Traumatic Brain Injury - The Effect Of Markers In Inflammation
Traumatic brain injury (TBI) has been referred to for decades as a hidden epidemic. Between 1995 and 2001, it was responsible for at least 1.5 million emergency room visits and hospitalizations annually in the United States, a number that has undoubtedly escalated due to the conflicts in Iraq and Afghanistan.
Author:Suleman ShahReviewer:Han JuMay 29, 20234.6K Shares122.1K Views
Traumatic brain injury(TBI) has been referred to for decades as a hidden epidemic.
Between 1995 and 2001, it was responsible for at least 1.5 million emergency room visits and hospitalizations annually in the United States, a number that has undoubtedly escalated due to the conflicts in Iraq and Afghanistan.
Many survivors of traumatic brain injuries are left with permanent disability, and even mild traumatic brain injuries can result in cognitive deficits, concentration difficulties, exhaustion, and headaches.
It primarily affects young men, but is also becoming increasingly prevalent among the elderly.
Currently, monitoring and maintenance of normal intracranial pressure (ICP) and cerebral perfusion pressure are the primary focuses of TBI patient care (CPP).
One of the repercussions of an increased ICP is a decrease in CPP, which leads to secondary ischemia.
Therefore, it is not surprising that a high ICP has been associated with death and poor outcome in TBI patients.
What Exactly Is Traumatic Brain Injury?
Traumatic Brain Injury (TBI) disrupts the normal function of the brain and can be caused by a blow, bump, or jolt to the head, or when an object pierces the skull and enters brain tissue. Observing one of these clinical signs alters brain function:
- Change in mental state, such as confusion, sluggish thinking, or trouble focusing.
- Focal neurological deficits include muscle weakness, vision loss, and speech changes.
- Amnesia or the loss of memory for things that happened before or after the event.
- Consciousness is lost or weakened.
Depending on brain damage, TBI symptoms can be mild, moderate, or severe. In mild cases, mental state or consciousness may briefly change. Severe cases can cause unconsciousness, coma, or death.

Traumatic Brain Injury Symptoms
The Types Of Traumatic Brain Injuries
Mass lesions, like hematomas and contusions, increase brain pressure after a TBI. Traumatic brain injury effects include:
- Linear or simple skull fractures, or "cracks," may accompany TBIs. Possible skull fracture forces may injure the brain. When evaluating a patient, skull fractures might be frightening. Base-of-the-skull fractures can damage nerves, arteries, and other structures. If the fracture enters the sinuses, CSF may flow out of the nose or ears. Depressed skull fractures push on the brain.
- Ischemia is another kind of widespread brain damage. Many TBI patients experience poor blood supply. A brain that has just been injured is highly vulnerable to blood flow decreases. Blood pressure changes might be harmful after a head injury.
- Axonal damage causes decreased function and eventual axonal loss. Nerve cells interact via lengthy extensions. If enough axons are damaged, nerve cells' capacity to communicate and integrate their functions may be lost or compromised, leaving a patient with significant disability.
- TBIs can cause minute alterations throughout the brain that aren't seen on CT scans. Diffuse brain injuries can occur with or without a mass lesion.
- Subarachnoid hemorrhage (SAH) is subarachnoid bleeding. It emerges as diffuse cerebral blood following TBI. Most head trauma-related SAHs are minor. SAH can cause hydrocephalus.
- Intracerebral hemorrhage (ICH) involves bleeding within the brain and may be related to other brain traumas, especially contusions. Size and location influence whether a hemorrhage can be surgically removed.
- Brain contusions are bruises. Cerebral contusions look like bruises under a microscope. An injured or enlarged brain combined with blood from arteries, veins, or capillaries. Contusions usually occur around the base of the frontal lobe but can occur anywhere.
- Hematomas are blood clots in or on the brain. Brain hemorrhages can form anywhere. Epidural hematomas are blood collections between the dura mater and the skull. Subdural hematomas are blood collections between the brain's dura mater and arachnoid layer.
The Development Of Biomarkers In TBI
S100B, neuron-specific enolase (NSE), and myelin basic protein (MBP) reflect tissue injury and have predictive value. S100B has been linked with initial brain injury severity (GCS), brain damage size (on CT/MRI scans), and neurological outcome (Glasgow Outcome Scale/Extended; GOSE) in various observational clinical TBI studies. Biomarkers have only recently been used in clinical studies with prospective data collection, outcomes, and intervention efficacy assessment. The goal is to show links between neuroprotection and biomarker reduction in TBI patients. Biomarkers are a more sensitive early measure of outcome than 6 month neurological scores. Due to limited patient numbers in TBI clinical trials, biomarkers could provide a more robust tool to discover outcome differences in TBI patient populations.
The most researched TBI biomarker is S100B, a low-molecular-weight calcium-binding astrocyte protein. S100B's validity as a TBI biomarker hinges on its constitutively low serum and CSF expression, which are rapidly released after brain injury. High S100B expression is linked to injury severity and a negative prognosis. S100B isn't suitable as a TBI biomarker since it doesn't cross the BBB, its serum levels increase after peripheral damage without brain injury, and it doesn't always predict prognosis. In the hunt for a TBI biomarker, numerous molecules have been evaluated, including GFAP, NSE, MBP, II-spectrin breakdown products (BDPs), ubiquitin C-terminal hydrolase-L1, and different cytokines.
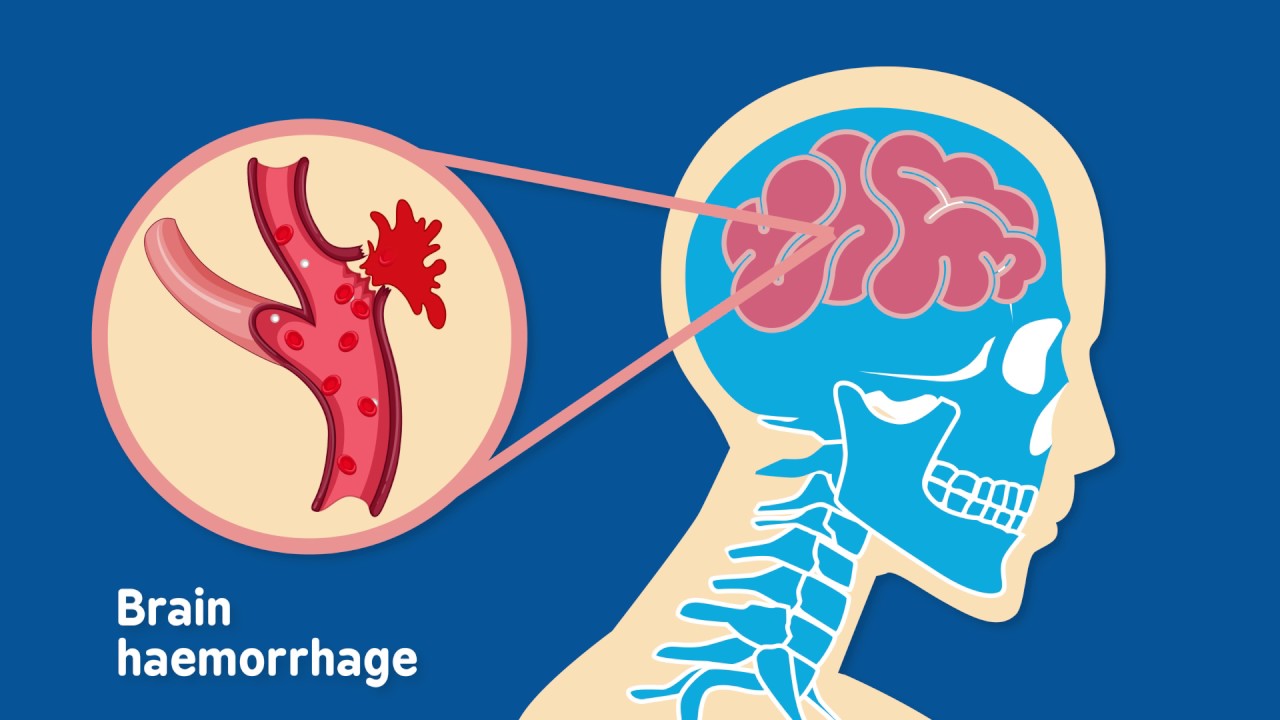
What is a head injury?
The Potential Of Inflammatory Cytokines As Biomarkers Of TBI
Pro and anti-inflammatory cytokines modulate the inflammatory response to TBI. Leukocytes and glial cells generate cytokines. They're soon quarantined after TBI. Many overlapping cytokines constitute a complicated network of inflammatory mediators. Pro-inflammatory cytokines promote inflammation, while anti-inflammatory cytokines reduce it. The expression profile of each cytokine after brain injury can be evaluated to determine the level of tissue damage. Cytokine concentrations vary by tissue or fluid (brain tissue, CSF blood, serum, plasma, etc.), and the temporal profile of the cerebral immune response in rodent versus human data can show variances and similarities. Below are some of the most investigated cytokines for brain injury and biomarkers.
The Tumor Necrosis Factor
TNF (formerly TNFα) is a multifunctional cytokine produced by microglia and astrocytes. Early research in rat models of TBI revealed that TNF overexpression is harmful. Recent work using TNF and TNF receptor deletion mice shows increased mortality and worse long-term healing in localized TBI models. These seemingly contradictory facts show TNF's dual role as a pro and anti-inflammatory cytokine.
