, breathing rate, blood pressure, weight, and height.
Examining a person's body for average results and alterations that may suggest a diagnosis.
Checking parts of a person's body for discomfort, tenderness, swelling, lumps, masses, or other changes by touching them.
Examining the heart, lungs, or abdominal organs by listening to internal body noises.
Tapping on specific body parts to detect the presence of air, liquid, or solid structures.
Evaluating the nervous system involves testing reflexes, nerves, coordination, sensory, and motor functions, such as strength and balance.
The doctor may then determine if lab tests, imaging investigations, clinical treatments, or referrals to other medical experts are required to diagnose the source of the patient's health concerns based on the medical history and physical exam findings.
Imaging Studies
Diagnostic imaging investigations allow clinicians to see into a patient's body for information that can aid in diagnosing or managing an illness. The kind of imaging scan chosen by a doctor is determined by the patient's symptoms and the portion of the body being studied.
If your doctor suggests an imaging scan, you may find more information on Diagnostic Imaging.
Laboratory Tests
Laboratory tests look for indicators of medical disorders in a sample of a patient's blood, urine, or bodily tissues. The findings or results of lab tests may offer information to a clinician to aid in diagnosing an illness. The lab tests will determine a patient's symptoms and the disorders under consideration.
Fever, pyuria, hematuria, and an increased circulating C-reactive protein concentration are all symptoms of this condition.
Clinical Procedures
Clinical techniques may assist in identifying a diagnosis by measuring biological processes or looking for indicators of illness. Other treatments may be performed to treat or manage symptoms. A doctor's recommendation for clinical therapies will be based on the patient's symptoms and the portion or process of the body being investigated or treated.
Treatment
You don't need to do anything if you have a urachal cyst that isn't creating symptoms. Only if the cyst gets infected would treatment be considered urgent.
Antibiotics are essential in this scenario. The majority of urachal cyst infections may be treated with over-the-counter drugs (oral antibiotics). If the infection is serious, you may require antibiotics administered via a vein in your arm (intravenous).
A surgical removal of an infected urachal cyst is sometimes required. If the surgery may be advised if the cyst causes extensive draining, irritation, pain, and/or recurring infection
The removal of the urachal cyst avoids further infections and lowers the chance of urachal malignancy (a rare bladder cancer).
Similarly, a draining urachal sinus may be removed and closed up (excised) with a minor belly button incision or laparoscopic surgery.
There have been a few occasions when urachal anomalies were cleared independently without therapy.
Because this result is less probable and urachal cysts might create issues, you should consult your healthcare practitioner about the best course of action for your specific circumstance.
People Also Ask
Is Urachal Cyst Cancerous?
Urachal carcinoma is a kind of cancer that develops in the urachus structure. The urachus is a channel that occurs before birth while the fetus grows. This canal connects the fetus's bladder to the belly button (umbilicus). It empties the fetus's urine bladder.
How Common Are Urachal Cysts In Adults?
One in every 5,000 live newborns has a urachal cyst. It is mainly asymptomatic, with around 35% of patients presenting with lower abdomen discomfort, urinary tract infection symptoms, a painful abdominal mass, and hematuria.
How Do You Treat An Urachal Cyst?
Urachal cysts are treated by removing the cyst entirely. However, the typical treatment of an infected urachal cyst consists of a two-stage procedure that includes an incision, draining the infected cyst, and secondary excision.
Is Urachal Cyst Serious?
People may spend their whole lives with urachal cysts without recognizing them since they seldom cause difficulties. However, cyst drainage might cause pain or other symptoms. Infections are also possible. An infected urachal cyst is a dangerous ailment that requires immediate medical attention.
Final Words
You might spend your whole lifewith a urachal cyst and never have any problems. You may not even be aware that you have one.
However, if the cyst gets infected, it might cause significant medical complications.
Seek medical attention immediately if you experience signs of an infected urachal cyst, such as sudden or severe stomach discomfort.
Proper treatment is required to avoid problems or future concerns caused by the cyst. Most infections may be treated with medications, but in other circumstances, a doctor may opt to remove the cyst surgically.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles
