The Effects Of Cannabis On Antibiotic-Resistant Bacterial Infections
Antibiotic-resistant bacteria are now one of the top health concerns of the world and using cannabis as a treatment for antibiotic-resistant bacterial infections has just gained recognition. Infections that were formerly thought to be easily curable can now be fatal. Thousands of people die each year as a result of methicillin-resistant Staphylococcus aureus (MRSA).
Author:Suleman ShahReviewer:Han JuApr 11, 202212 Shares298 Views
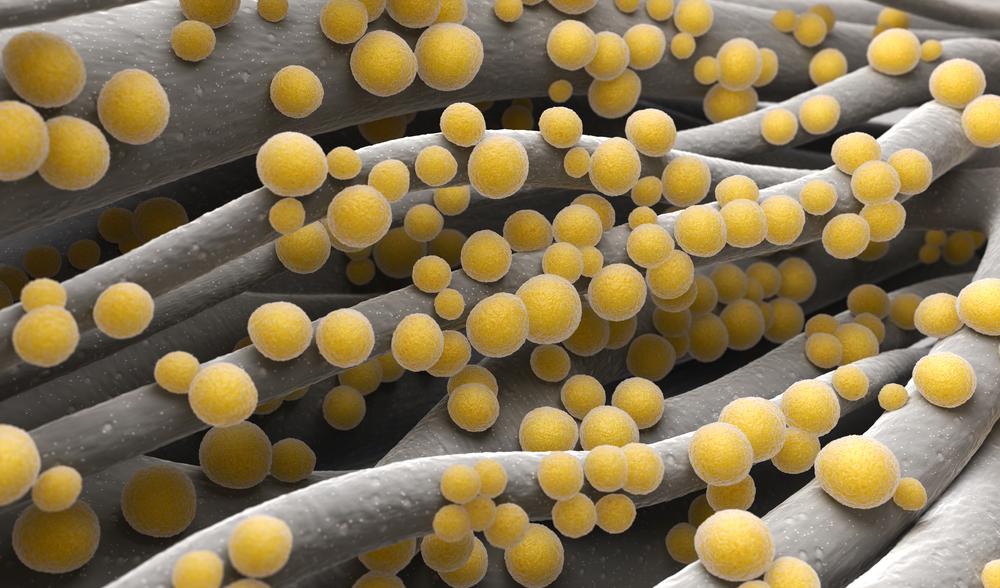
Antibiotic-resistant bacteria are now one of the top healthconcerns of the world and the effects of cannabis on antibiotic-resistant bacterial infectionshas just gained recognition. Infections that were formerly thought to be easily curable can now be fatal. Thousands of people die each year as a result of methicillin-resistant Staphylococcus aureus (MRSA).
People with low immune systems are the most vulnerable, but even healthy people can become sick if they are exposed to the bacteria. In 2014, President Barack Obama signed an executive order and appropriated funds for the creation of a special task force to address the issue, with the goal of developing an action plan to combat the rapid spread of antibiotic-resistant germs such as MRSA.
What Is Antibiotic Resistance?
Antibiotic resistance occurs when bacteria (germs) develop resistance to antibiotics that are intended to kill them. Antibiotic resistance has been linked to misuse and overuse of these drugs, which has been identified as a serious threat to public health by international health agencies.
Antibiotics are no longer as efficient in preventing illness when a person is infected with antibiotic-resistant bacteria. This complicates treatment and raises the danger of the infection spreading to individuals who are resistant to antibiotics.
Experts have discovered ways to help prevent antibiotic resistance from becoming a bigger problem.
What Are Antibiotic-Resistant Bacterial Infections?
Antibiotic-resistant bacteria are microorganisms that cannot be controlled or destroyed by antibiotics. When bacteria adapt or alter in such a way that antibiotics become less effective, resistance develops.
Antibiotic resistance develops naturally as bacteria evolve and create defense mechanisms to adapt to a changing environment, but researchers believe that antibiotic abuse is hastening the process.
Bacteria that cause skin infections, urinary tract infections, meningitis, sexually transmitted diseases (STDs), and respiratory tract infections including pneumonia are becoming increasingly resistant to antibiotics.
Antibiotic resistance develops in germs, not people. Antibiotic resistance, in other words, does not imply that the human body develops resistance to antibiotics. This indicates that the bacteria are antibiotic-resistant.
Prevention
Antibiotic-resistant bacteria can cause infections that are difficult to treat and affect almost anyone. While eradicating antibiotic resistance is unlikely, there are steps that may be taken to assist prevent the problem from worsening.
Antibiotic overuse should be avoided, bacterial infections should be stopped, foods should be carefully selected, food should be handled and prepared securely, and antibacterial home products should be used with caution.
Unnecessary Medication Should Be Avoided
Antibiotic resistance is largely caused by overprescribing antibiotics. Antibiotics can save people's lives when they are infected with bacteria. However, they are frequently prescribed and used for viral diseases such as colds, coughs, the flu, and viral sore throats that are not necessary.
By following these guidelines, you can minimize unnecessary antibiotic prescriptions:
- If you have a virus, you shouldn't take antibiotics (such as a cold or the flu).
- Antibiotics should never be saved for later use.
- Never take an antibiotics that someone else has prescribed for you.
- Follow the directions on your medicines exactly.
Stop Bacterial Infection From Spreading
Antibiotic-resistant bacteria spread in the same way that other bacteria do: by contact with an infected person, exposure to germs in the environment, or consumption of contaminated food or water.
In general, there are several good hygiene behaviors that can help you avoid illnesses and prevent the development of antibiotic-resistant microorganisms, such as:
- Using soap and water to clean your hands.
- When sneezing or coughing, cover your mouth and nose.
- Maintaining the cleanliness and protection of your wounds or cuts.
- To avoid foodborne diseases, properly prepare and handle food.
- By practicing safe sex, you can avoid sexually transmitted infections (STDs).
Antibiotic-Raised Meat Should Be Eliminated
Antibiotic-resistant bacteria can spread not only from person to person, but also from animal to animal and through the food supply. Antibiotic resistance is a contributing factor, according to experts, in agricultural animals. Due to interaction with livestock manure and wastewater, these bacteria can contaminate other items.
As a result, scientists stress the necessity of avoiding antibiotic-affected meat wherever feasible. Look for phrases like "grown without antibiotics," "no antibiotics administered," and "organic" on the product label.
You could also try reducing or eliminating meat from your diet.
Antibiotic-Resistant Bacterial Infections And The Effects Of Cannabis
Cannabis has been successfully utilized and studied in the treatment of different bacterial illnesses on a regular basis. THC and CBDwere found to be beneficial against staph and strep infections in 1976 research. Oral CBD preparations, for example, can be utilized to treat oral infections as systemic antibacterial agents.
Pinene has also been demonstrated to be as effective as vancomycin and other antimicrobials in treating MRSA. Pinene can help improve skin permeability, which is a major obstacle to phytocannabinoids absorption.
In the fight against MRSA and other treatment-resistant bacteria, combining CBD/CBG-based extracts with pinene could be fruitful. "The most practical application of cannabis in a hospital environment would be as topical treatments to heal ulcers and wounds, reducing the load of antibiotics," said Giovanni Appendino, a professor at Italy's Piemonte Orientale University and co-author of the 2008 study.
How To Take The Medicine - Dosage And Delivery
Patients should collaborate with a healthcare professional who has experience recommending CBD or medicinal cannabis to establish and fine-tune dosage and delivery methods on an individual basis. At the same time, well-informed patients can act as their own health consultants.
CBD-dominant cannabis or other strains can be used to make topical treatments that are applied to the skin. When germs infect the skin or a wound site, this procedure is used. THC-containing topical treatments affect cells nearby but do not cross the blood-brain barrier, making them non psychoactive. These products can come in a variety of forms, including oils, ointments, sprays, and other forms, with various CBD and THC ratios (a ratio of 1:1 is often recommended as ideal for skin application).
CB2 receptors are found in the greatest number and concentration in the skin. Products containing any of the primary cannabinoids can be effective against an antibiotic-resistant infection, according to the 2008 study mentioned above in this section.
Final Words
Antibiotics have saved many lives, yet they can contribute to the development and spread of antibiotic resistance if they are used excessively. Antibiotic resistance, according to the World Health Organization, results in longer hospital admissions, higher medical costs, and more bacterial infection-related fatalities.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles

