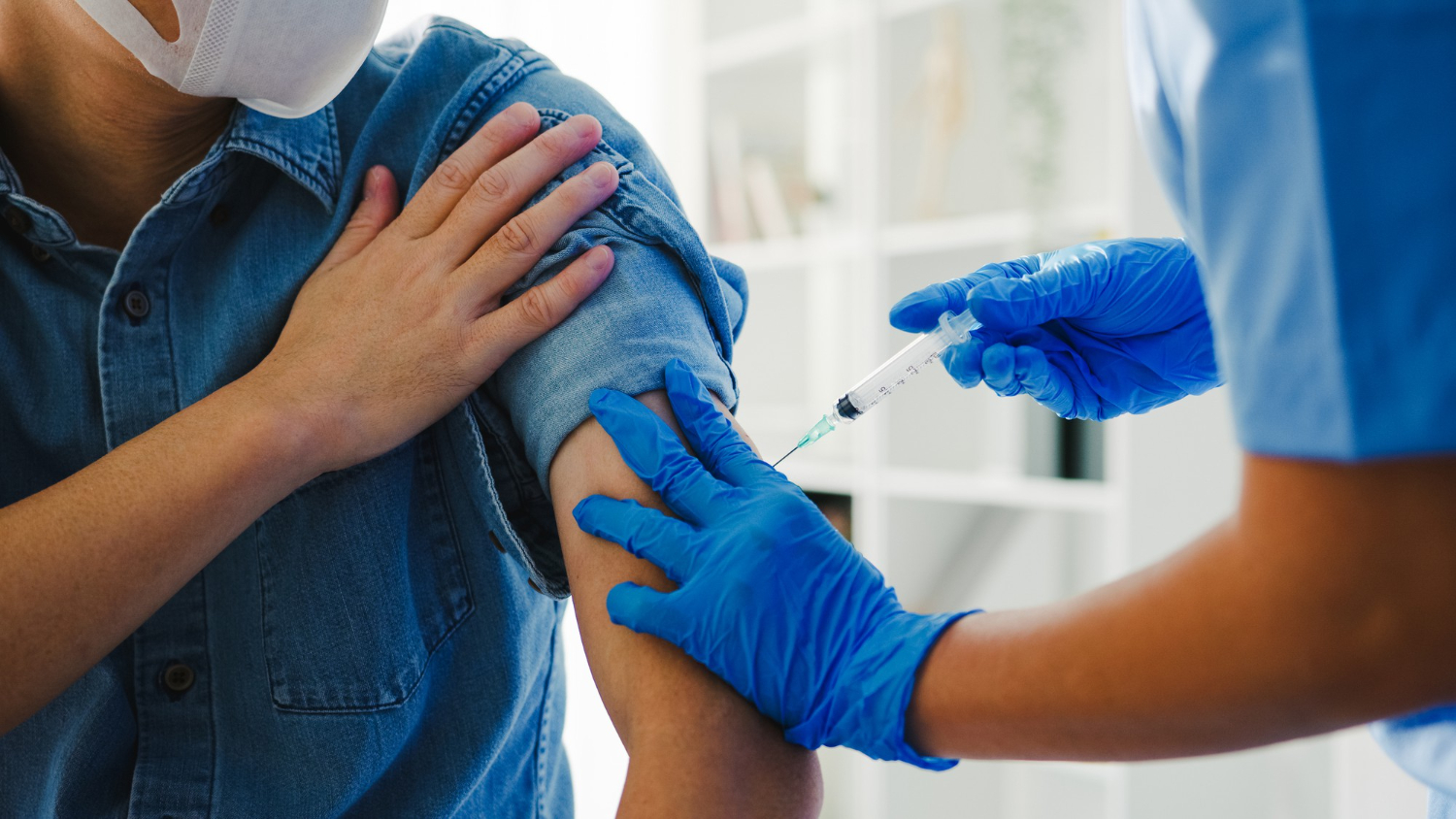
Regadenoson – Overview Of Its Uses And Mechanism Of Action
Regadenoson is an A2A adenosine receptor agonist that produces coronary vasodilation and is a pharmacologic stress agent suggested for radionuclide myocardial perfusion imaging (MPI) in individuals unable to exercise enough. This medication works by dilating the arteries in the heart and increasing blood flow to aid in diagnosing coronary artery disease.