Interleukin-10
Interleukin-10 is thought to be predominantly an anti-inflammatory cytokine since it has a strong inhibitory effect on the production of a variety of pro-inflammatory mediators, such as IL-1β and TNF, but also IL-1α, GM-CSF, IL-6, IL-8, IL-12, and IL-18. Its most crucial action is the suppression of IL-1β and TNF since these cytokines are recognized to be crucial in the beginning and spreading of the inflammatory response. Indeed, IL-10 treatment after LFP injury in rats leads to better results and lower levels of IL-1β and TNF in the brain tissues.
Interleukin-6
Interleukin-6 has been studied a lot, and scientists have found that it is involved in a lot of normal and unhealthy bodily processes. It is known that IL-6 controls inflammation, immunity, bone metabolism, hematopoiesis, and the development of nerve cells. IL-6 has also been linked to aging, osteoporosis, autoimmune diseases, Alzheimer's disease, and injuries to the brain. Even though IL-6 is not only found in the CNS, it is significantly upregulated after a brain injury.
Interleukin-8/CXCL8 And Monocyte Chemoattractant Protein/CCL2
Interleukin-8 (CXCL8) is a CXC chemokine that is made by glial cells, macrophages, and endothelial cells. It is a key part of how neutrophils get activated and move toward chemicals. Early studies showed that cytokines like IL-1β and TNF cause astrocytes to release IL-8. Both IL-1β and TNF are released soon after a brain injury. Increased IL-8 expression has been linked to many types of cancer, bacterial infections, and heart disease.
The monocyte chemoattractant protein-1 (MCP-1) or CCL2 is made by astrocytes within hours of an injury. The number of recruited macrophages is related to the amount of MCP-1 or CCL2 (Semple et al., 2010c). Since MCP-1 is controlled in an autocrine way, the release of MCP-1 by macrophages and microglia that have moved into the damaged brain keeps cells moving there. In models of brain injury, stroke, and multiple sclerosis, removing MCP-1 reduced the number of macrophages that came into the brain and the damage to the nervous system.
Other Markers Of Inflammation
Besides cytokines, there are a few other molecules that might be useful as biomarkers of brain injury. For example, IL-6 controls how much GFAP is made by turning on the JAK/STAT pathway. It is well known that after TBI, GFAP expression goes up in serum. Serum GFAP levels have been shown to be able to predict death and outcome in people who have had a severe TBI. More recently, it has been found that GFAP-BDPs in the serum of patients with mild and moderate TBI within 4 hours of the injury correlate with injury severity (GCS) and may be linked to CT lesions. In a recent study, it was found that by combining measurements of GFAP in CSF and serum with the IMPACT Outcome Calculator, it was possible to get a much better idea of what would happen. Also, the expression of II-spectrin breakdown product 145 (SBDP145) was measured in the cerebrospinal fluid (CSF) and showed a strong correlation with death at 6 months.
People Also Ask
What Defines A Traumatic Brain Injury?
A traumatic brain injury (TBI) is a type of acquired brain injury that happens when the brain is hurt by a sudden blow or blows to the head. TBIs can happen when the head suddenly hits an object hard or when an object goes through the skull and hurts brain tissue.
What Are Three Causes Of Traumatic Brain Injury?
People usually get TBIs from a fall, an injury from a gun, a car accident, or an attack. Research shows that almost half of the hospitalizations for TBI are caused by falls. In the United States, most people who die from TBI do so because they kill themselves with a gun.
What Is The Most Common Type Of Traumatic Brain Injury?
One of the most common types of TBI is a concussion. A concussion can happen when the head or body is moved back and forth quickly, like in a car accident or sports injury, or when the head is hit hard. Concussions are usually not life-threatening, so they are often called "mild TBIs."
Can You Recover From Traumatic Brain Injury?
For those who have suffered a moderate TBI, the majority of their brain function can be restored, but further treatments such as neurosurgery, o/p therapy, speech/language therapy, psychotherapy, and/or social services may be required.
Conclusion
Brain injury biomarkers have the potential to improve how patients are diagnosed, treated, and what happens to them. They could also help come up with new treatments. The now-well-known inflammatory response that happens when the brain is hurt could give doctors a number of markers that tell them specific things about the injury. Experiments with animal models of traumatic brain injury have shown that the brain makes a lot of inflammatory mediators after an injury. Many of these change their expression quickly, reaching peaks that are over a thousand times higher than their normal levels within hours of being hurt. The amount, timing, and length of time that these mediators are active may be able to tell us not only about the injury, but also about how complicated it is when multiple injuries happen at the same time.
Jump to
What Exactly Is Traumatic Brain Injury?
The Types Of Traumatic Brain Injuries
The Development Of Biomarkers In TBI
The Potential Of Inflammatory Cytokines As Biomarkers Of TBI
The Tumor Necrosis Factor
Interleukin-10
Interleukin-6
Interleukin-8/CXCL8 And Monocyte Chemoattractant Protein/CCL2
Other Markers Of Inflammation
People Also Ask
Conclusion

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles
