Necrotizing Fasciitis – Skin Infection Caused By A Bacterial Group
Necrotizing fasciitis is a serious, uncommon, and sometimes fatal soft tissue infection affecting the scrotum, perineum, the abdominal wall, or the extremities.
Author:Suleman ShahReviewer:Han JuJul 03, 202248 Shares1.1K Views
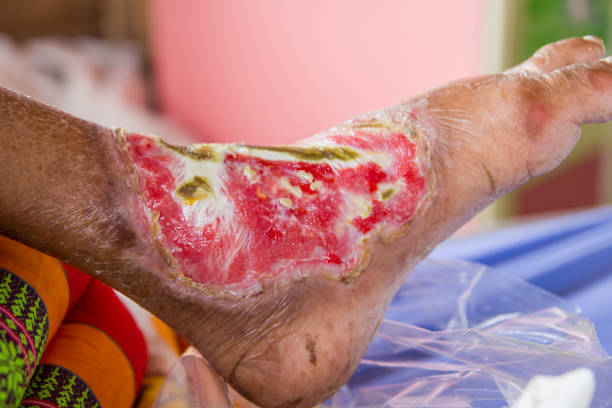
Necrotizing fasciitis(NF) is a serious, uncommon, and sometimes fatal soft tissue infection affecting the scrotum, perineum, the abdominal wall, or the extremities. Because the disease spreads quickly and septic shock might occur, the fatality rate is significant (median mortality 32.2 percent ).
Co-morbidities like diabetes, immunosuppression, chronic alcohol illness, chronic renal failure, and liver cirrhosis worsen the prognosis.
Based on microbiological discoveries, necrotizing fasciitis is categorized into four kinds. The majority of cases are polymicrobial, classified as type I.
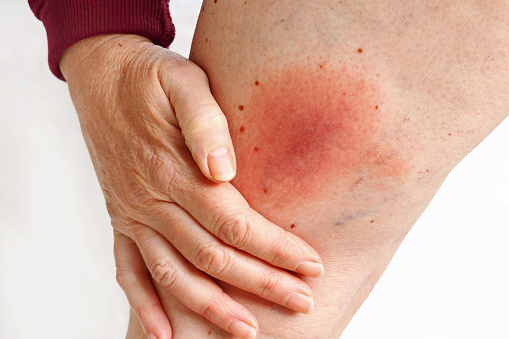
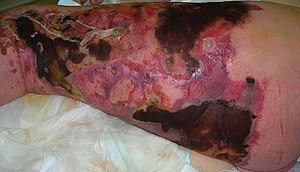
The patient's clinical condition ranges from erythema, edema, and soreness in the early stages of infection to skin ischemia with blisters and bullae in the latter stages.
The patient is severely unwell in its fulminant phase, with signs and symptoms of acute septic shock and extensive organ failure. The essential information for diagnosis is the clinical state.
What Is Necrotizing Fasciitis?
Necrotizing fasciitis (NF), often known as flesh-eating disease, is a bacterial illness that destroys soft tissue in the body. It is a severe illness with a fast start and rapid spread. In the afflicted region, extreme pain, fever, and vomiting are common symptoms in red or purple skin. The limbs and perineum are the most usually afflicted locations.
The infection usually enters the body via a breach in the skin, such as a cut or burn. Poor immunological function, such as diabetes or cancer, obesity, alcoholism, intravenous drug use, and peripheral vascular disease are also risk factors. It usually does not spread between individuals.
The sickness is categorized into four categories based on the organism that causes it. More than one species of bacteria is involved in between 55 and 80 percent of cases. Up to one-third of patients contain Methicillin-resistant Staphylococcus aureus (MRSA). Medical imaging is often used to confirm a diagnosis.
Handwashing and wound care may help to avoid necrotizing fasciitis. Surgery to remove the affected tissue and intravenous antibiotics are frequently used to treat it. A mixture of antibiotics, such as penicillin G, clindamycin, vancomycin, and gentamicin, is often utilized. Surgery delays are connected with a substantially increased risk of mortality. Despite high-quality care, mortality is between 25% and 35%.
Necrotizing fasciitis affects around 0.4 individuals per 100,000 in the United States and roughly 1 person per 100,000 in Western Europe each year.
Both sexes are equally impacted. It is more prevalent in elderly persons and uncommon in children. It has been described at least since Hippocrates' time. The term "necrotizing fasciitis" was coined in 1952.

Flesh Eating Bacteria (Necrotizing fasciitis)
Necrotizing Fasciitis Epidemiology
The yearly incidence of necrotizing fasciitis is estimated to be 500-1,000 cases yearly, with a worldwide frequency of 0.40 per 100,000 people. It seems to favor males, with a male-to-female ratio of 3:1; this ratio is mainly attributable to the greater prevalence of Fournier's gangrenein men. According to Anaya et al., infection of the lower extremities is the most prevalent location of necrotizing fasciitis (57, 8%), followed by the abdomen and the perineum.
Necrotizing Fasciitis Causes
Bacteria may enter the body through a cut, scrape, or surgical site. These wounds do not have to be severe for the bacteria to take hold. A needle puncture may be sufficient.
A variety of microorganisms causes necrotizing fasciitis. Group A Streptococcus is the most prevalent and well-known kind. This is not, however, the only kind of bacterium that may cause this illness. Aeromonas hydrophila, Clostridium, E. coli, Klebsiella, and Staphylococcus aureus are among the bacteria that may cause necrotizing fasciitis.
Necrotizing Fasciitis Diagnosis
Clinical Symptoms
The traditional trio of symptoms associated with necrotizing fasciitis is local discomfort, swelling, and erythema. Tenderness, sclerosis, skin necrosis, and hemorrhagic bullae may be seen at the infected location. The patient is severely sick in the fulminant stage of the illness, with signs and symptoms of acute septic shock, multiple organ failure syndromes, and widespread soft tissue necrosis. The subacute type of the illness has a sluggish clinical course that might last for days or weeks. The most recurring sign of early necrotizing fasciitis is pain that is not proportional to edema or erythema.
Once clinical indications arise, the look mimics the late stage of necrotizing fasciitis, with apparent bruises, bullae, and cutaneous necrosis owing to the necrotizing process's expansion—additional necrosis of the superficial fascia and fat results in crepitus and a thin watery malodorous discharge. Fournier's gangrene has a significantly distinct clinical history; it commonly starts with the perineum, scrotal skin discomfort, and itching.
Laboratory Tests
Typically, laboratory tests in this condition are not specific. Certain laboratory results may assist the doctor in distinguishing necrotizing fasciitis from other skin illnesses, such as necrotizing soft tissue infection. Leukocytosis is a frequent symptom of necrotizing fasciitis (NF), and a white blood cell count of more than 20,000/L is highly suggestive. Blood urea nitrogen levels more than 18 mg/dL and serum creatinine levels greater than 1.2 mg/dL indicate continuing renal failure, which is common in these individuals. This condition is distinguished by the presence of distinctive "dishwater pus," as well as a lack of bleeding and tissue resistance to blunt finger dissection.
Imaging Tests
Imaging studies may aid in diagnosing necrotizing fasciitis, particularly in equivocal instances. Although plain radiographyhas limited sensitivity and specificity, it may detect gas production in soft tissue, which is present in about half of all patients and strongly implies Clostridium species infection. CT and MRI scans are more sensitive and specific than conventional radiography. The degree of tissue infection, fascial edema, inflammation, and gas formation may all be shown by a CT scan. Although more accurate than CT, an MRI scan is not routinely utilized owing to expense.
Ultrasonographyis another viable alternative, giving essential information about the type and degree of infection, mainly when the diagnosis is ambiguous. The most crucial result in diagnosis is hyperechoic foci with reverberation artifact and filthy shadowing at the site of infection, reflecting subcutaneous gas. However, ultrasonography requires a highly experienced operator, limiting its usage in the ICU, where patients with necrotizing fasciitis are often treated.
Necrotizing Fasciitis Risk Factors
Nonsteroidal anti-inflammatory medicines (NSAIDs) or steroid treatments might reduce fever, making it challenging to diagnose necrotizing fasciitis. Diabetes mellitus affects 40 and 60 percent of people with necrotizing fasciitis. Cirrhosis of the liver, chronic heart failure, obesity, alcohol misuse, immunodeficiency, pre-existing hypertension, and peripheral vascular disease are all prevalent co-morbidities. Patients with concomitant illnesses are often classified as seriously sick and need long-term intensive care. Although somewhat disputed, old age is another risk factor for increased incidence and death.
Necrotizing Fasciitis Treatment
Using Antibiotic
Depending on its history, gram stain, and culture, a polymicrobial infection should be treated with antibiotics. Anaerobic coverage is critical for type 1 infection; effective antimicrobials include metronidazole, clindamycin, and carbapenems (imipenem). Antibiotics against S. pyogenes and S. aureus, which commonly coexist with the former, are used to treat type 2 illnesses.
As an initial empirical treatment, broad gram-negative coverage is required for newly treated patients. Clindamycin and penicillin, which cover Clostridium species, should be used to treat type 3 necrotizing fasciitis. If a Vibrio infection is detected, using tetracyclines and cephalosporins as soon as possible is critical for survival. Amphotericin B or fluoroconazoles may treat type 4 necrotizing fasciitis, although the outcomes are often poor. Intravenous immunoglobulin (IVIG) has been reported as a viable approach for neutralizing streptococcal toxins.
Surgery
Surgical intervention is life-saving and should be done as soon as feasible. In fulminant necrotizing fasciitis, a delay in treatment of more than 12 hours might be deadly. The significant features of surgical therapyinclude surgical debridement, necrosectomy, and fasciotomy. Necrotizing fasciitis patients should be thoroughly watched over the following 24 hours. A "second-look procedure" with severe surgical debridement is required for complicated surgical wounds.
The affected body location determines the amount of tissue taken metabolic needs are comparable to other severe traumas or burns. Necrotizing fasciitis of the abdominal wall needs particular attention. Serial dressing changes are required in the days after surgery. In situations of infection advancement, aggressive surgical debridement should be repeated.
In diffuse peritonitis, Hartmann's resection is regarded as the best option. A pressure sore, perineal abscess, or paraplegia are all common risk factors for infection spreading to the scrotum, inguinal area, and lower abdominal wall. An orchiectomy, cystostomy, or diverting colostomy is often necessary. Wide tissue incision, drastic debridement, and draining of the affected regions are all part of the surgical therapy. Despite the appearance of normal soft tissue, people with necrotizing fasciitis have widespread vascular microthromboses as well as vasculitis.
Amputation is often seen as a less invasive treatment with less blood loss than radical debridement. Patients with hypotension and shock benefit from amputation because they cannot tolerate subsequent lengthy surgeries.
Vacuum-Assisted Closure Device Therapy
Many surgeons have begun using vacuum-assisted closure (VAC) treatment for quick and successful wound closure. A vacuum-assisted closure device is made of a sterile, open-cell foam sponge inserted in the wound and sized to fit the wound. This is covered with a transparent adhesive drape to create an airtight atmosphere. Non-collapsible tubing connects the sponge to a portable vacuum pump. The pump makes constant negative pressure and is used to evacuate the sponge. Microstrain provided by the vacuum-assisted closure device enhances wound healing. Several randomized controlled trials have shown that full-thickness wounds treated with vacuum-assisted closure devices heal faster and have a lower wound surface area than standard gauze treatment.
Vacuum-assisted closure treatment provides various advantages in wound care, the most notable of which are wound area reduction and the creation of granulation tissue. Other benefits, including excellent wound cleansing and the removal of exudate, make vacuum-assisted closure a viable adjunct treatment for wound closure.
People Also Ask
How Do You Get Necrotizing Fasciitis?
You must have the bacteria in your body to have necrotizing fasciitis. This usually happens when the skin is broken. Bacteria, for example, may enter your body via a cut, scrape, or surgical site. These wounds do not have to be severe for the bacteria to take hold.
Where Is Necrotizing Fasciitis Most Commonly Found?
The extremities are the most prevalent body regions where necrotizing fasciitis occurs (arms, hands, feet, and legs). However, necrotizing fasciitis may also develop in the head, neck, and groin areas depending on the conditions and risk factors.
What Are The First Signs Of Necrosis?
Pain, warmth, skin redness, or swelling around a wound if the redness spreads quickly. Blisters on the skin, often with a "crackling" feeling under the skin. Pain from a skin wound combined with symptoms of a more severe illness, such as chills and fever. A grayish, odorous liquid is seeping from the incision.
How Do You Recognise Necrotizing Fasciitis?
Intense pain or loss of sensation around a cut or wound - the agony may seem to be much greater than you would anticipate from a cut or wound. Skin swelling surrounding the afflicted region. Flu-like symptoms include a high fever, headache, and fatigue.
Conclusion
Necrotizing fasciitis is an uncommon but deadly infection with a high mortality rate (median mortality 32.2%) that exceeds 100% without treatment. The diagnosis of necrotizing fasciitis is complex, as is the distinction between necrotizing fasciitis and other necrotizing soft tissue infections. Antibiotic therapy has a poor value in necrotizing fasciitis, and early forceful drainage and debridement are essential. The doctor should consider amputating the infected limb in necrotizing fasciitis of the extremities.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles