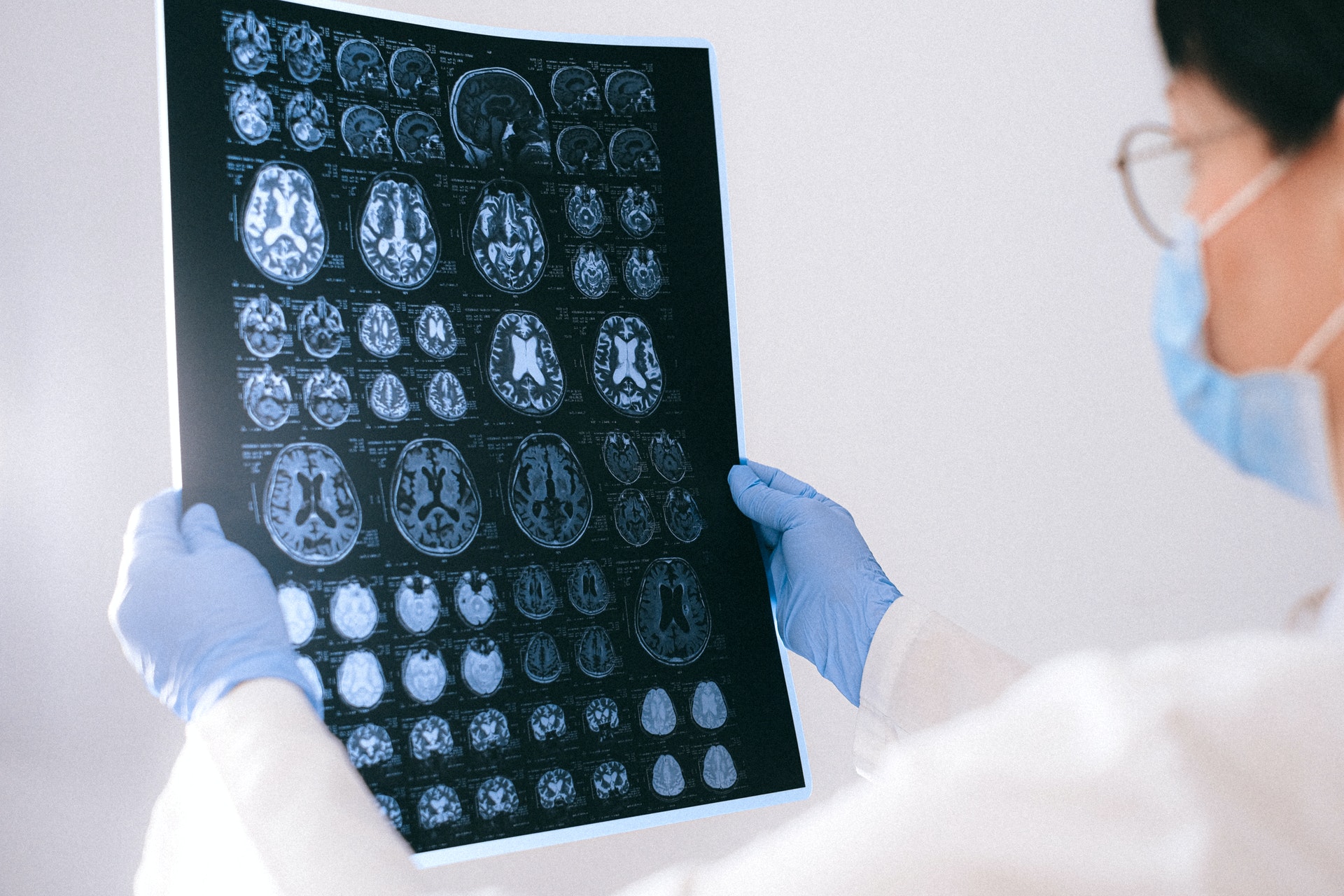
Dynamic Contrast Enhanced - What The Heck Is It And How Will It Change Healthcare?
Dynamic contrast enhanced (DCE) is one of the primary MRI perfusion approaches, which determines perfusion parameters by analyzing T1 shortening.
Author:Suleman ShahReviewer:Han JuMay 28, 202316.6K Shares475.1K Views

Dynamic contrast enhanced(DCE) is one of the primary MRI perfusion approaches, which determines perfusion parameters by analyzing T1 shortening caused by a gadolinium-based contrast bolus flowing through tissue.
K-trans is the most usually computed parameter.
Dynamic Contrast Enhanced MRI
In oncology, dynamic contrast-enhanced magnetic resonance imaging (DCE-MRI) is a noninvasive approach for assessing tumor microvasculature qualities.
DCE-MRI has the potential to be employed as an imaging biomarker to assess the antiangiogenic effects of cancer therapy.
This article highlights current data, limitations to using DCE-MRI for treatment response evaluation in clinical trials, and the basic approach to doing DCE-MRI.
Difference Between Dynamic Contrast Enhanced And Dynamic Susceptibility Contrast In Imaging
Dynamic contrast enhanced imaging evaluates T1 tissue changes over time after gadolinium bolus injection.
It varies from dynamic susceptibility contrast imaging because it monitors T2 and T2* changes.
Gadolinium contrast agents remain in plasma immediately after injection and are circulated to organs according to blood flow.
Because of their tiny molecular size (5001000 Da), these medicines may pass past the vascular endothelium and into the extracellular space of most tissues through passive diffusion.
The brain and spinal cord are the sole exceptions, where tight endothelial junctions form a blood-brain barrier (BBB) that prevents this process.
When the BBB is damaged by a tumor, infection, or other illness, gadolinium accumulates, causing T1-shortening and contrast enhancement.
The primary purpose of dynamic contrast enhanced imaging is to observe and measure the temporal course of this contrast enhancement.
Generally, the degree of contrast enhancement is determined by regional blood flow, the size and number of blood vessels measured by surface area per unit mass of tissue, and leakiness or permeability.
Although it is not feasible to separate the F, P, and S components separately, we may assess their total influence by mathematical modeling, represented in the so-called transfer constant (Ktrans).
Ktrans is a measure of the diffusion of gadolinium contrast through the vascular endothelium.
Ktrans and other dynamic contrast enhanced-derived indices have become more relevant in assessing tumor response to treatment, particularly for non-cytotoxic medicines that target tumor vascularity.
In addition to Ktrans, dynamic contrast-enhanced can estimate the volume fraction of extravascular extracellular space (ve) in tissue, the volume fraction of plasma in tissue (VP), and the rate constant for gadolinium contrast efflux back into plasma from the extracellular tissue space.
Dynamic Contrast Enhanced CT
Dynamic contrast enhanced (DCE) imaging entails acquiring a baseline image(s) without contrast enhancement, followed by a series of pictures taken over time after an intravenous bolus of a conventional contrast agent.
A contrast agent inside cerebral blood vessels and tissues has a linear effect on observed X-ray attenuation on CT and a non-linear effect on computed signal intensity on MRI.
Deconvolution analysis may properly handle images recorded for compartmental analysis.
There is no agreement on which perfusion CT approach is best for assessing tumor vascularity.
Software solutions for DCE-CT data processing often incorporate automated or semi-automatic techniques for identifying specific structures to increase findings' accuracy and repeatability.
Using attenuation thresholds on baseline pictures, brain tissue may be easily differentiated from non-cerebral tissues, while arterial input and sagittal sinus can be segregated from contrast-enhanced images.
The primary benefit of DCE-CT over MRI is its ease of capture and processing.
CT's high spatial resolution allows for precise identifying areas of interest and produces high-resolution parametric pictures.
It may also be done using combined PET/CT systems, which allow for simultaneous evaluation of tumor vascularity and glucose metabolism.
This combined data provides fresh insights into tumor pathogenesis and can predict tumor aggressiveness.
People Also Ask
What Is Enhanced MRI?
Gadolinium-based chemicals are the most often utilized contrast enhancers.
Following oral or intravenous injection, these MRI contrast agents reduce the relaxation times of nuclei inside human tissues.
What Is Contrast Enhanced CT Scan?
Contrast CT, also known as contrast enhanced computed tomography (CECT), is a kind of X-ray computed tomography (CT) that employs radiocontrast.
Iodine-based radio contrasts are often used in X-ray CT.
This is beneficial for highlighting features like blood vessels that would otherwise be difficult to distinguish from their surroundings.
What Is Dynamic Contrast Enhancement In MRI?
Dynamic contrast-enhanced MR perfusion is one of the primary techniques used for MRI perfusion.
This technique calculates perfusion parameters by evaluating the T1 shortening induced by a gadolinium-based contrast bolus passing through tissue. Permeability MRI is another name for this technique.
What Is Dynamic Contrast Enhanced CT?
During the dynamic contrast enhanced-CT procedure, the patient is instructed to hold their breath after receiving an intravenous bolus of iodinated contrast medium at a concentration of 300 mg/ml injected at a rate of 2 ml/sec.
This is followed by acquiring a dynamic series of short spiral acquisitions centered on the SPN.
The contrast substance's volume will be 1.4 milliliters per kilogram.
Conclusion
The T1-shortening effects of gadolinium-based contrast agents are essential to the operation of dynamic contrast enhanced.
After administering an intravenous contrast bolus, fast repetitive imaging with the T1 sequence is performed.
Regional enhanced signal (T1 shortening) is due to gadolinium concentration, which in turn will rely on several factors: intravascular gadolinium (also known as actual perfusion) and accumulation of gadolinium in the extravascular space (also known as permeability).

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles