Q Waves - A New Shift In ECG For Heart Problems
The Q waves indicate the interventricular septum's first depolarization and are defined as the first negative deflection after the P wave and occurring before the R wave.
Author:Suleman ShahReviewer:Han JuAug 06, 202228 Shares725 Views
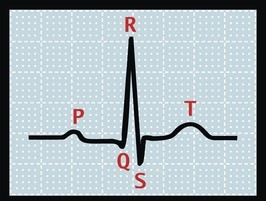
The Q wavesindicate the interventricular septum's first depolarization and are defined as the first negative deflection after the P wave and occurring before the R wave.
A Q waveon an electrocardiogram (ECG) is an initially negative deflection of the QRS complex. A Q wave technically signifies that the net direction of early ventricular depolarization(QRS) electrical forces is pointing toward the negative pole of the lead axis.
Although strong Q waves are a hallmark of myocardial infarction, they may also be seen in various noninfarct conditions. Failure to recognize the different origins of Q waves might result in significant diagnostic mistakes.
A Q wave does not suggest any particular electrophysiological process. However, Q waves may be linked to one or more of the following factors:
- Effects of physiology and place
- Myocardial damage or replacement
- Ventricular hypertrophy
What Is A Q Wave?
The QRS complex begins with the Q wave, the first downward deflection following the P wave.
There is no Q wave when the initial deflection of the QRS complex is vertical. In many, but not all, ECG leads, a typical person will have a modest Q wave. Q wave abnormalities are usually suggestive of myocardial infarction.
"Q wave myocardial infarction" and "non-Q w.ave myocardial infarction" were formerly used to describe various kinds of myocardial infarctions that resulted in either Q wave development or the lack of Q wave development.
- A Q wave is a negative deflection before the R wave.
- The Q wave indicates the interventricular septum's usual left-to-right depolarization.
- Small 'septal' Q waves are often seen in the left-sided leads (I, aVL, V5 and V6)
- In most leads, little Q waves are typical.
- As a typical variation, deeper Q waves (>2 mm) may be found in leads III and aVR.
- Q waves are not often seen in the right-sided leads (V1-3)

Q Wave
Pathologic Q Waves
Pathologic Q waves indicate a prior myocardial infarction. A lack of electrical activity causes them. A myocardial infarction may be seen as an electrical 'hole' since scar tissue is electrically dead, resulting in pathologic Q waves.
Pathologic Q waves are not an early indicator of myocardial infarction; they often develop over many hours to days. Once pathogenic Q waves have formed, they seldom disappear.
If the myocardial infarction is reperfused early (for example, percutaneous coronary intervention), shocked myocardial tissue may recover, and pathologic Q waves dissipate. In all other cases, they usually last eternally.
The exact definition of pathologic Q waves has been questioned. The most recent report, adopted by the ESC and ACC, is shown below.
A pathologic Q wave is defined as
- Any Q-wave in leads V2-V3 ≥0.02 s or QS complex in leads V2 and V3
- Q-wave ≥0.03 s and > 0.1 mV deep or QS complex in any two leads in a contiguous lead grouping (I, aVL, V6; V4-V6; II, III, and aVF)
- In the absence of a conduction defect, R-wave ≥0.04 s in V1-V2 and R/S 1 with a concordant positive T-wave
Q waves are deemed pathological if the following conditions are met:
- > 40 ms (1 mm) broad
- > 2 mm deep
- > 40 ms (1 mm) broad
- seen in leads V1-3
- Pathological Q waves generally imply a recent or previous myocardial infarction.
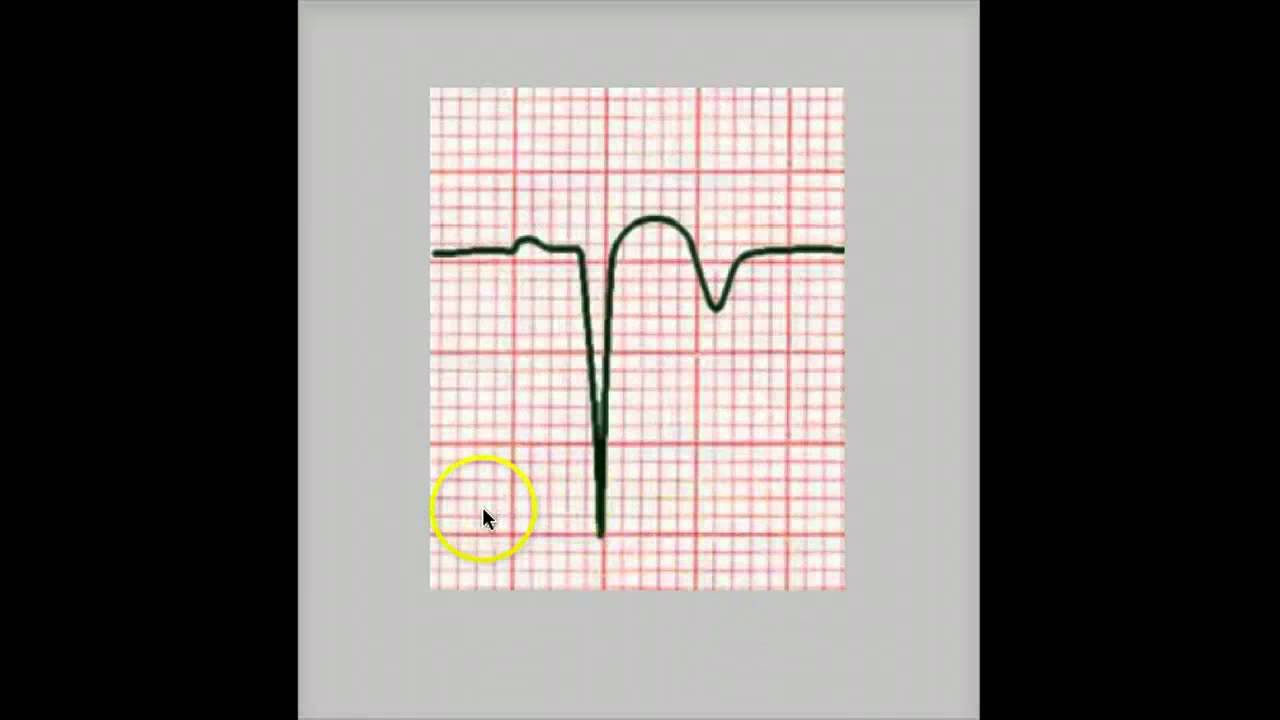
PATHOLOGIC Q WAVE
Q Waves In Lead III
The initial forces that come from depolarization of the interventricular septum from left to right are responsible for the usual Q wave in lead I (a horizontal lead) and either an initial R or Q wave in the lead III (a lead with a dominantly vertical orientation at 120°).
It is generally known that Q waves are not always present in the lead III. The initial septal vector, oriented superiorly in such individuals, is the source of this Q wave. A Q wave in lead III is frequent in a normal heart when the electrical axis is horizontal.
Similarly, the existence of a Q3 and an inverted T3 may not indicate a myocardial infarction since a transverse posture might cause them.
Q Wave Abnormalities
Q waves represent the early phase of ventricular depolarization. If they are extremely broad (>0.2 seconds) or abnormally deep (>5 mm), they are pathogenic.
Pathologically deep but not broad Q waves are often indicative of ventricular hypertrophy. Myocardial infarction is indicated by Q waves that are both excessively deep and broad.
Anterolateral infarction with aberrant Q waves in leads I and aVL and precordial leads V4 to V6 is common in patients with an atypical origin of the left coronary artery from the pulmonary artery.
Q Waves And Myocardial Infarction
Normal conduction occurs when ventricular depolarization goes left to right through the septum and across both ventricles, with net forces directed towards the bigger left ventricle.
Posterior myocardial infarction does not create Q-waves on the 12-lead (unless inferior or lateral myocardial infarction accompanies i), but rather towering R waves in the anterior leads. "A QS complex in lead V1 is typical," says the Fourth Universal Definition of Myocardial Infarction.
If the frontal QRS axis is between 60 and 90 degrees, a Q-wave may be expected in aVL. Myocardial infarctions were formerly classified as Q-wave or non-Q-wave, with the former having permanent transmural necrosis.
However, additional Q-waves may appear as soon as one hour following the onset of ischemic symptoms and are related to bigger infarcts, worse EF, and increased mortality.
As a result, despite putative transmural and permanent cardiac damage, individuals detected with STEMI within 12 hours of symptom onset usually have positive effects following reperfusion.
Acute ischemia causes hyperacute T waves (compared to the previous QRS complex), which might assist in distinguishing fresh STE from old STE.
The most often misinterpreted type of ST elevation in ED patients with chest discomfort is old anterior QS waves with persistent ST elevation (LV aneurysm morphology).
ECG machines and STEMI criteria cannot distinguish the two, but previous medical history, symptom duration, prior ECG, and other ECG criteria may.
Q Waves And Heart Attack
Myocardial infarction (MI) is not necessarily accompanied by traditional chest discomfort. According to studies, 20-43% of all myocardial infarctions go undiagnosed, either because there are no symptoms (silent myocardial infarction) or because the symptoms are so faint or diffuse that neither the patient nor the practitioner considers the diagnosis.
Because published prevalences are based on the presence of pathogenic Q-waves in the electrocardiogram (ECG), they likely exclude a significant proportion of myocardial infarctions that do not (or just temporarily) present Q-waves in the ECG.
Previous cohort studies have shown mixed findings when comparing the long-term prognosis of these quiet or unrecognized myocardial infarctions to that of identified myocardial infarctions.
Some studies discover a comparable death rate, whereas othersfind prognoses for unreported or recognized myocardial infarctions. This disparity may be explained in part by huge disparities in baseline populations.
The discrepancy in the incidence of undetected myocardial infarctions might be attributed to variations in the electrocardiographic criteria utilized in cohort studies to diagnose previous myocardial infarctions.
This might also explain disparities in long-term prognosis since some studies with stricter ECG criteria would include only bigger myocardial infarctions than those with laxer ECG criteria.
However, since prior research utilized the ECG to evaluate whether or not there were symptoms of previous myocardial infarction, it is unknown if all electrocardiographic indicators of myocardial infarction are equally essential in termsof prognosis.
Furthermore, this information would be more attractive to the physician than the scholarly debate about whether a Q-wave reflects a previous myocardial infarction or not.
4. Q Wave Overview - ECG assessment and ECG interpretation made easy
People Also Ask
What Can Cause Q Waves?
A pathologic Q wave. Pathologic Q waves indicate a prior myocardial infarction. A lack of electrical activity causes them. A myocardial infarction may be seen as an electrical 'hole' since scar tissue is electrically dead, resulting in pathologic Q waves.
What Does An Abnormal Q Wave On ECG Mean?
Abnormal Q waves (AQW) on an ECG are often attributed to an underlying myocardial infarction. The effectiveness of AQW in diagnosing myocardial infarction as an inadequately specific indicator of myocardial infarction depends on its prevalence in the population examined.
What Do Abnormal Q Waves Indicate?
Q waves represent the early phase of ventricular depolarization. If they are extremely broad (>0.2 seconds) or abnormally deep (>5 mm), they are pathogenic. Pathologically deep but not broad Q waves are often indicative of ventricular hypertrophy.
What Are Q Waves?
A Q wave is an electrocardiogram (ECG) deflection of the QRS complex that is initially negative. A Q wave technically signifies that the net direction of early ventricular depolarization (QRS) electrical forces is pointing toward the negative pole of the lead axis.
Final Words
Q waves on an ECG are linked with an increased risk of heart disease and even death.
In the early stages of acute myocardial infarction, abnormal Q waves are common. There is no indication. However, abnormal Q waves are associated with a worse effect in terms of infarct size reduction after thrombolytic therapy.
Any Q-wave may suggest the necessity for additional examination and the implementation of appropriate medical and perhaps invasive or surgical therapy.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles