Cardiovascular Disease - The Effects And Benefits Of Exercise
The greatest cause of illness and death globally is cardiovascular disease (CVD). Cardiovascular disease accounts for 600,000 fatalities (25%) in the United States each year, and after a steady drop over the previous five decades, its prevalence is rising again. We now know that a sedentary lifestyle, which is marked by low levels of physical activity that don't change, is one of the main risk factors for cardiovascular disease (CVD) that leads to poor health.
Author:Suleman ShahReviewer:Han JuMay 31, 20239.3K Shares389K Views
The greatest cause of illness and death globally is cardiovascular disease(CVD). Cardiovascular disease accounts for 600,000 fatalities (25%) in the United States each year, and after a steady drop over the previous five decades, its prevalence is rising again.
We now know that a sedentary lifestyle, which is marked by low levels of physical activity that don't change, is one of the main risk factors for cardiovascular disease (CVD) that leads to poor health.
On the other hand, regular exercise and physical activity are linked to a wide range of health benefits and a much lower risk of CVD.
Several long-term studies have shown that being more active is linked to a lower death rate from all causes and may slightly increase lifeexpectancy. This effect is closely linked to a lower chance of getting heart and lung diseases.
Death rates for both men and women have been shown to be inversely related to cardiorespiratory fitness, even when other factors like smoking, high blood pressure, and high cholesterol are also present.
Also, both men and women who exercise more may be able to partially reverse the increased risk of death from all causes and CVD that comes with having a high BMI.
Recent research from cardiovascular cohorts demonstrates that continuous physical exercise is related to a more favorable inflammatory marker profile, lowers the incidence of heart failure, and increases survival in people with coronary artery disease after 30 years of follow-up.
Plasma Lipids And Atherogenesis
Given that plasma lipids are significant CVD risk factors, several studies have explored whether regular physical exercise might cut CVD risk by modifying circulating lipoproteins. According to these studies, endurance exercise raises HDL and lowers triglycerides. Both of these things lower the risk of coronary heart disease.
The effects of physical activity on plasma lipids are diverse and vary in type, intensity, duration, and nutrition. Early research on exercise's impact on LDL levels did not evaluate dose-dependence.
A study of subjects with mild to moderate dyslipidemia found a dose-dependent effect of exercise on plasma levels of low density lipoprotein (LDL), triglycerides, and large particle very low density lipoprotein (VLDL).
Increasing activity levels throughout time increased HDL levels from baseline (pre-exercise routine). Recent research shows that several drug treatments that raise HDL levels in the blood do not reduce the risk of CVD.
The size of HDL particles is a major factor in how ABCA1 exports cholesterol, which suggests that it may be a risk factor for CVD.
Rather than HDL levels, exercise training may protect against CVD by increasing LDL and HDL particle size and decreasing VLDL particle size.
A recent study investigating the dose-dependent effects of exercise on cholesterol efflux in 2 randomized trials consisting of six distinct exercise doses reported a significant increase in HDL cholesterol and efflux capacity with exercise, though only in the high amount/high intensity intervention groups.
Even though exercise alters the plasma lipid profile and increases HDL concentration and particle size, moderate exercise may have limited effects on HDL functionality, and the contribution of changes in plasma lipoprotein concentration, structure, and function to overall CVD risk reduction by exercise is unclear.
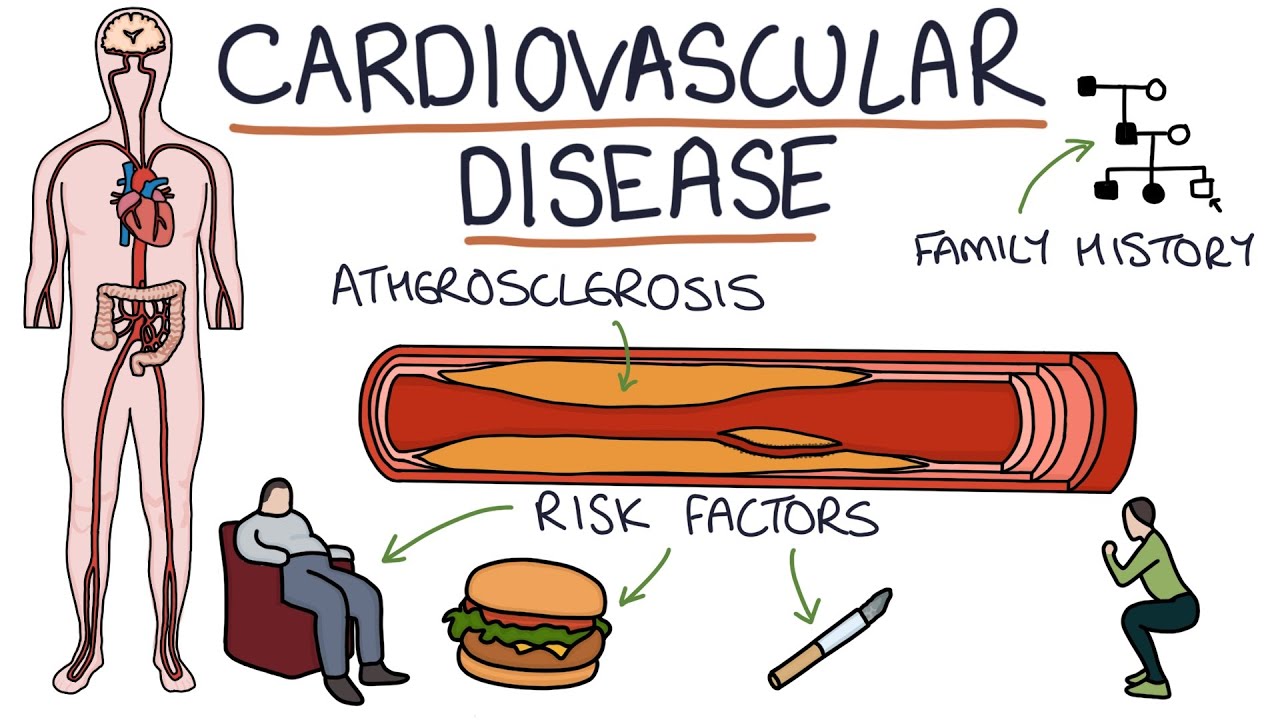
Understanding Cardiovascular Disease: Visual Explanation for Students
Insulin Sensitivity
Insulin sensitivity changes how blood lipids affect heart health, while insulin resistance causes heart disease by changing how blood lipids work.
Insulin resistance in adipocytes reduces glucose absorption, causing the liver to produce and release more triglycerides and VLDL.
Due to an increase in the activity of cholesteryl ester transfer protein (CETP) and the transfer of HDL cholesteryl esters to triglyceride-rich lipoproteins, insulin resistance causes HDL to drop. This prevents cholesterol from leaving the artery walls and speeds up the formation of atherosclerotic plaque.
Insulin signalingstimulates Akt-dependent phosphorylation and activation of eNOS, which generates NO. Ras-RAF-MAPK pathway activation boosts cell proliferation and differentiation and increases endothelin-1 synthesis (ET-1).
With compensatory hyperinsulinemia, selective inhibition of the PI3K-Akt-eNOS pathway leads to unmasking and stimulation of the MAPK-mediated production of endothelin-1 (ET-1) and vascular smooth muscle proliferation. This may contribute to the development of atherosclerotic plaques and peripheral artery disease.
Enhanced endothelial synthesis and release of ET-1, combined with increased sympathetic activity, may contribute to vasoconstriction of small diameter arteries and arterioles in insulin-resistant states, raising systemic vascular resistance to blood flow and arterial blood pressure.
High blood glucose levels also encourage the production of advanced glycation end products (AGEs), which are proteins and lipids that have been non-enzymatically glycated and oxidized. This leads to cross-linking of collagen and elastin fibers and loss of vascular flexibility, which is another way of saying that the arteries get stiffer.
Exercise training improves insulin sensitivity and glycemic control in insulin-dependent and non-insulin-dependent diabetes.
Even one low-intensity (50% VO2 max, 350 kcal) workout improves insulin sensitivity and fatty acid intake the next day.
Animal studies show that exercise may make adipose tissue, skeletal muscle, and endothelium more sensitive to insulin. This makes systemic insulin resistance, which is a part of type 2 diabetes, worse.
Inconsistent results across species and exercise protocols have hampered our understanding of the exact cellular and molecular mechanisms involved in the enhancement of insulin signaling following exercise.
But it looks like exercise conditioning is linked to adaptive changes in the expression or regulation of one or more parts of the insulin receptor/insulin receptor substrate (IRS)/PI3K/Akt signaling cascade.
During exercise, insulin levels are somewhat lowered and contracting muscle increases glucose absorption through insulin-independent sarcolemmal translocation of GLUT4 glucose transporters. Eccentric exercise-induced muscle damage may result in insulin resistance via TNF-α-mediated PI3K decreases.
Further study is needed to understand how various exercise regimes might generate tissue-specific changes in insulin signaling and how these pathways may be targeted to cure insulin-resistance and diabetes-related cardiovascular problems.
Blood Pressure
During exercise, increases in cardiac stroke volume and heart rate boost cardiac output, which raises mean arterial blood pressure. Long-term activity reduces resting blood pressure. Regular moderate-to-hard exercise 3–5 times per week decreases blood pressure by 3.4/2.4 mmHg, according to a meta-analysis.
Even a 1 mmHg drop in systolic BP reduces heart failure occurrences by 20.3 (blacks) or 13.3 (whites) per 100,000 person-years. Thus, lowering blood pressure with exercise, nutrition, and weight loss might reduce CVD incidence.
Chronic aerobic and resistance exercise reduce systemic vascular resistance, which lowers ambulatory blood pressure. Shear forces and metabolites made by active skeletal muscle during exercise widen blood vessels by relaxing smooth muscle cells in the blood vessels.
Reduced eNOS activity owing to age or NOS3 polymorphism has been linked to hypertension. Long-term exercise training makes hypertensive people make more eNOS and nitric oxide (NO), which lowers their blood pressure.
The results show that rats with high blood pressure caused by chronic NOS suppression who swam for 6 weeks had much more eNOS protein expression and better vasodilation caused by acetylcholine.
After exercise training, the endothelium-dependent vasodilation seems to get better, which may lower blood pressure and vascular resistance at rest.
Mayo Clinic Minute: What is heart disease?
In addition to NO-mediated reductions in resistance vascular tone, exercise may also lower blood pressure through adaptive reductions in sympathetic nerve activity, prevention or reversal of arterial stiffening, and suppression of inflammation, though the effects may be different for different groups (e.g., at-risk adults vs. healthy adults).
As with changes in the blood lipid profile, it's uncertain if exercise's blood pressure-lowering benefits can explain its positive effects on CVD risk and death.
Cardiac Adaptations
During exercise, the heart experiences occasional pressure, volume, or both overloads. To regulate stress and fulfill the systemic demand for more blood, the heart adapts to repeated exercise by expanding its mass, mostly through ventricular chamber wall thickening.
This heart enlargement is caused by larger terminally differentiated cardiac myocytes. Adaptive remodeling of the heart during exercise preserves or improves contractile performance.
This is different from pathologic remodeling caused by chronic pressure overload, like high blood pressure or aortic stenosis, which can lead to heart failure.
Recent studies in animal exercise models have found cellular and molecular changes in the heart's physiologic development program during exercise training. Pathologic cardiac remodeling decreases oxidative energy production through fatty acid oxidation and increases glucose consumption, but exercise increases both mitochondrial biogenesis and fatty acid oxidation.
Recent research reveals that myocardial glycolytic activity variations during acute exercise and recovery might regulate metabolic gene expression and heart remodeling. Studies have shown that IGF-1 and insulin receptors play the most important role in signaling through the PI3K/Akt1 pathway, which leads to protein synthesis and muscle growth.
Untargeted techniques have uncovered additional transcriptional drivers of exercise-induced hypertrophy. Exercise reduces the negative regulation of CCAAT-enhancer binding protein β (C/EBPβ) by CBP/p300-interactive transactivator with ED-rich carboxy-terminal domain-4 (Cited4).
Exercise-induced cardiac hypertrophy needs Cited4 to be turned on, and cardiac-specific overexpression of the gene makes the heart bigger and protects it from damage caused by ischemia and reperfusion.
Some signaling pathways that are used during exercise-induced growth programs may work directly against proteins like NFATc2 that promote pathological remodeling.
Blood And Vasculature
Blood oxygen carrying capacity, determined by circulating erythrocytes and intracellular hemoglobin concentration, affects exercise performance and fatigue resistance. Athletes with a lot of endurance often have "athlete's anemia" because they lose erythrocytes or have a low hematocrit because their plasma volume has grown.
Total erythrocyte mass is higher in high-altitude athletes. Oxygen O2) dose-dependently affects hypoxia-inducible factor (HIF)-mediated erythropoietin synthesis and upregulates erythropoietin receptors, iron transporters, and transferrins. Multiple studies show exercise boosts hematopoiesis.
Intense activity releases stress and inflammatory substances acting on the bone marrow, such as cortisol, IL-6, TNF-α, PMN elastase, and granulocyte colony stimulating factor.
One study indicated that circulating CD34+ hematopoietic progenitor cell counts were 3 to 4-fold greater in runners compared to non-runners at baseline, which may improve tissue repair.
Further investigation demonstrated that strenuous exercise released CD34+/KDR+ endothelial progenitor cells from the bone marrow. This effect was heightened in people with higher LDL/HDL and LDL/TC ratios.
Within hours after resistance training, women had a substantial rise in circulating EPCs, VEGF, HIF-1α, and EPO.
Since the effects of exercise on angiogenesis and wound healing have not been studied in depth, no one knows what these reactions mean for the body.
People Also Ask
Can Cardiovascular Disease Be Cured?
Even though coronary heart disease cannot be cured, medication may help control the symptoms and lower the risk of complications like heart attacks. Alterations to the patient's lifestyle, such as beginning an exercise routine and giving up smoking, may be part of the treatment.
How Long Can You Live With Cardiovascular Disease?
Women who have heart disease tend to live longer than men who have the same condition. With heart disease, the average life expectancy for a woman at age 50 is 7.9 years, while for a man it is 6.7 years. Compared to men, women usually get heart disease three years later and heart attacks four and a half years later, on average.
What Are The Top Three Types Of Cardiovascular Disease?
- Coronary heart disease – a condition that affects the blood vessels that feed the heart muscle with blood.
- Cerebrovascular disease – a condition that affects the veins and arteries that feed the brain.
- Peripheral arterial disease – a condition in which the blood arteries that feed the arms and legs become diseased.
What Are The Top Ten Cardiovascular Diseases?
- Abnormal heart rhythms, or arrhythmias.
- Aorta disease and Marfan syndrome.
- Congenital heart disease.
- Coronary artery disease (narrowing of the arteries).
- Deep vein thrombosisand pulmonary embolism.
- Heart attack.
- Heart failure.
- Heart muscle disease (cardiomyopathy).
Conclusion
Despite overwhelming evidence of exercise's health advantages, most Americans are inactive. Regular exercise, even short bursts, lowers the risk of dying, and 50–60 minutes of vigorous activity every day is best.
How much exercise is ideal for cardiovascular health? Studies show that the number of bad cardiovascular events in marathoners is the same as in a group of people with CHD. This suggests that too much exercise may be bad for you.
A recent study found that those who ran at least 25 marathons over 25 years had greater levels of coronary artery calcification (CAC) and calcified coronary plaque volume than inactive people.
A recent study also showed that physically active people (~3 times the recommended levels) are more likely to acquire CAC, especially white guys.
Other studies show that exercisers have more stable plaques due to calcification. This shows that even though they have more plaques and normal CAC scores, higher levels of physical activity may improve plaque quality to lower the risk of cardiovascular events.
As with other exercise effects, the dose-response curve is unclear, and it is unclear at what intensity and duration the benefits of exercise begin to decrease and become harmful. We don't know how age, gender, race, and the risk of cardiovascular disease at the start affect this benefit-to-harm threshold.

Suleman Shah
Author
Suleman Shah is a researcher and freelance writer. As a researcher, he has worked with MNS University of Agriculture, Multan (Pakistan) and Texas A & M University (USA). He regularly writes science articles and blogs for science news website immersse.com and open access publishers OA Publishing London and Scientific Times. He loves to keep himself updated on scientific developments and convert these developments into everyday language to update the readers about the developments in the scientific era. His primary research focus is Plant sciences, and he contributed to this field by publishing his research in scientific journals and presenting his work at many Conferences.
Shah graduated from the University of Agriculture Faisalabad (Pakistan) and started his professional carrier with Jaffer Agro Services and later with the Agriculture Department of the Government of Pakistan. His research interest compelled and attracted him to proceed with his carrier in Plant sciences research. So, he started his Ph.D. in Soil Science at MNS University of Agriculture Multan (Pakistan). Later, he started working as a visiting scholar with Texas A&M University (USA).
Shah’s experience with big Open Excess publishers like Springers, Frontiers, MDPI, etc., testified to his belief in Open Access as a barrier-removing mechanism between researchers and the readers of their research. Shah believes that Open Access is revolutionizing the publication process and benefitting research in all fields.

Han Ju
Reviewer
Hello! I'm Han Ju, the heart behind World Wide Journals. My life is a unique tapestry woven from the threads of news, spirituality, and science, enriched by melodies from my guitar. Raised amidst tales of the ancient and the arcane, I developed a keen eye for the stories that truly matter. Through my work, I seek to bridge the seen with the unseen, marrying the rigor of science with the depth of spirituality.
Each article at World Wide Journals is a piece of this ongoing quest, blending analysis with personal reflection. Whether exploring quantum frontiers or strumming chords under the stars, my aim is to inspire and provoke thought, inviting you into a world where every discovery is a note in the grand symphony of existence.
Welcome aboard this journey of insight and exploration, where curiosity leads and music guides.
Latest Articles
Popular Articles