Author:Suleman ShahReviewer:Han JuAug 09, 20220 Shares114 Views
Regadenosonis an A2A adenosine receptor agonist that produces coronary vasodilation and is a pharmacologic stress agent suggested for radionuclide myocardial perfusion imaging (MPI) in individuals unable to exercise enough.
This medication works by dilating the arteries in the heart and increasing blood flow to aid in diagnosing coronary artery disease. This medication should only be administered by or under the direct supervision of a doctor. Astellas manufactures it, and the FDA authorized it on April 10, 2008.
Regadenoson Mechanism Of Action
Regadenoson is a selective low-affinity (Ki= 1.3 M) A2A receptor agonist that mimics adenosine's effects on coronary vasodilation and myocardial blood flow.
It is an extremely weak A1 adenosine receptor agonist (Ki > 16.5 M). It also has a low affinity for A2B, and A3 adenosine receptors. Regadenoson is being tested in pharmacological stress testing.
In individuals with paroxysmal supraventricular tachycardia (PSVT), particularly PSVT associated with Wolff-Parkinson-White Syndrome, adenosine reduces conduction time through the A-V node, may inhibit reentry routes via the A-V node, and can restore normal sinus rhythm.
Regadenoson Uses
Regadenoson is exclusively for diagnostic purposes. Its treatment is only permitted in medical facilities equipped with cardiac monitoring and resuscitation equipment.
Regadenoson is a selective coronary vasodilator approved for use as a pharmacological stress agent in humans for:
- Myocardial perfusion imaging (MPI) in individuals unable to tolerate appropriate exercise stress.
- The assessment of a single coronary artery stenosis's fractional flow reserve (FFR) during invasive coronary angiography when repeated FFR measurements are not expected.
Regadenoson Dose
A single injection of 400 micrograms of regadenoson (5 ml) into a peripheral vein is advised, with no dosage modification required for body weight.
Patients should refrain from consuming methylxanthines (e.g., coffee) or theophylline-containing products for at least 12 hours before regadenoson administration.
Dipyridamole should be avoided for at least two days before regadenoson administration if feasible. Aminophylline may reduce severe and/or long-lasting adverse responses to regadenoson. However, it should not be taken only to stop a seizure caused by regadenoson.
Regadenoson elevates the heart rate quickly. Patients should sit or lie down following the injection and be monitored at regular intervals until the ECG parameters, heart rate, and blood pressure have reverted to pre-dose values.
This medication should only be used once during 24 hours for MPI. The safety and tolerability of using this medicine again within 24 hours have not been determined.
This product should be given no more than twice in 24 hours, no less than 10 minutes apart. Complete safety data for the second regadenoson injection are unavailable when given twice 10 minutes apart in 24 hours.
Regadenoson's safety and effectiveness in children under 18 have yet to be proved.
No need to alter the dosage for the elderly, hepatic impairment, or renal impairment.
Regadenoson Administration
For intravenous administration.
Myocardial Perfusion Imaging (MPI)
- Regadenoson should be injected into a peripheral vein in a 10-second burst using a 22-gauge or larger catheter or needle.
- 5 mL of sodium chloride 9 mg/mL (0.9 percent) injectable solution should be given immediately after the regadenoson injection.
- The MPI acquisition methodology must adhere to clinical practice recommendations.
Fractional Flow Reserve (FFR)
- Regadenoson should be delivered as a quick 10-second injection into a peripheral vein using a 22-gauge or larger catheter or needle.
- 10 mL of sodium chloride 9 mg/mL (0.9 percent) injectable solution should be given immediately after the regadenoson injection.
- FFR should be calculated as the lowest Pd/Pa value obtained during steady-state hyperemia.
Regadenoson Warnings And Precautions
Regadenoson has the potential to produce significant and perhaps fatal responses, such as those described below.
Continuous ECG and vital signs monitoring should be conducted until the ECG parameters, heart rate, and blood pressure revert to pre-dose values.
Regadenoson should be used with care and only in a medical center equipped with cardiac monitoring and resuscitation equipment.
Aminophylline may be given in dosages ranging from 50 mg to 250 mg via gradual intravenous injection (50 mg to 100 mg over 30-60 seconds) to reduce severe and/or long-lasting adverse responses to regadenoson.
However, it should not be used only to stop a seizure caused by regadenoson.
- Myocardial Ischemia: Ischemia caused by pharmacologic stress agents such as regadenoson may result in fatal cardiac arrest, life-threatening ventricular arrhythmias, and myocardial infarction. Regadenoson should be taken with care in individuals who have recently had a myocardial infarction. Patients with recent (within three months) myocardial infarction were excluded from Single Photon Emission Computed Tomography (SPECT) myocardial perfusion imaging (MPI) clinical studies using regadenoson. Patients having an acute myocardial infarction or within five days of an acute myocardial infarction were excluded from clinical studies for FFR assessment.
- Atrioventricular and Sinoatrial nodal obstruction:Regadenoson and other adenosine receptor agonists may depress the sinoatrial (SA) and AV nodes, resulting in first, second, or third-degree AV block or sinus bradycardia.
- Hypotension:Regadenoson and other adenosine receptor agonists cause arterial vasodilation and hypotension. Autonomic dysfunction, hypovolemia, left main coronary artery stenosis, stenotic valvular heart disease, pericarditis or pericardial effusions, or stenotic carotid artery disease with cerebrovascular insufficiency may increase the risk of significant hypotension.
- High blood pressure:Regadenoson may produce clinically substantial rises in blood pressure, which can lead to hypertensive crisis in certain people. Patients with uncontrolled hypertension may be at greater risk of significant blood pressure rises. Delaying regadenoson administration until blood pressure is effectively regulated might be considered.
- Combination with physical activity:The use of regadenoson during exercise has been linked to significant side effects such as hypotension, hypertension, syncope, and cardiac arrest. Patients with symptoms or indications of acute myocardial ischaemia during exercise or recovery are at an increased risk of significant adverse events.
- Ischaemic stroke and cerebrovascular accident:Regadenoson has the potential to trigger a transient ischemic attack. There have also been cerebrovascular accidents in post-marketing experience (CVA).
- Seizure danger:When delivering regadenoson to patients with a historyof seizures or other risk factors for seizures, such as the concurrent administration of seizure-lowering medications, extreme caution should be used (e.g., antipsychotics, antidepressants, theophyllines, tramadol, systemic steroids, and quinolones). Because of its proconvulsant activity, aminophylline should be taken with care in individuals with a history of seizures or other risk factors for seizures. It may prolong a seizure or produce several seizures. As a result, using aminophylline merely to stop a seizure caused by regadenoson is not suggested.
- Flutter or atrial fibrillation:In individuals with a history of atrial fibrillation or flutter, regadenoson should be administered with care. There have been occurrences of atrial fibrillation worsening or recurrence following regadenoson medication in post-marketing experience.
- Bronchoconstriction:Regadenoson may induce bronchoconstriction and respiratory arrest, particularly in individuals with bronchoconstrictive illness, chronic obstructive pulmonary disease (COPD), or asthma. Before regadenoson administration, adequate bronchodilator treatment and resuscitation procedures should be provided.
- QT prolongation syndrome:In individuals with long QT syndrome, regadenoson enhances sympathetic output and may increase the incidence of ventricular tachyarrhythmias.
- Excipient-related cautions:Each dosage of this medication includes less than 1 mmol sodium (23 mg). The injection of sodium chloride 9 mg/ml (0.9 percent) solution administered following regadenoson, on the other hand, includes 45 mg of sodium. Patients on a low salt diet should take this into account.
Regadenoson Contraindications
Regadenoson has a high safety profile; however, it is completely contraindicated in patients with second-degree AV block, third-degree AV block, sinus node disease without a functioning pacemaker, a bronchospastic disease with active wheezing, hypotension (systolic blood pressure less than 90 mm Hg), uncontrolled hypertension (systolic blood pressure greater than 200 mmHg or diastolic blood pressure greater than 110 mm Severe sinus bradycardia (heart rate less than 40 beats/min), Mobitz type 1 2nd degree AV block, ingestion of caffeine-containing drinks or foods within 12 hours, history of seizure disorder (regadenoson may lower seizure threshold), and severe aortic stenosis are relative contraindications to regadenoson stress testing.
Regadenoson Side Effects
A drug may have inevitable unintended consequences in addition to its intended benefits. Although not all of these side effects are possible, they may need medical treatment if they occur.
If any of the following side effects occur, contact your doctor or nurse right away:
More Common Side Effects
- Pain in the arm, back, or jaw
- Chest pain or discomfort
- Difficult or strained breathing
- rapid or irregular pulse
- Nausea
- Sweating
- Chest tightness
Overdose Symptoms
If any of the following overdose signs occur, seek urgent medical attention:
- Dizziness
- The sensation of warmth
- Elevated heart rate.
- face, neck, arms, and, on rare occasions, upper chest redness
Mild Side Effects
Some side effects may develop that might not need medical treatment. These side effects may subside as your body responds to the medication. Your doctor may also be able to advise you on how to avoid or mitigate some of these side effects. Consult your doctor if any of the following side effects persist or become bothersome or if you have any concerns about them:
- Headache
- Flavor change
- Loss of taste
- Stomach ache
- Discomfort
- Diarrhea
- Difficulty with moving joint pain
- Aching or cramping muscles
Other side effects that have not been described may occur in some people. Check with your doctor if you detect any additional side effects.
Regadenoson Adverse Reactions
The most prevalent adverse responses to Lexiscan in clinical studies (5 percent) were dyspnea, headache, flushing, chest discomfort, angina pectoris or ST-segment depression, dizziness, chest pain, nausea, and stomach discomfort, dysgeusia, and feeling overheated.
Most adverse events occurred shortly after dosage and typically dissipated within 15 minutes, except for headache, which cleared in most patients within 30 minutes. In 3% of patients, aminophylline was employed as a reversal medication.
Supraventricular tachyarrhythmias, acute coronary syndrome (ACS), tremor, QTc prolongation, stomach discomfort associated with nausea, vomiting, myalgias, diarrhea, fecal incontinence, wheezing, and musculoskeletal pain have all been reported in postmarketing experience.
People Also Ask
What Class Drug Is Regadenoson?
Regadenoson is a member of the Diagnostic Imaging Agents family of medicines.
Is Regadenoson The Same As Adenosine?
In animals, regadenoson is a more effective vasodilator than adenosine and prefers coronary circulation over renal, peripheral, and mesenteric circulations. Adenosine has a nonselective action on A1 receptors, causing adverse chronotropic, dromotropic, and inotropic effects.
Is Regadenoson The Same As Lexiscan?
Lexiscan® injection contains regadenoson, a pharmacologic stress agent used in radionuclide myocardial perfusion imaging (MPI) in patients unable to exercise enough.
What Is Regadenoson Used For?
In individuals unable to endure appropriate exercise stress, regadenoson injection is utilized as a pharmacologic stress agent for radionuclide myocardial perfusion imaging (MPI). This medication works by dilating the arteries in the heart and increasing blood flow to aid in diagnosing coronary artery disease.
Bottomline
It is essential to thoroughly investigate the patient's profile to establish the most suitable stress test and assess the safety profile of utilizing the regadenoson pharmacological stress test in specific patient groups. Compared to apadenoson and binodenoson, Regadenoson may have the least selectivity and affinity for A2A receptors. However, its brief duration of action and lack of weight changes underline its advantage over the other agents.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles